Key Takeaways
Hello Heart Hero. We're glad you're here. If you've just come across the term "bidirectional ventricular tachycardia," or BVT, you might be feeling a mix of confusion and concern. It’s a very rare and specific kind of fast heartbeat that originates in the heart’s lower chambers, known as the ventricles.
Your Guide to a Complex Rhythm
Hearing a complicated medical term like bidirectional ventricular tachycardia can be overwhelming. We get it. Medical information is often dense, and it’s easy to feel left behind by a system that doesn’t always give you clear, straightforward answers. We created this guide to fix that.
Our goal is to break down BVT in a way that makes sense. We'll explain it without the heavy medical jargon, helping you understand what it is, what might cause it, and what it could mean for you. Understanding your heart is the first step toward taking back control of your health journey.
What Is Bidirectional Ventricular Tachycardia?
To understand BVT, let’s start with how your heart beats. Think of your heart's electrical system as a choreographer leading a dance. Normally, the steps are consistent and predictable, creating a steady rhythm.
In bidirectional ventricular tachycardia, it’s like the dancers suddenly start alternating their moves in completely opposite directions with every single beat. This creates a very specific, alternating "zigzag" pattern on an ECG.
This rare arrhythmia isn’t just a fast heartbeat; it’s a fast heartbeat with a unique beat-to-beat directional change. This signature is what makes BVT stand out from other rhythm problems and often points to a specific underlying cause.
How This Guide Can Help
Facing a potential heart issue can feel isolating, but you're not going through this alone. Many people are looking for better ways to understand their health, outside of short, rushed doctor's appointments. This guide is here to walk with you on that path. We’ll cover:
- What BVT is: Explained in simple terms you can actually use.
- The main causes: From medication side effects to rare genetic conditions.
- What it looks like on an ECG: So you can feel more empowered to recognize unusual patterns.
- Practical next steps: Helping you turn confusing information into a clear plan.
We'll go through this together, step by step. Our promise is to provide clarity and support, replacing fear with knowledge and helping you become an informed advocate for your own heart.
What BVT Looks Like on Your Wearable ECG
Let's break down what bidirectional ventricular tachycardia actually looks like on the ECG from your watch. Think about your normal heartbeat for a second. It creates a consistent, predictable wave on an ECG. With BVT, that signal becomes chaotic, but in a very specific and recognizable way.
The name "bidirectional" is quite literal. It means the main electrical push of your heartbeat, called the QRS complex, flips its direction back and forth. One beat points up, the next points down, creating a visually distinct pattern.
On an ECG from your wearable device, this looks like a fast, wide rhythm with a unique "zigzag" appearance. You'll see the peaks of the waves alternating in height and direction, one tall, one short, one tall, one short, over and over.
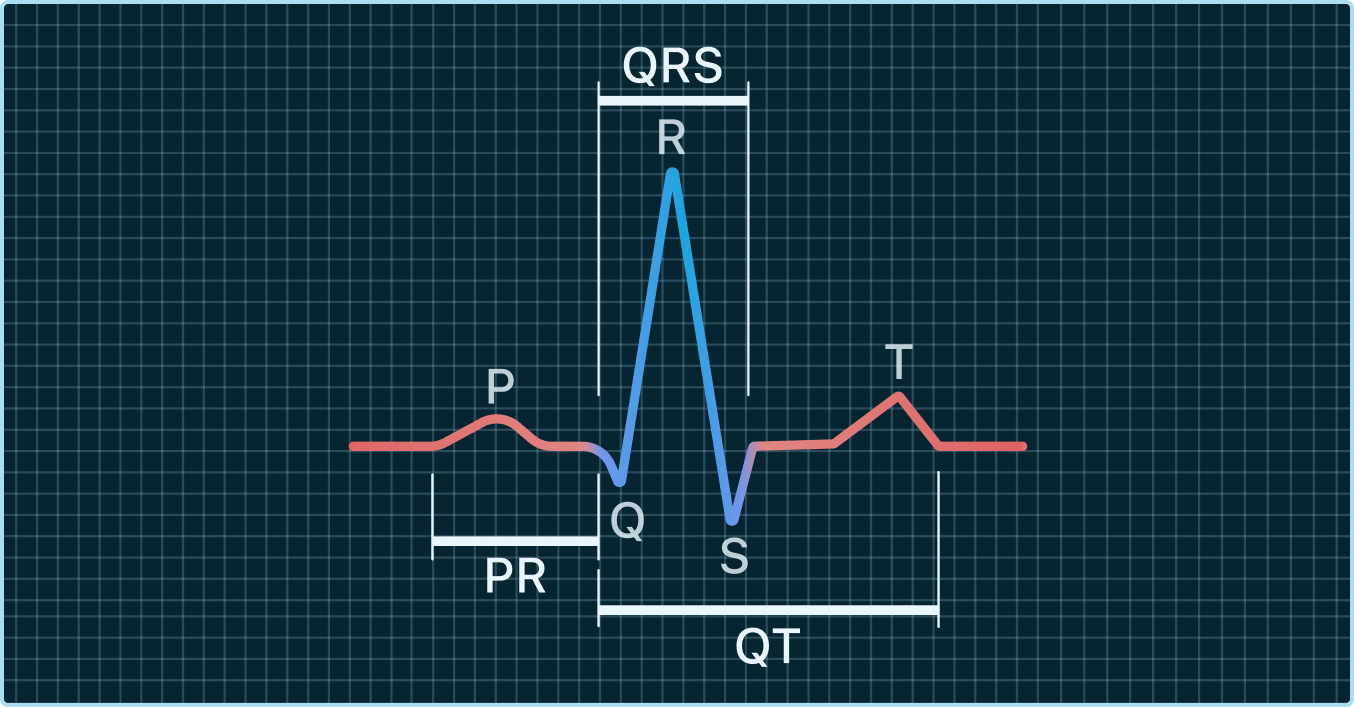
The Signature 'Zigzag' Pattern
So, what’s causing this? Imagine your heart's lower chambers, the ventricles, are getting rapid-fire signals from two different, competing spots. As they take turns firing, it creates that beat-to-beat electrical shift that is the absolute hallmark of bidirectional ventricular tachycardia.
This specific pattern is critical because it sets BVT apart from other fast heart rhythms. It’s not just about the speed; it's about this unique, alternating shape of the ECG waveform. Knowing this helps you recognize when a reading is unusual enough to need a professional review right away.
Bidirectional ventricular tachycardia (BVT) is one of the most striking yet rare heart rhythm disorders, first noted in medical literature back in the 1920s. Imagine your heart's electrical signals going haywire, causing the main electrical push on an ECG to flip 180 degrees beat by beat, creating that visual zigzag. A rate of 140-180 bpm combined with this axis shift can be a vital clue, flagging an underlying issue before it can worsen. To explore the history and clinical significance of this rhythm, you can read the full research on its ECG characteristics and causes.
Distinguishing BVT From Other Rhythms
When you're looking at a single-lead ECG from your watch, plenty of things can look scary. It's completely normal to feel a jolt of anxiety when you see any fast or messy-looking rhythm. But BVT has some key features that help tell it apart.
While this is never for self-diagnosis, here’s a quick comparison of what makes BVT different:
- Compared to Atrial Fibrillation (AFib): AFib is known for being "irregularly irregular," where the timing between heartbeats is completely random. BVT, on the other hand, is usually regular in its timing, but it’s the shape and height of the QRS complexes that alternate.
- Compared to other Ventricular Tachycardias (VT): Most types of V-Tach are "monomorphic," meaning the QRS complex has the same abnormal shape from beat to beat. BVT is a type of "polymorphic" V-Tach, where the shapes change, but they do so in a very predictable, alternating fashion. If you'd like to see more examples, you can check out our guide on whether your watch ECG can detect V-Tach.
- Compared to ECG Artifact: Sometimes, just moving your arm or having a poor connection can create a messy-looking ECG that might mimic a serious arrhythmia. We call this artifact. The key difference is that artifact is usually totally random and won't follow the organized, repeating, alternating pattern of BVT.
Recognizing that BVT has a specific look is empowering. It doesn't mean you should try to diagnose yourself. Instead, it helps you understand that certain patterns are more urgent than others and absolutely require an expert analysis. This knowledge can turn a moment of worry into a clear and productive conversation with your doctor or an ECG interpretation service like Qaly.
Exploring the Main Causes of This Rare Rhythm
Now that you have a clearer picture of what bidirectional ventricular tachycardia looks like, let's explore why it happens. This unique rhythm is not a random glitch; it's a very specific signal that almost always points to a significant underlying issue within the heart's electrical system.
The most classic and well-known cause is digoxin toxicity. Digoxin is a medication used for centuries to help the heart pump more strongly and control certain arrhythmias. However, if the level of this drug in the body becomes too high, it can seriously disrupt the heart's delicate electrical balance, leading to BVT.
This is a powerful reminder of how important it is to monitor medications, especially for drugs with a narrow therapeutic window. It’s not about being alarmed, but about being aware and engaged in your own treatment plan.
When the Problem Is Genetic
Beyond medications, bidirectional ventricular tachycardia is a key feature of certain rare genetic conditions. These are disorders someone is born with, where the very "wiring" of their heart's cells is different. One of the most important of these is catecholaminergic polymorphic ventricular tachycardia, or CPVT.
Imagine a heart that looks perfectly normal on the outside and even on a standard resting ECG. But when the person exercises or experiences strong emotions like excitement or stress, their body releases adrenaline. In someone with CPVT, this adrenaline surge triggers dangerous arrhythmias, including BVT.
CPVT is like a hidden electrical vulnerability in the heart. This inherited condition affects roughly 1 in 10,000 people and often strikes young, otherwise healthy individuals. Its hallmark is bidirectional VT triggered by adrenaline. Without treatment, the outlook can be serious, with mortality rates as high as 30-50% by age 35. Discover more about the genetics and risks of CPVT on aerjournal.com.
Another rare genetic disorder that can cause bidirectional ventricular tachycardia is Andersen–Tawil syndrome (ATS). This condition is a bit different because it affects more than just the heart. People with ATS often have unique physical features and may experience episodes of muscle weakness or paralysis, in addition to arrhythmias like BVT.
Other Potential Triggers
While digoxin toxicity and genetic conditions are the most common culprits, other factors can also create the right environment for this arrhythmia. Severe disturbances in the body's chemistry can play a role.
These less frequent causes can include:
- Severe Electrolyte Imbalances: Very low or very high levels of minerals like potassium are critical for stable heart function. An extreme imbalance can disrupt the heart's electrical signals enough to trigger BVT. You can learn more about how electrolyte imbalance impacts your ECG in our detailed guide.
- Toxicity from Other Substances: In very rare cases, poisoning from certain chemicals, such as dichloromethane (a solvent found in some paint strippers), has been reported to cause BVT by directly harming heart tissue.
- Heart Inflammation (Myocarditis): When the heart muscle becomes inflamed due to infection or other causes, it can lead to electrical instability and, in rare instances, trigger BVT.
Understanding that bidirectional ventricular tachycardia has specific and identifiable causes is a crucial step. It transforms the rhythm from a mysterious event into a clue, guiding you and your care team toward the right diagnosis and the most effective path forward.
How Doctors Manage and Treat BVT
Seeing a fast, bizarre rhythm on your watch ECG or feeling scary symptoms is deeply unsettling. We get it. But knowing how doctors approach bidirectional ventricular tachycardia can give you back a powerful sense of control.
The good news is that because BVT points so specifically to certain causes, the treatment plan is often very direct. Management is typically split into two phases: immediate action during an episode and long-term prevention. Both have the same simple goal: getting you back to living your life with confidence.
Immediate Action in an Emergency
When someone is actively in BVT and feeling very unwell, the first priority is to stabilize their heart rhythm right away. This all happens in an emergency room, where the team can act fast to protect your heart.
The first step is to stop the dangerous rhythm and get a normal beat back. Doctors will quickly check if you are "stable," which means your blood pressure is okay and you're conscious. If not, they may need to use an electrical shock (cardioversion) to instantly reset the heart. It sounds dramatic, but it's the fastest and most effective way to stop an unstable arrhythmia.
If you're stable, the focus turns to medication. You'll likely receive specific intravenous (IV) medicines to calm the heart's overactive electrical system and break the BVT cycle.
The most crucial step is often treating the root cause on the spot. If digoxin toxicity is the culprit, for instance, doctors can give an antidote called Digibind. This rapidly neutralizes the excess medication, directly fixing the problem instead of just managing the symptoms.
Long-Term Prevention Strategies
Once the immediate danger has passed, the conversation shifts entirely to long-term prevention. The goal here is simple: to make sure bidirectional ventricular tachycardia doesn't happen again. This part of your care is highly personalized, and it all depends on the underlying cause that was found.
This is where you become a key partner in your own health. Your input, lifestyle, and how you feel about different options are all part of the discussion.
Common long-term strategies include:
- Medication Adjustments: If BVT was caused by digoxin toxicity, the solution is straightforward: your doctor will stop or drastically lower your dose. For genetic conditions like CPVT, medications called beta-blockers are the first line of defense. They work by blunting adrenaline's effect on the heart, which helps prevent the triggers that can set off arrhythmias.
- Implantable Cardioverter-Defibrillator (ICD): For higher-risk conditions, especially CPVT, an ICD is often recommended. Think of it as a personal safety net. It's a small device implanted under the skin that constantly watches your heart. If it ever detects a life-threatening rhythm like BVT, it automatically delivers a small shock to restore a normal beat. This can provide incredible peace of mind.
- Lifestyle Modifications: For people with CPVT, managing adrenaline triggers is a big part of staying healthy. This doesn't mean you have to live in a bubble, but it does mean working with your doctor to find safe levels of physical activity and developing ways to handle emotional stress.
Making decisions about long-term treatment, like getting an ICD or starting a new daily medication, can feel overwhelming. It’s okay to take your time, ask every question that comes to mind, and speak up for what feels right for you. It's also important to understand the potential side effects of any treatment, and you can learn more about how antiarrhythmic drugs' side effects can affect your ECG.
Ultimately, every treatment for bidirectional ventricular tachycardia is designed to give you back your freedom and security.
Making Sense of Your Wearable ECG Data
Your personal ECG device is a powerful health ally, but we get it, looking at the data can feel confusing, maybe even a little scary. This guide is here to give you clear, practical steps for what to do with the ECGs you record, especially if you see something that makes you worry.
While bidirectional ventricular tachycardia is incredibly rare, its unique alternating pattern can sometimes show up on a single-lead ECG from your watch. You might notice a very fast rhythm where the QRS complexes, the tall spikes of your heartbeat, seem to flip-flop in direction. One beat could have a tall, upward spike, and the very next beat could have a deep, downward one.
This is what creates that "zigzag" or alternating look we talked about. Seeing this can be alarming, for sure. But it's important to understand both what your device can do and what its limits are.
What to Do If You Record a Concerning Rhythm
First things first: stay as calm as you can. Panicking can drive your heart rate even higher and make it tough to think straight. If you capture an ECG that looks very fast, bizarre, and has that alternating pattern, here’s a simple game plan.
Your main goals are to save the recording and get it looked at by a professional. This simple process turns a moment of anxiety into productive action.
Here’s what you can do:
- Save the ECG Strip: Make sure the ECG recording is saved in your device’s app. This is the single most valuable piece of information you can have.
- Add Notes: If the app lets you, jot down how you were feeling in that moment. Were you dizzy, short of breath, or feeling palpitations? This context is crucial for a proper interpretation.
- Do Not Self-Diagnose: It’s so tempting to go searching for answers online, but this almost always leads to more anxiety. Remember, electrical "noise" or artifact can sometimes mimic a serious arrhythmia. Resist the urge to jump to conclusions.
Getting a human expert to look at your ECG is the next critical step. This is where you take back control, bypassing the long waits and uncertainty that can come with trying to get answers through traditional channels.
The real power of your wearable ECG isn't in diagnosing yourself, but in its ability to capture those fleeting moments. When you pair this data with an immediate, human-verified interpretation, you build a bridge from confusion to clarity.
This approach provides a clear, professional report you can then take to your doctor for a much quicker and more informed conversation. It puts you in the driver’s seat of your own health monitoring.
Why Professional Review Is Non-Negotiable
A single-lead ECG from a watch is a fantastic screening tool, but it's not a diagnostic machine. A trained human eye can spot the subtle differences between true bidirectional ventricular tachycardia and other rhythms or artifacts that might look similar.
For instance, a technician can see if the wide shapes of the QRS are consistent with a ventricular origin. To get a better handle on what makes a QRS complex wide or narrow, you might find it helpful to check out our guide on the QRS interval on your watch ECG. This knowledge helps put your own recordings into better context.
A service like Qaly is built for exactly this situation. Within minutes of uploading your ECG, a certified cardiographic technician can analyze the strip. They can tell you if the rhythm is dangerous, if it's a more benign arrhythmia, or if it's simply artifact.
This immediate feedback does two things. First, it can bring immense peace of mind if the rhythm turns out to be harmless. Second, if it is a concerning rhythm like bidirectional ventricular tachycardia, it gives you a validated report to take straight to your doctor or the emergency room. You're no longer just saying, "I felt funny"; you're presenting concrete, professionally reviewed evidence. This empowers you and speeds up your path to getting the right care.
Your Questions About Bidirectional Ventricular Tachycardia
It's completely normal to have questions when you're looking at a potential diagnosis. We get it, this journey can feel overwhelming, and finding clear answers is a huge part of feeling more in control. We've listened to the most common concerns and are here to offer straightforward, reassuring answers.
Our goal is to give you the honest information you're looking for, so you can feel more confident and prepared for the conversations ahead with your doctor.
Can I Live a Normal Life with a Condition That Causes BVT?
Yes, absolutely. Hearing that you have a condition that can cause bidirectional ventricular tachycardia, like CPVT, is scary. It’s natural to wonder if your life will ever feel normal again. The answer is a definite yes, and modern medicine is designed to help make that happen.
It’s all about management. The goal of treatment isn't just to keep you safe; it's to help you lead a full, active, and vibrant life. Think of it as a partnership between you and your healthcare team, working together to find the best strategy. This might involve a daily medication like a beta-blocker to prevent adrenaline-fueled arrhythmias, or an implantable cardioverter-defibrillator (ICD) that acts as a reliable safety net. An ICD constantly monitors your heart, and for many people, having that protection provides incredible peace of mind.
Once a solid plan is in place, countless people get back to their jobs, hobbies, and family activities with confidence. Your wearable ECG becomes a valuable tool in this new normal, making you an active, informed partner in your own care. It lets you and your doctor see how your heart responds to different activities and medications, providing priceless insights.
Does a Fast, Irregular Rhythm on My Watch Mean I Have BVT?
No, not necessarily. Seeing a fast or chaotic-looking rhythm on your watch ECG can make your heart race for a whole different reason: anxiety. Before you panic, take a deep breath and remember that many things can cause a strange-looking recording. Most of the time, it's not a serious arrhythmia.
The most common culprit is something called artifact, which is just electrical noise from movement. If you were moving your arm, talking, or didn't have a good skin connection, your ECG can look wild and messy. It might look alarming, but it isn't your actual heart rhythm. Other, more common arrhythmias can also appear fast and irregular.
Bidirectional ventricular tachycardia has a very specific alternating pattern that is extremely rare. Jumping to the conclusion that you have BVT from one strange ECG can cause a lot of unnecessary stress. The best first step is always to get the recording professionally reviewed. A trained technician can easily spot the difference between artifact, a common arrhythmia, and a genuinely concerning rhythm.
Is BVT Always Considered a Medical Emergency?
Yes, bidirectional ventricular tachycardia is a life-threatening arrhythmia that requires immediate medical attention. This is not a "watch and wait" rhythm. It's an unstable rhythm that signals serious electrical trouble in the heart and can quickly progress to ventricular fibrillation, a form of cardiac arrest.
If you are experiencing symptoms like severe dizziness, fainting, shortness of breath, or chest pain along with a very fast heart rate, you should seek emergency medical care immediately. Every second counts.
Even if you capture an ECG that looks like BVT but your symptoms aren't severe, that recording is a critical warning sign. It shows that the heart is electrically unstable, and the underlying cause must be found and treated quickly to prevent a more dangerous event. Never dismiss a rhythm that looks like BVT.
How Can an App Like Qaly Help if I See a Concerning ECG?
Looking at a concerning ECG on your watch without understanding its implications can be distressing. The anticipation of a doctor's appointment or waiting for a callback can seem interminable. An app like Qaly offers valuable support and clarity in such situations.
Rather than waiting anxiously, you can take immediate action. Upload your ECG to the app, and within minutes, a certified cardiographic technician provides a detailed review, available 24/7. They are trained to identify various arrhythmias and can quickly differentiate between serious rhythms, more benign issues, or simple electrical noise.
This service not only offers a quick response but also provides a reliable, professional report that you can share with your doctor. Instead of merely describing symptoms, you're presenting concrete, expertly reviewed data. This assists your doctor in making faster, more informed decisions about your health and empowers you to take control.
Qaly provides on-demand, expert analysis of your wearable ECGs, turning moments of anxiety into clear, actionable insights.










.png)
.png)