Key Takeaways
Hello, Heart Hero. That flutter, skip, or thump you’ve felt in your chest has a name: an ectopic beat. The term ectopic beat burden is simply a way of measuring how often these little heart "hiccups" happen over a certain period. Understanding this measurement is the first and most powerful step toward turning worry into clarity and having more confident conversations with your doctor.
What Are Ectopic Beats and Why Does Burden Matter?
If you're reading this, you've probably felt an unsettling sensation in your chest and want answers. You’re not alone, and it's completely understandable to feel frustrated when those concerns are brushed aside in a healthcare system that often feels rushed. This guide is here to empower you with clear, reassuring information.
Let's start by demystifying what's happening. An ectopic beat is just an extra or early heartbeat. Imagine your heart is a drummer keeping a perfect, steady rhythm. An ectopic beat is like a single, out-of-place tap on the drum that briefly messes with the beat. It feels weird, but most of the time, it's just a temporary blip.
These "blips" come in two main flavors:
- Premature Atrial Contractions (PACs): These start in the heart's upper chambers (the atria).
- Premature Ventricular Contractions (PVCs): These come from the heart's lower chambers (the ventricles).
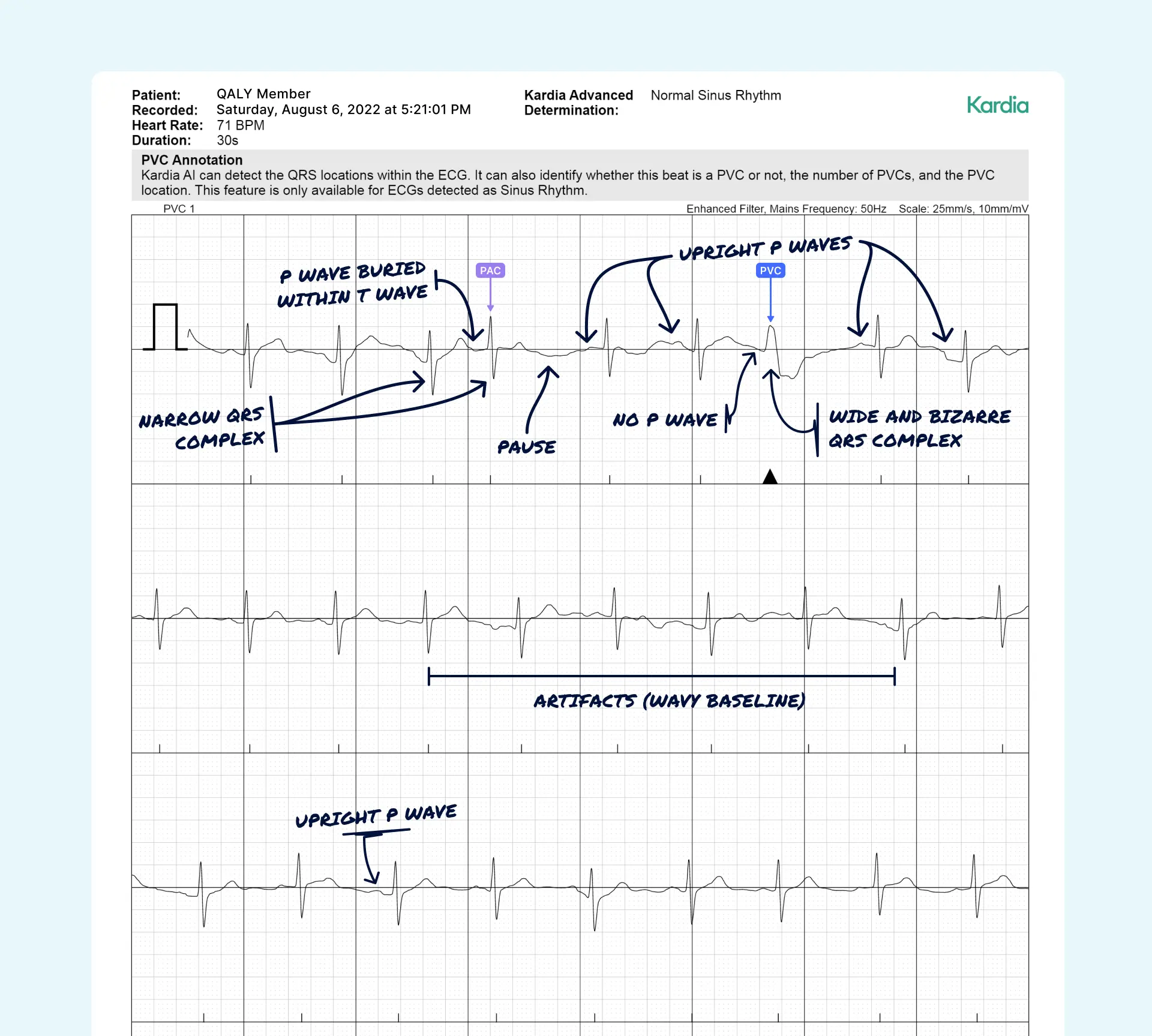
From a Single Beat to a Bigger Picture
While a one-off flutter is pretty common, what really matters for your health is how often they're happening. This is where the idea of ectopic beat burden comes in. It’s not about fixating on one skipped beat; it's about figuring out the percentage of these hiccups compared to your total number of heartbeats throughout the day.
This percentage gives you and your doctor valuable context. The medical community really started paying attention to this after a landmark 2010 study showed that even small increases in PVCs could be linked to changes in heart function. Researchers found that a two-fold increase in someone's PVC burden was associated with a higher chance of their heart's pumping ability declining. This is exactly why tracking the burden is so much more useful than just noting a single odd beat.
By measuring the burden, you shift the focus from a single, scary moment to a broader, more manageable pattern. It’s the difference between seeing one raindrop and understanding the total inches of rainfall.
Our goal is to help you get a handle on this measurement so you feel informed and in control. Knowing your ectopic beat burden gives you peace of mind and the confidence to know exactly when and how to talk to your doctor.
How Ectopic Beat Burden Is Measured
When you feel those confusing heart hiccups, it’s natural to want to know what they mean. Doctors have a specific way of quantifying them, and understanding this process can give you a real sense of control. The key metric they use is the ectopic beat burden, and it's what gives them a clear picture of what’s happening inside your chest.
Think of it like tracking rain. You could count the individual raindrops, or you could measure the total inches of rainfall. Just counting the beats is like counting raindrops, for example saying you had 500 PVCs in 24 hours. But calculating the percentage, like a 1% ectopic beat burden, is like measuring the total inches. It puts the number in context and tells you how significant the "rainfall" really was for your heart's rhythm that day.
Holter Monitors: The Gold Standard
To get an accurate daily percentage, cardiologists often turn to the Holter monitor. This is a small, portable device you wear for 24 to 48 hours, sometimes even longer. It’s the gold standard because it continuously records every single heartbeat, leaving no gaps.
This complete picture allows for a very precise calculation of your total ectopic beat burden. Because it captures everything, the Holter can tell your doctor if you have a 1%, 5%, or 15% burden over a full day. This comprehensive data gives them a reliable baseline to distinguish between harmless, occasional flutters and a pattern that might need a closer look.
For those whose symptoms are rare and might be missed in a day or two, your doctor might suggest a longer-term solution like an implantable device. You can learn more about how these work in our guide on what an internal loop recorder is and how it helps track heart rhythms for months or years.
Wearables: Your Personal Health Detective
Your Apple Watch, Kardia, or Fitbit is an incredible tool, but it works very differently from a Holter monitor. These devices are built for “spot checks.” They take a snapshot of your heart rhythm, usually for about 30 seconds, right when you tell them to.
This is a powerful feature. It means you can capture your heart’s activity the moment you feel a symptom. That fleeting flutter can be turned into concrete data that you can share with your doctor.
However, it's crucial to understand the limitations here. A wearable doesn’t calculate your daily ectopic beat burden because it isn't recording continuously. Seeing a few PVCs on a single 30-second recording is a world away from having a consistently high burden measured over 24 hours.
Knowing this distinction is so important. It can save you from the unnecessary anxiety that comes from over-analyzing a single ECG strip. Instead of worrying about one or two odd beats, think of your wearable as a tool to spot patterns and capture episodes when you feel them. This way, you become an active partner in your own care, armed with useful information for your next doctor’s visit.
When Ectopic Beat Burden Becomes A Concern
You've felt the flutters, tracked the data on your watch, and now you’re asking the big question: when does my ectopic beat burden actually become a problem? This is where we shift from just noticing these heart hiccups to understanding what the numbers truly mean for your long-term health. It’s completely normal to feel a bit anxious about this, and getting clear answers is the best way to find some peace of mind.
The numbers themselves are just one piece of the puzzle, but they provide a crucial starting point for a meaningful conversation with your doctor. Understanding these clinical thresholds empowers you to know when your situation might need a closer look.
The Numbers That Matter Most
From a clinical perspective, many doctors start paying closer attention when a person’s ectopic beat burden from PVCs consistently rises above 10% to 20% of their total heartbeats over a 24-hour period. This isn't just an arbitrary number. This range matters because of a potential long-term risk of the heart muscle weakening over time, a condition known as PVC-induced cardiomyopathy.
Think of it this way: if your heart is a powerful engine, a very high burden of PVCs is like asking it to run inefficiently for a long, long time. Over years, this extra strain can sometimes tire out the heart muscle.
A high burden of PACs is viewed a bit differently. While less directly linked to weakening the heart muscle, a consistently high PAC burden can sometimes be a sign of increased electrical instability in the heart's upper chambers. For some people, this could indicate a higher future risk of developing other arrhythmias, like atrial fibrillation.
The goal here is not to cause alarm, but to give you context. Awareness of these potential long-term risks is the very first step in being proactive about your heart health.
The Significance of High Ectopic Beat Burden
Our medical understanding of this has evolved quite a bit over the years. A landmark 23-year study of over 6,000 initially asymptomatic men provided powerful evidence. Researchers found that men with frequent ventricular ectopy, specifically more than 10% in a short recording, had a much greater risk of cardiovascular issues down the line compared to those without.
This kind of research helped establish that even in people without symptoms, a high ectopic beat burden could be an important predictor of future risk. This is precisely why tracking your burden is so valuable. It gives you the information needed to flag when you're approaching a threshold that warrants a discussion with your healthcare provider.
Why Your Symptoms Are Just As Important
While thresholds like 10% are useful clinical guideposts, they don’t tell the whole story. Your personal experience, specifically how you feel, is just as critical. A very low ectopic beat burden that causes you significant distress is absolutely a valid reason to seek medical advice.
Your symptoms matter immensely. Here are a few examples of when your feelings are as important as the data:
- Significant Dizziness or Lightheadedness: If your ectopic beats leave you feeling faint or unsteady, it needs to be addressed, regardless of the burden percentage.
- Shortness of Breath: Feeling winded or unable to catch your breath during episodes of palpitations is a signal that your body is being affected.
- Chest Discomfort or Pain: Any pain or significant tightness associated with your ectopic beats should always be evaluated.
- Severe Anxiety: If the sensations are causing a major disruption to your quality of life and mental well-being, that alone is a valid medical concern.
Never let anyone tell you it's "just anxiety" if what you're feeling is real and disruptive. Your lived experience is a vital piece of your health profile. Sometimes, the primary goal is simply managing symptoms, and for that, treatments might be considered even at a lower burden. If you're exploring treatment options, you might be interested in our guide on beta-blockers for PVCs, which are often a common first step.
Making Sense Of Your Wearable ECG Data

Your wearable is way more than just a heart rate counter. Think of it as a powerful tool that gives you a direct window into your heart’s daily rhythms and patterns. So, when you see a notification pop up with an acronym like ‘PVC’ or ‘PAC,’ it’s natural to feel a jolt of concern. My goal here is to help you transform that raw data from a source of anxiety into a source of personal insight.
The trick is to shift your perspective. Instead of fixating on a single, 30-second ECG strip, the real value comes from zooming out to see the bigger picture. Your device helps you become your own health detective, connecting the dots between your life and your heart rhythm. This way, you can start piecing together a story that a single heartbeat could never tell.
Becoming a Pattern Detective
Treat each ECG you take as a clue. One clue on its own might not mean much, but collecting them over time can reveal some surprisingly clear patterns. The next time you notice an uptick in ectopic beats, start asking yourself some simple detective questions.
- Timing: Do they pop up more often at a certain time of day? Maybe after your morning coffee ritual, or late at night when you’re finally trying to unwind?
- Triggers: What was going on right before you felt that flutter? Were you navigating a stressful meeting, feeling a wave of anxiety, or had you just finished a heavy meal?
- Lifestyle Factors: How did you sleep last night? Were you well-hydrated? Did you have a glass of wine the evening before?
Simply by noticing these connections, you begin to build a personal profile of your unique triggers. This information is incredibly valuable, both for your own peace of mind and for sharing with your doctor. Figuring out what might be causing your ectopic beats is often the very first step toward managing them.
Reading Your Wearable Reports
When you pull up a report from your watch, you’ll usually see the ECG waveform itself alongside the device’s algorithmic interpretation. For a great visual guide on what you're looking at, check out our article on how to identify ectopic beats on your Apple Watch ECG. And remember, while these algorithms are smart, they aren't perfect. Their main job is to flag potential blips for you to look into further.
The goal isn't to diagnose yourself. It's to collect high-quality data that helps your doctor understand what you are experiencing. A clear recording linked to a specific symptom is one of the most useful things you can bring to an appointment.
This is where you can really take charge. Instead of just being a passive recipient of data, you can actively work to capture the cleanest, most useful information possible for your healthcare team.
Tips for a Crystal-Clear ECG Recording
To make sure the data you share with your doctor is as helpful as possible, you need a clean recording without any "noise" or artifact. Electrical noise can make an ECG nearly impossible to read accurately, so follow these simple steps every single time.
- Sit Down and Relax: Find a comfortable chair and rest your arms on a steady surface, like a table or even your lap. Don't try to take a recording while you're walking around.
- Stay Still and Silent: Any movement, even talking, creates tiny muscle contractions that show up as fuzzy interference on your ECG. Take a few deep breaths and try to stay as still as possible for the full 30 seconds.
- Ensure Good Contact: Make sure your skin is clean and dry. Lotions or sweat can mess with the electrical signal. Just rest your finger gently on the sensor without pressing down too hard.
By making these small steps a habit, you turn your wearable from a simple monitor into a serious data-gathering tool. You'll be creating a clear, readable log of your heart's activity that makes your conversations with your doctor more focused and productive, ensuring your concerns are backed up by solid evidence.
Lifestyle Strategies To Help Manage Ectopic Beats

Feeling those frustrating heart flutters can leave you feeling powerless, but this is exactly where you can start taking back some control. Many people find that simple, gentle lifestyle adjustments make a real difference in how often they experience ectopic beats.
This isn't about finding a magic cure. It's about discovering what helps your body and heart feel their calmest and most stable. Think of it as a series of compassionate experiments in self-care. The goal is to pinpoint your personal triggers and build routines that support your heart's natural rhythm.
Tuning Into Your Body’s Triggers
One of the most powerful things you can do is become a detective of your own body, figuring out what might be sparking your ectopic beats. For many of us, the culprits are hiding in plain sight.
- Caffeine and Alcohol: These are well-known stimulants that can ramp up your heart rate and make its electrical system a bit more "irritable." You might not need to cut them out completely, but experimenting with reducing your intake could be very revealing. For more on this, check out our guide on examining coffee's impact on your heart.
- Dehydration and Electrolytes: Your heart's electrical wiring relies on a delicate balance of minerals like magnesium and potassium. When you're dehydrated, this balance gets thrown off. Simply making sure you're drinking enough water is a small but crucial step.
- Poor Sleep: A lack of consistent, quality sleep puts a strain on your entire body, including your heart. Prioritizing a regular sleep schedule can have a profoundly calming effect on your nervous system and, in turn, your heart rhythm.
Managing Stress and Calming Your Nervous System
Stress and anxiety are major triggers for ectopic beats. Why? They activate your body’s "fight or flight" response, flooding your system with adrenaline and putting your heart on high alert. Learning to soothe your nervous system can be a game-changer.
Simple practices can make a huge difference. Try adding a quiet 15-minute walk to your daily routine, or practice some deep breathing exercises when you feel overwhelmed. Regular physical activity is also a fantastic stress reliever. When you're building a fitness habit, learning how to effectively balance cardio and strength training is key to getting the benefits without overdoing it.
By focusing on what you can control, like your breath, your hydration, or your evening routine, you shift from a place of worry to a position of empowerment. Each small change is a step toward feeling better.
This approach isn't just about feeling better in the moment; it's also a key preventative strategy. For instance, research has shown that excessive supraventricular ectopic activity (ESVEA), or frequent PACs, can be a significant predictor of future atrial fibrillation.
One study involving over 23,000 participants found that having frequent PACs significantly increased the risk of developing AFib, a condition linked to stroke. This makes monitoring and managing these ectopics an important part of your long-term health.
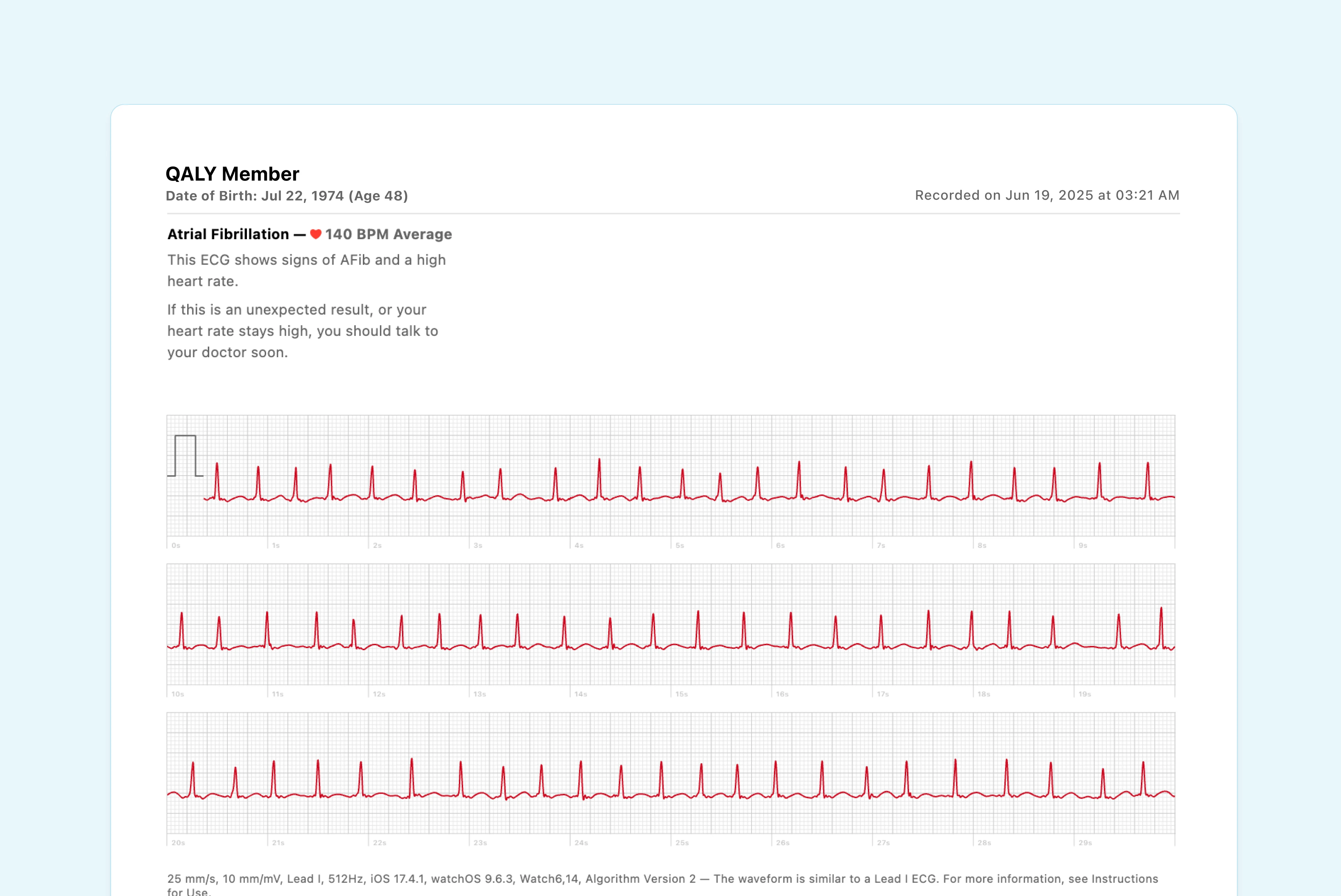
Ultimately, these lifestyle adjustments are powerful because they put you in the driver’s seat. By patiently observing your body and making small, sustainable changes, you can often reduce your ectopic beat burden and, most importantly, improve your quality of life.
How To Talk To Your Doctor About Your Heart Rhythm
Turning your personal health data and your very real concerns into a productive conversation with your doctor is a huge step. This is where you move from being a passive patient to an informed partner in your own healthcare. A clear, well-prepared approach makes sure your worries about your ectopic beat burden are heard, respected, and thoroughly addressed.
It's easy to feel overwhelmed walking into an appointment, worried you won’t be taken seriously. The key is to shift from presenting a pile of random ECG strips to telling a clear, concise story backed by your data. This simple change in approach can make all the difference.
Prepare Your Story Before You Go
Before your visit, take a moment to organize your thoughts and your data. The goal is to give your doctor a summary that’s easy to digest quickly. Instead of just saying "my heart feels weird," you can frame your experience in a much more impactful way.
For example, you could say something like this: "Over the past month, I've noticed a pattern of palpitations that seem to happen most evenings, especially on stressful days. I’ve captured several examples on my watch, and they often feel like a strong thud followed by a pause." This single sentence provides context, identifies a potential trigger, and describes the physical sensation.
Articulating your experience with clarity and confidence is the most powerful tool you have. It helps your doctor understand not just what is happening, but how it is impacting your daily life.
By preparing your story, you set the stage for a collaborative conversation. You’re not just presenting a problem; you're presenting valuable clues that can help solve it.
What to Bring to Your Appointment
Being organized shows you're serious about your health and helps your doctor get the full picture right away. A little prep can make your limited appointment time much more effective.
Here’s a simple checklist of what to bring along:
- A Symptom Diary: Just a brief log noting the date, time, what you were doing, and how you felt during episodes.
- Key ECG Examples: Save or print a few clear ECG recordings that match up with your most significant symptoms. You don't need to bring every single one.
- A List of Questions: Write down your questions beforehand so you don’t forget anything in the moment. Simple as that.
- Your Goals for the Visit: Know what you want to get out of the appointment. For instance, you might say, "My main goal today is to understand if these ectopic beats are harmless and to discuss potential strategies for reducing them."
This organized approach helps focus the conversation on what matters most to you. It ensures your concerns about your ectopic beat burden aren't just mentioned but are central to the discussion, leading to better outcomes and, hopefully, greater peace of mind.
Frequently Asked Questions About Ectopic Beat Burden
Diving into your heart rhythm data can bring up a lot of questions, and it’s perfectly normal to want clear answers. We’ve gathered some of the most common things people ask when they start tracking their ectopic beats. Think of this as a final layer of clarity and reassurance on your journey.
Can My Wearable Accurately Measure My Total Ectopic Beat Burden?
Your wearable device, like an Apple Watch or Fitbit, is incredibly useful for "spot checks." It’s designed to capture your heart rhythm the moment you feel a symptom, giving you a snapshot in time.
However, it can't measure your total daily ectopic beat burden the way a 24-hour Holter monitor from a doctor's office can. A true burden calculation needs continuous, around-the-clock monitoring to figure out what percentage of your total heartbeats are ectopic. The real power of your wearable is its ability to find patterns and catch symptoms as they happen, and these are the essential clues you and your doctor need.
Is It Normal For My Ectopic Beats To Fluctuate Daily?
Yes, absolutely. It's very common and completely normal for the number of ectopic beats to change from one day to the next. Dozens of factors can influence this, including:
- Your stress levels
- How well you slept
- Your hydration and electrolyte balance
- Dietary choices like having caffeine or alcohol
This is exactly why looking at trends over several weeks gives you a much better picture than worrying about the numbers from a single day. A consistent, significant increase over time is what really matters and what should prompt a conversation with your provider.
What Is The Difference Between PVCs And PACs?
Both PVCs and PACs are types of ectopic beats, but the key difference is where they start in your heart.
- PACs (Premature Atrial Contractions) are early beats that fire from the heart’s upper chambers, known as the atria.
- PVCs (Premature Ventricular Contractions) come from the lower chambers, the ventricles.
While both can feel like a flutter or a skipped beat, doctors often view their long-term significance differently. For anyone curious about how a heart condition might affect insurance, this resource is helpful for understanding pre-existing conditions health insurance.
Turn your heart palpitations into clear data. Start tracking your ectopic burden with Qaly.










.png)
.png)