Key Takeaways
Hello Heart Hero.
You had a drink, maybe two. The night seemed normal. Then later your chest started doing something strange. A flutter. A hard thump. A run of fast beats that made you stop mid-sentence and wonder if you should be worried.
That experience can feel unsettling, especially when it seems to come out of nowhere. A lot of people get dismissed with vague advice like “cut back a little” or “it’s probably anxiety,” and that can leave you stuck between fear and frustration. If you're dealing with heart palpitations after drinking alcohol, you're not overreacting by wanting a clearer explanation.
That Scary Flutter After a Drink Is Real and You're Not Alone
A very common story goes like this. Someone has wine with dinner or a few drinks at a party. They go home, try to sleep, and suddenly notice their heartbeat feels louder, faster, or uneven. Some describe it as a fish flopping in the chest. Others say it feels like a skipped beat followed by a heavy “catch-up” beat.
If that's happened to you, your body isn't making it up. Alcohol can affect heart rhythm in real, physical ways. For some people it causes a brief racing sensation. For others it can trigger a more clearly irregular rhythm.
Many readers first search for symptoms like chest fluttering before they even know the word “palpitations.” If that sounds familiar, this guide on heart fluttering sensations and what they can mean may also help you put words to what you're feeling.
Why this feels so frightening
Palpitations are scary because your heart is usually something you don't notice. When it suddenly becomes impossible to ignore, your brain treats it like an alarm. That doesn't automatically mean danger, but it does mean your attention gets pulled straight to it.
You don't need to choose between panic and denial. You can take the symptom seriously without assuming the worst.
What you deserve right now
You deserve more than “wait and see” with no context. You deserve to understand what alcohol can do to the heart, which kinds of rhythm changes are more likely, when to get urgent care, and how to use the tools you already have, like an Apple Watch, Fitbit, Kardia, Samsung watch, or Withings device, to gather useful information instead of spiraling in uncertainty.
Why Alcohol Can Make Your Heart Skip a Beat
A normal heartbeat depends on tiny electrical signals moving through the heart in the right order. First the upper chambers fire, then the lower chambers follow. When that sequence stays organized, you usually feel nothing. When alcohol interferes with the timing, you may notice a thump, a pause, a flutter, or a short burst of racing.
Alcohol can affect that timing in several ways at once. That is why the experience can feel so confusing. You may have one drink and feel fine, then have symptoms later in bed and wonder whether the two are even related. In many people, they are.

It can disturb your body's fluid and mineral balance
Alcohol increases fluid loss. If you are also sweating, eating less than usual, or staying up late, the shift can be stronger. That matters because heart cells rely on minerals such as potassium and magnesium to pass electrical signals cleanly from one cell to the next.
A small change in those minerals does not guarantee an arrhythmia, but it can make the heart more irritable. That is one reason symptoms often show up after a night that also included dehydration, salty food, poor sleep, or vomiting. This practical guide to electrolyte imbalance and ECG changes explains why those shifts can sometimes show up on a tracing.
It can push your nervous system into a more reactive state
Your heart rate is partly controlled by the autonomic nervous system, which adjusts speed and rhythm in the background without you having to think about it. Alcohol can disrupt that balance.
Research summarized in the NCBI review on alcohol and atrial fibrillation describes how alcohol can promote atrial fibrillation through electrophysiologic effects and sympathetic activation. In plain language, alcohol can make heart cells reset faster than usual and make the body's “fight or flight” signals louder. That combination can make extra beats or disorganized rhythms more likely in some people.
A simple way to picture the reset problem is a camera flash that needs a moment to recharge before the next photo. Heart cells also need a brief recovery period after each beat. If that recovery window gets shortened, stray signals have a better chance of slipping through.
The timing can be delayed
Many people expect palpitations to happen during the drink itself. Often they show up hours later.
That delay makes sense. Your body may still be dealing with dehydration, lighter sleep, a faster resting heart rate, and lingering stress hormones long after the last drink. The same NCBI review on alcohol and atrial fibrillation notes that hangover states can keep resting heart rate increased, which helps explain the late-night or next-morning “why is my heart doing this?” moment.
Binge drinking can trigger a recognizable rhythm pattern
Doctors have long observed a pattern where heavier-than-usual alcohol intake is followed by an episode of irregular rhythm, often atrial fibrillation. You may hear this called holiday heart syndrome.
The name sounds casual, but the event is not. A person with no known heart condition can still develop a real rhythm disturbance after a weekend, celebration, or vacation where they drank more than their usual amount. Sometimes it settles after alcohol is out of the system. It still deserves attention, especially if it happens more than once.
Why your reaction may be different from someone else's
This part frustrates people. One friend can drink several cocktails and feel nothing. Another person gets a hard skipped beat after one or two drinks.
That difference does not mean the symptom is “just anxiety,” and it does not mean you are weak. It usually means your personal threshold is lower, or other factors are piling on at the same time, such as poor sleep, illness, stress, stimulant use, dehydration, or an underlying rhythm tendency.
Your pattern matters.
If you notice that palpitations reliably cluster after drinking, treat that as useful information. If you have a wearable ECG, try to capture the rhythm while it is happening. That can give you something more concrete than a memory of “it felt weird,” and services like Qaly can help you review that tracing before your appointment so you can ask better, more specific questions instead of waiting in the dark.
Understanding the Different Types of Alcohol-Related Palpitations
A pounding heart after a drink can feel like one thing, but several different rhythm patterns can produce that sensation. The word palpitations only describes what you feel. It does not tell you which rhythm is happening underneath.
That distinction matters because a brief extra beat, a steady fast rhythm, and atrial fibrillation can all feel alarming, yet they raise different questions and lead to different next steps.
A fast but regular heartbeat
Sometimes alcohol does not create a chaotic rhythm. It pushes your heart rate up. You may notice this most when you are lying in bed, the room is quiet, and every beat suddenly feels louder than usual.
This pattern is often regular, like a drumbeat played too quickly. On a wearable ECG, the beats may still be evenly spaced, just closer together than your usual baseline. Alcohol can contribute indirectly here by nudging the body toward dehydration, lighter sleep, and higher stress-hormone output.

Skipped beats or extra beats
Many people describe this as a “flip-flop,” a thump, or a moment when the heart seems to pause. In many cases, the heart did not stop. An early beat arrived ahead of schedule, then a brief pause followed, and the next beat landed harder.
That sequence is easy to feel. It can happen with beats that start in the upper chambers or lower chambers, and it often shows up as one early beat interrupting an otherwise normal rhythm. These are often brief, but they can repeat enough times to make a person hyper-aware of every sensation.
-samsung.webp)
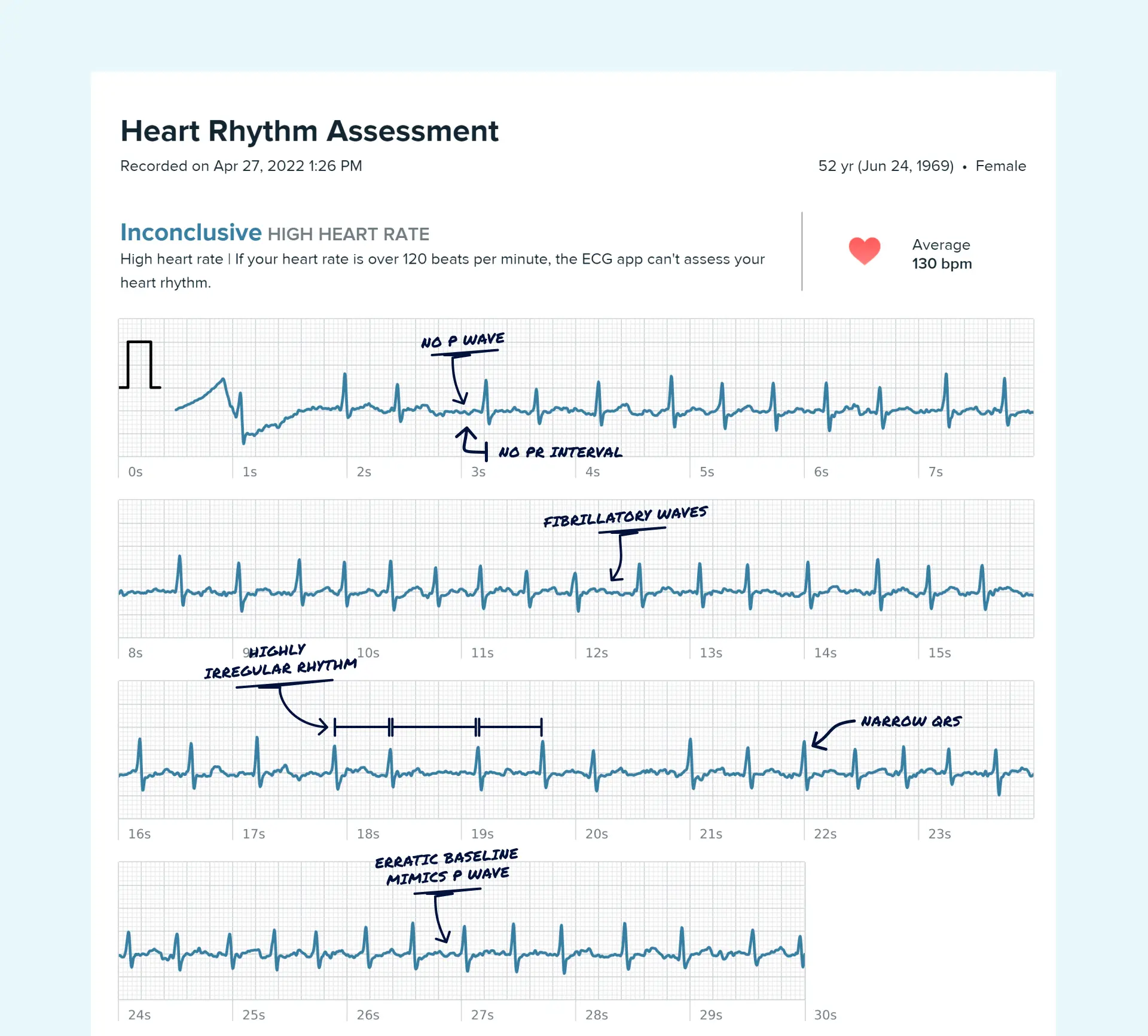
Atrial fibrillation
Atrial fibrillation, or AFib, is different. Instead of the upper chambers squeezing in an organized rhythm, they fire in a more disorganized way. The result is often an uneven pulse that feels irregular rather than just fast.
People often notice AFib as a heartbeat with no clear pattern. Fast, slow, pause, thump. It can feel random, and that unpredictability is part of what makes it unsettling.
If you use an Apple Watch or another wearable ECG device, learning what atrial fibrillation can look like on your watch ECG can make your recordings much more useful. Instead of telling your doctor, “something felt off,” you may be able to show the timing and rhythm of the episode and ask sharper questions. Services like Qaly can also help review those tracings so you are not left guessing alone while waiting for an appointment.
An irregular feeling is not automatically AFib. Anxiety, extra beats, and a fast regular rhythm can all feel dramatic too.
Why sorting this out helps
Your heart’s electrical system works like the timing system for an orchestra. If one musician comes in early, that is different from the whole group speeding up, and different again from the conductor losing the beat entirely. The sound changes in each case. So does the meaning.
That is why a wearable ECG can be so helpful. It cannot replace medical care, but it can turn a frightening, fuzzy memory into something more concrete. For people who already feel dismissed or told to “just monitor it,” having an actual tracing gives you something to bring into the room.
You may also notice other alcohol-related body signals around the same time, such as flushing, dry eyes, or irritation. Those symptoms do not diagnose a rhythm problem, but they can support the bigger picture that alcohol is affecting your system in a noticeable way. If that sounds familiar, see Nexus Recovery Centers on red eyes for another example of how drinking can show up outside the heart.
The goal is not to label every flutter yourself. The goal is to get clearer about the pattern so you can have a more informed conversation with a clinician, sooner and with less uncertainty.
How to Know When to Worry and Get Clear Answers
This is usually the biggest question. Not “Why did it happen?” but “Is this dangerous?”
The answer depends on what else is happening with the palpitations, how long they last, how often they recur, and whether you have a known heart condition. The feeling itself matters, but the full context matters more.
Get urgent medical help now if this is happening
Don't sit on symptoms that suggest something more serious. Seek urgent care or emergency evaluation if palpitations come with any of the following:
- Chest pain or pressure that doesn't quickly settle
- Fainting or near-fainting
- Severe shortness of breath
- Marked dizziness or confusion
- A feeling that you may pass out
- A sustained very rapid or very irregular rhythm that isn't calming down
These red flags don't guarantee a dangerous cause, but they deserve real-time medical assessment, not internet reassurance.
When it's reasonable to monitor and document
A different situation is the person who gets a short-lived flutter after alcohol, feels uncomfortable but stable, and is now trying to figure out whether this is a one-off or a pattern. That's where monitoring becomes useful.
If you've ever shown a doctor a symptom from memory and felt like the moment got lost in translation, you're not alone. Palpitations often vanish before the appointment. By the time you get seen, the ECG in clinic may be perfectly normal.
That's one reason wearable devices matter so much. A single-lead tracing from an Apple Watch, Fitbit, Kardia, Samsung watch, or Withings device can capture what your heart was doing during the episode, not days later when everything has settled.
What to record when an episode happens
You don't need a complicated system. Capture a few details consistently.
- Time and timing. Note when the palpitations started and whether they happened during drinking, before bed, or the next morning.
- Amount and pace. Write down what you drank and roughly how quickly.
- Symptoms around it. Include breathlessness, lightheadedness, chest discomfort, nausea, or anxiety.
- Your wearable ECG. Save the tracing if your device allows it.
- Context. Poor sleep, a salty meal, caffeine, stress, and dehydration can all matter.
This kind of pattern tracking gives you something far more useful than “I felt weird after wine once.”
The goal isn't to self-diagnose perfectly. The goal is to arrive at care with evidence instead of guesswork.
Why broader alcohol effects matter too
Alcohol doesn't only affect the heart. It can affect the eyes, sleep, hydration, mood, and blood vessels in ways that overlap with how you feel during a palpitation episode. If you've also noticed burning or bloodshot eyes after drinking, this resource from Nexus Recovery Centers on red eyes after drinking can help explain one more piece of the body's reaction.
For skeptical readers, that bigger picture matters. Sometimes traditional care fragments symptoms into separate boxes. But your body experiences alcohol as one whole-body stressor.
Bring your doctor data, not just a story
Doctors are often much more helpful when they can review timing, symptoms, and recordings together. That doesn't excuse rushed care, but it does improve the odds of a productive appointment.
A short note that says, “Palpitations started three hours after two drinks, lasted twenty minutes, wearable ECG recorded irregular rhythm, happened again the next weekend,” is much harder to dismiss than “Sometimes my heart feels funny.”
Steps for Immediate Relief and Long-Term Prevention
You can't always stop an episode instantly, but you can reduce the chaos around it. A calm, structured response helps you feel more in control and may reduce the things that are fueling the palpitations.
What to do right now
Start simple. Sit down. Loosen anything tight around your chest or neck. Try to breathe slowly instead of checking your pulse every few seconds.
Then work through the basics:
- Drink water. Small steady sips are often better than chugging.
- Stop alcohol for the rest of the day. More alcohol is not a fix.
- Skip stimulants. Hold off on caffeine, nicotine, and pre-workout products.
- Rest somewhere quiet. Lying on your left side makes some people more aware of their heartbeat, so adjust position if needed.
- Record the episode if your wearable ECG can capture it.
If you want a practical symptom-by-symptom approach, this guide on how to stop heart palpitations with relief tips is a useful companion.
How to prevent it next time
Here's the frustrating truth. Research still has a major gap regarding the details people really want, like whether beer differs from wine, whether food changes the timing, or whether drinking slowly changes the rhythm response. The Virginia Cardiovascular Specialists discussion of alcohol and AFib highlights that lack of granular guidance and points to personal tracking as the best way to identify your own triggers and patterns.
That means your prevention plan should be personal, not generic.
Build your own trigger map
Keep a note in your phone with a few repeat fields:
- What you drank
- How much
- How fast
- Whether you ate
- How you slept
- Whether palpitations happened
Over time, patterns often become obvious. Maybe it's not alcohol in general. Maybe it's drinking quickly on an empty stomach after a bad night of sleep.
Lower the overall strain
A few habits make episodes less likely:
- Hydrate before and after drinking
- Don't stack alcohol with heavy caffeine
- Avoid drinking when you're already exhausted
- Consider alcohol-free days
- Be honest about your threshold, even if it's lower than your friends' threshold
If your body repeatedly reacts to alcohol, the most heart-protective move may be cutting back sharply or avoiding it altogether.
If alcohol use is becoming hard to control
Some readers aren't dealing with an occasional social trigger. They're seeing more regular symptoms and realizing alcohol may be taking up too much space in their life. If that's where you are, don't quit abruptly without thinking through safety. This guide on safely stopping alcohol in Dallas explains why suddenly stopping can be risky for some people and why supervised help may be the better path.
That isn't a judgment. It's a safety issue.
Taking Proactive Control of Your Heart Health Journey
What started as a scary, confusing flutter doesn't have to stay a mystery.
By now, you know that heart palpitations after drinking alcohol can be a real physiologic response. Alcohol can disrupt fluid balance, irritate the heart's electrical timing, and trigger rhythm changes that are sometimes brief and sometimes more significant. You also know that not every palpitation means the same thing.
A better role for you in your own care
You do not have to be a passive patient who waits anxiously and hopes an episode happens at the exact moment someone is watching. If you wear an Apple Watch, Fitbit, Kardia, Samsung watch, or Withings device, you already have a tool that can help capture what your heart is doing in real life.
That doesn't replace a doctor. It makes your conversation with a doctor better.
The mindset shift that helps most
Think like a careful observer, not a panicked detective. Notice timing. Save recordings. Track patterns. Learn your red flags. Bring evidence.
When you do that, you move from “something scary happened to me” to “I know what happened, I documented it, and I'm ready to make informed decisions.”
Felt your heart race after a few drinks? Capture it on your smartwatch and upload the ECG to Qaly for a human-reviewed interpretation.










.png)
.png)