Key Takeaways
Hello Heart Hero. If your Apple Watch, Fitbit, Kardia, or Samsung device showed a rhythm strip and a phrase like “possible AV block” or “PR prolongation,” it makes sense if your stomach dropped a little. A short alert can feel huge when it is about your heart.
Wearable users are not asking for perfect textbook cardiology. They want clear answers. What part of my heart is this talking about? Is this dangerous? Did my coffee, medication, or bad watch contact mess up the reading? Should I relax, monitor, or get help now?
The av node sits right in the middle of those questions. It is small, but it has a big job. When you understand what it does, your ECG stops looking like random spikes and starts telling a story you can follow.
An Introduction to Your Hearts Electrical Gatekeeper
Your heart runs on electricity before it pumps with muscle. A signal starts in the upper chambers, moves through the middle, and then tells the lower chambers when to squeeze. The av node is the checkpoint in that pathway.
For many people, confusion starts here. A watch may flag a rhythm issue, but it seldom explains the “why” in plain language. That is why learning a little about the electrical system can calm a lot of fear.
If you want a bigger picture of how rhythm specialists think about these signals, this overview of cardiac electrophysiology is a helpful companion.
Why this tiny structure matters
The av node acts like a smart gatekeeper between the top and bottom chambers of the heart. It does not pass signals along. It controls timing.
That timing matters because the top chambers need a moment to finish pushing blood into the bottom chambers before the lower chambers contract. If the signal rushed through too quickly, the squeeze would be less coordinated.
A lot of wearable anxiety comes from seeing an alert without context. One device notice can sound dramatic, when the pattern is mild, temporary, or not real. Knowing what the av node does gives you a steadier way to read your own data.
Key takeaway: A watch alert is not a diagnosis by itself. It is a clue. Understanding the av node helps you tell the difference between a clue that needs follow-up and a clue that may need a cleaner recording or trend tracking.
What you are really looking for
When wearable users monitor the av node, they are trying to answer one of three questions:
- Is the signal a little slow? This often shows up as a longer PR interval.
- Are some signals getting through inconsistently? That can suggest a form of AV block.
- Is the node filtering a fast rhythm above it? This can happen during atrial fibrillation or AVNRT.
You do not need to memorize every rhythm name today. You need a basic map. Once you have that, the rest gets less intimidating.
What Is the AV Node and Its Function
The av node is a tiny cluster of specialized cells in the heart. It sits in Koch’s triangle near the lower back part of the wall between the upper chambers. It is about 1 x 3 x 5 millimeters, but it creates a delay of about 0.09 seconds, and it can act as a backup pacemaker at 40 to 60 beats per minute if needed, according to this AV node overview.
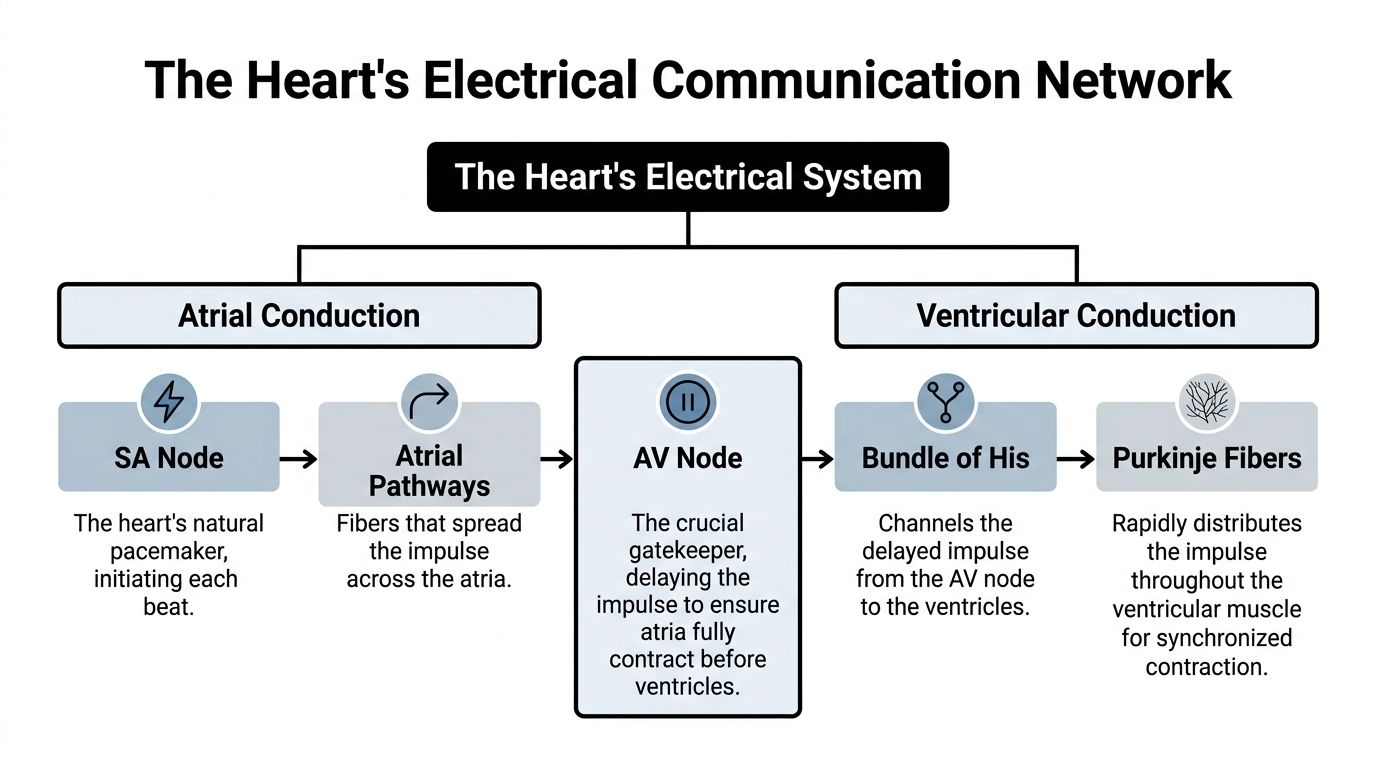
A guarded doorway analogy
A simple way to picture the av node is a doorway with a careful security guard.
The upper chambers of the heart send the “go” signal first. The av node pauses that message for a moment before letting it pass into the lower chambers. That pause is not a flaw. It is the design.
If the top and bottom chambers fired at the same time, the heart would lose that smooth handoff that makes pumping efficient. The av node protects that sequence.
Why a delay is healthy
People often hear the word “delay” and assume something is wrong. In this case, a delay is exactly what you want.
The atria contract first. Then the ventricles contract. The av node creates the handoff that keeps those two events in order.
That is why the av node is often called an electrical gatekeeper. It keeps the traffic organized rather than moving everything through as fast as possible.
It also has a backup role
Another reassuring fact is that the av node is not a checkpoint alone. It also has its own slower built-in rhythm.
If signals from above fail, the av node can help keep the ventricles beating at its baseline rate. That rate is slower than the heart’s usual primary pacemaker, but it is part of the body’s backup plan.
For an anxious reader, this matters. The heart has layers of protection. The conduction system is not fragile in the way many people fear after seeing one odd watch strip.
Helpful way to remember it: The SA node starts the beat, the av node times the handoff, and the ventricles deliver the main squeeze.
Where people get mixed up
Many wearable users confuse the av node with the whole electrical system. It is one part, but it is an important middle part.
A watch reading tied to the av node is about timing. It is asking whether the signal is getting from the top chambers to the bottom chambers normally, too slowly, inconsistently, or in a way that helps create a rapid rhythm.
That timing question is what you see on ECG as the PR interval, which is why that interval matters so much on watch tracings.

Reading Your AV Node on a Watch ECG
When your watch records a single-lead ECG, you are not seeing the av node directly. You are seeing its effect on timing. The main clue is the PR interval.
Find the P wave and the QRS
Start with the broad pattern:
- The P wave shows the upper chambers activating.
- The QRS complex shows the lower chambers activating.
- The PR interval is the span from the start of the P wave to the start of the QRS.
A normal PR interval is 120 to 200 milliseconds, as noted in this PR interval explanation. On a wearable ECG, that interval is your most practical window into av node conduction.
If your tracing is noisy, do not force an interpretation. Motion, dry skin, loose contact, and muscle tension can distort small waves. The P wave is often the first thing to become hard to see.
What a normal PR interval means
A normal PR interval means the signal is traveling from the atria through the av node and onward to the ventricles in a steady, efficient way.
That does not mean every normal-looking strip rules out all rhythm issues. It means this specific handoff appears to be within the expected range on that recording.
This is why one clean baseline ECG can be so useful. Once you know your usual pattern, changes become easier to spot.
Why rhythm can look irregular during fast atrial activity
The av node does more than delay. It also filters.
The node has a fast pathway and a slow pathway, and that helps explain why a fast atrial rhythm like atrial fibrillation, with atrial rates over 400 bpm, does not send every impulse to the ventricles. Instead, the ventricles often respond in a slower irregular range of 100 to 180 bpm, as described in this dual-pathway AV nodal modeling paper.
On a wearable ECG, that can look messy and uneven. The confusing part is that the watch may tell you the rhythm is irregular but not explain that the av node is acting like a filter in the middle.
Tip: If your watch strip looks irregularly irregular and the beats below are not racing as fast as the atria would be, that filtering effect may be part of the story.
A simple way to look at your own strips
When you review your recordings, ask:
- Can I see a P wave before each QRS?
- Does the PR interval look fairly consistent?
- Is the tracing clean enough to trust what I am seeing?
If the answer to the third question is no, repeat the ECG before panicking. A better recording often answers the question more clearly than a lot of guessing.
Understanding Different Types of AV Block
The phrase AV block sounds scary. It helps to translate it into plain language. AV block means the electrical signal is having trouble getting through the av node area on time, or getting through at all.
One useful analogy is a traffic light between the upper and lower chambers. Sometimes the light is slow. Sometimes it skips cars. Sometimes nothing gets through.
First-degree AV block
This is the long yellow light.
The signal still gets through every time, but it moves more slowly than expected. The av node’s conduction delay averages 40 ms and contributes to a normal PR interval of 120 to 200 ms. A first-degree AV block is diagnosed when the PR interval exceeds 200 ms, according to Kenhub’s AV node review.

On a wearable ECG, this may show up as a consistently prolonged PR interval. Many people feel nothing at all.
That is where a lot of unnecessary fear starts. A first-degree block is often a timing issue, not a dramatic failure of the heart. Context matters, especially symptoms, medications, and whether the pattern is stable over time.
Second-degree AV block
This is the traffic light that sometimes fails to let a car through.
Some electrical signals make it to the ventricles, and some do not. One common form is Mobitz I, also called Wenckebach, where the PR interval gets longer and longer until a beat drops.

For wearable users, this pattern can be hard to catch and harder to interpret. If you want to see how this looks in plain language on a watch tracing, this guide to second-degree AV block type 1 on a watch ECG can help.
A person might notice skipped beats, brief lightheadedness, or nothing at all. The pattern itself matters, but symptoms matter just as much.
Third-degree AV block
This is the permanent red light.
Signals from the atria do not conduct to the ventricles in the usual way. The lower chambers rely on a backup rhythm instead. On a wearable, you may suspect this pattern rather than confidently diagnose it, especially with a single lead.

This is not the kind of finding to self-manage casually. If a strip suggests complete dissociation and the person has symptoms, it needs prompt medical attention.
Important: A watch can raise suspicion for AV block, but a single-lead tracing has limits. If the pattern is concerning or symptoms are present, use the watch as evidence to seek care, not as the final word.
Why AV block can happen
One reason can be reduced blood flow. The same Kenhub review notes that the right coronary artery commonly supplies the AV node. That is one reason ischemia can affect av nodal conduction.
Other times, the issue may be related to medicines, temporary physiology, higher vagal tone, or the fact that a wearable made a bad call on a noisy recording. The pattern matters, but the story around the pattern matters too.
Common Symptoms and Red Flags for AV Node Issues
Your watch shows a conduction alert, but you feel fine. Or you feel washed out and dizzy, yet the app gives you a vague label that does not tell you how worried to be. That gap is one of the hardest parts of AV node concerns, and it is why symptoms and daily context matter just as much as the tracing itself.
The AV node is like a gate in your heart’s wiring. If signals move through that gate too slowly, or some do not get through at all, your body may notice less blood flow for a moment. That is when people can feel lightheaded, weak, or short of breath. Some people feel nothing at all, especially if the finding is mild or temporary.
Symptoms that deserve closer attention
More significant conduction problems can cause:
- Lightheadedness, especially during a pause or a very slow stretch
- Dizziness that keeps recurring without an obvious explanation
- Unusual fatigue that feels out of proportion to your activity
- Shortness of breath during tasks that are usually easy
- Fainting or near-fainting, which needs prompt medical attention
A useful question is not “What did my watch say?” It is “What was my body doing at the same time?” A strip that appears mildly abnormal matters more if it lines up with symptoms you can feel.
When an alert may be less urgent
Some AV node findings on a watch are not an emergency, especially if you feel well. A prolonged PR interval, for example, can appear in people with high vagal tone, in trained athletes, or in people taking medicines that slow conduction.
Daily habits can affect what your watch records too. Dehydration, poor sleep, alcohol, stimulant use, and medication timing can all change heart rate or conduction enough to create a confusing strip. That does not mean every alert is harmless. It means the watch reading needs context from your day, your symptoms, and sometimes a repeat tracing.
Red flags that should change your next step
Use the pattern and the symptoms together.
- Get urgent medical help if you faint, nearly faint more than once, have chest pain, or develop severe shortness of breath along with a concerning rhythm alert.
- Contact your clinician soon if your watch repeatedly shows a possible conduction issue and you also feel dizzy, weak, unusually tired, or less able to exercise.
- Keep a log if you feel okay and the tracing is not alarming. Note the time, symptoms, activity, hydration, medications, caffeine, and alcohol. That record can make a follow-up visit much more useful.
If you are not sure whether what you felt sounds like a rhythm problem or a stress response, this guide to heart arrhythmia symptoms can help you sort out the difference.
Practical reassurance: A watch ECG can give an early clue, but it does not get the final say. One isolated alert without severe symptoms is often a reason to pay attention, capture a clean tracing, and look for patterns, not a reason to panic.
How Qaly Helps You Monitor Your AV Node
You get a watch alert during a normal day. Maybe you were walking the dog, answering emails, or lying in bed trying to relax. The alert sounds serious, but the screen gives you only a label. It does not explain whether the tracing shows a true AV node pattern, a temporary slowdown, or a messy recording.
That gap is often the hardest part.
AV node issues are about timing, and timing can be tricky on a watch ECG. A slightly longer PR interval, a harmless recording artifact, and a real dropped-beat pattern can look similar to a worried person staring at a tiny screen. If you already feel anxious about your heart, that uncertainty can make every alert feel bigger than it is.
Why automated alerts are not enough
A watch algorithm is a smoke alarm. It is helpful for getting your attention, but it cannot always tell whether the smoke came from burnt toast or a real fire.
That matters with AV node concerns because the question is rarely, "Was there an alert?" Instead, key questions include: Was the tracing clean enough to trust? Is the PR interval changing over time? Do your symptoms match the recording? Did this happen once, or is it becoming a pattern?
Wearable alerts can be useful early clues, but they do not replace review of the strip. They also do not know what was happening in your day, what medicines you take, or whether poor contact distorted the tracing.
What useful monitoring looks like
Good AV node monitoring works more like keeping a blood pressure log than reacting to one single number. You are looking for patterns that repeat and make sense together.
That usually includes:
- PR interval trends across more than one recording
- Symptoms at the same time as the ECG
- Medication changes or timing
- Daily factors like dehydration, alcohol, caffeine, or poor sleep
- Signal quality, because noise can imitate conduction problems
Qaly offers human-reviewed analysis of wearable and at-home ECGs, including interval measurements such as PR, QRS, and QTc, along with narrative reports from certified cardiographic technicians. For someone trying to sort out whether a watch alert points to a true AV node issue, a temporary body-state change, or a poor-quality strip, that added interpretation can be more helpful than an automated label alone.
How this can help you feel less stuck
Many people end up in an uncomfortable middle ground. The watch says something may be wrong. They do not feel bad enough to rush to the ER, but they also do not feel calm enough to ignore it.
A careful review can make that middle ground easier to handle. If several strips show the same delayed conduction pattern, that gives you something concrete to discuss with your clinician. If the recordings are inconsistent and noisy, that matters too. Clear reassurance is useful only when it is based on the tracing, your symptoms, and the bigger picture of your day.
In other words, the goal is not to hand your heart over to an app. The goal is to understand your own data well enough to know when to watch, when to follow up, and when to seek urgent care.
Frequently Asked Questions About the AV Node
Can stress alone cause an av node problem
Stress can make you more aware of palpitations and can affect heart rate, but a watch alert about av node timing needs context. Sometimes stress is the main issue. Sometimes stress makes you notice an underlying pattern more clearly.
Can medications affect the av node
Yes. Some medications can slow conduction through the av node. That is one reason a longer PR interval may appear after a medicine change. If a new ECG pattern shows up after starting or adjusting medication, log the timing and discuss it with your clinician.
If my watch says first-degree AV block, should I panic
No. A watch alert is not a verdict. First-degree block often needs context more than panic. Symptoms, repeat recordings, medication use, and the quality of the tracing all matter.
Can dehydration or poor contact fake an AV block
Yes. Wearable ECGs are sensitive to motion and poor signal quality. If the tracing is messy or the P waves are hard to see, repeat the recording before drawing conclusions.
Is an av node issue always permanent
No. Some patterns are temporary or situational. Others are more persistent. That is why trend tracking matters more than reacting to a single recording.
What should I bring to my appointment
Bring your cleanest ECG strips, the dates and times they were recorded, your symptoms, and notes about caffeine, alcohol, dehydration, exercise, and medication timing. A simple timeline helps more than a vague memory.
Have trouble measuring your PR Intervals? On the Qaly app, human experts will measure your ECGs' PR Intervals within minutes. Get started today.










.png)
.png)