Key Takeaways
Prednisone can cause heart palpitations, and the risk appears to rise with dose. In a 2020 study, people taking less than 5 mg of prednisolone daily had twice the risk of heart disease compared to non-users, while those taking 25 mg or more daily had six times the risk.
You might be here because your heart suddenly feels fluttery, thumpy, too fast, or just "off" after starting prednisone. That can be scary, especially if you were told the medication would help one problem and now you're wondering whether it created another.
Your Guide to Understanding Prednisone and Your Heart
If you've noticed a racing heartbeat, a strange chest flutter, or a hard thump that seems to come out of nowhere after taking prednisone, your concern makes sense. Can prednisone cause heart palpitations? Yes, it can. For some people, it's a temporary side effect. For others, it can be a clue that their body is reacting strongly to the medication, the dose, dehydration, stress, or an underlying rhythm issue.
Palpitations don't always mean danger. But they do mean your body is worth listening to.
A lot of people feel stuck in an uncomfortable middle ground. The symptom feels real, but it may not happen during a clinic visit. A doctor may say, "Monitor it," while you're left wondering what that means at home. That's where a more practical approach helps. Not just "wait and see," but notice, record, compare, and communicate clearly.
Practical rule: A symptom you can capture is easier to understand than a symptom you can only describe from memory.
Prednisone can affect heart rhythm through several body systems at once. It can shift fluids, disturb minerals that help the heart fire correctly, raise blood pressure, and make you feel revved up or anxious. If you're already sensitive to stimulant-like sensations, that combination can feel intense.
This article is for the person who wants plain English, not hand-waving. If you're using an Apple Watch, Fitbit, Kardia, or another wearable ECG tool, you can do more than worry. You can gather useful information, spot patterns, and bring something concrete to your medical visit instead of saying, "It happened sometime last week."
Understanding Why Prednisone Affects Your Heart
Prednisone doesn't target only one body part. It acts more like a system-wide signal changer. That helps with inflammation, but it can also change how your heart feels and behaves.
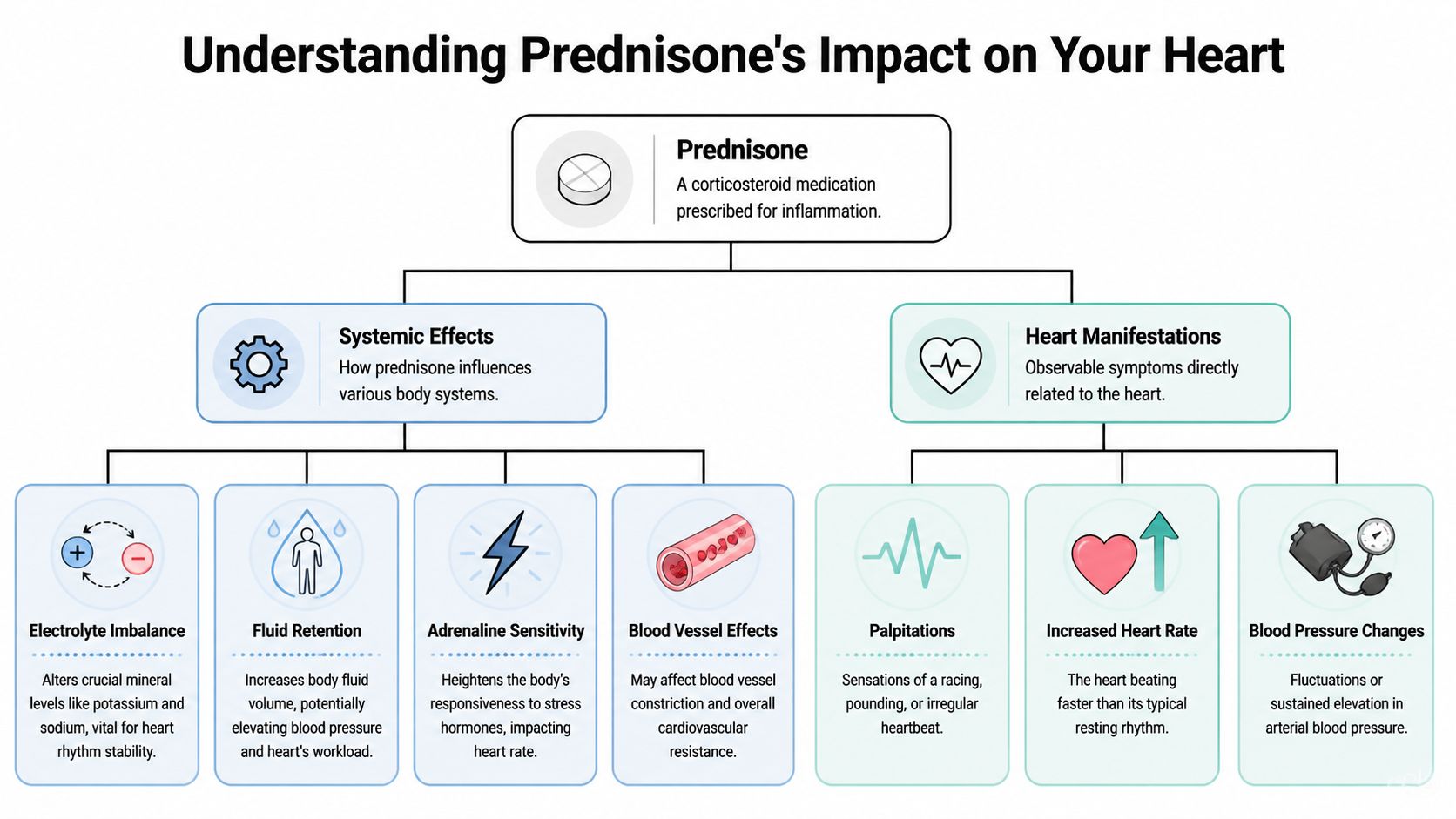
Your heart runs on timing and chemistry
Think of your heart like a carefully wired circuit. It needs the right electrical signals, the right fluid balance, and the right mineral levels to beat smoothly. Prednisone can interfere with all three.
One big issue is electrolytes, especially potassium. Potassium helps heart cells reset between beats. If those levels shift, the signal can become less steady, which can feel like fluttering, pounding, skipped beats, or a brief burst of rapid rhythm. If you want a simple explanation of why this matters, this article on potassium levels and the heart breaks it down clearly.
Prednisone can turn up the body's internal volume
Prednisone can also cause fluid retention and sodium-related changes. More fluid in the body can raise blood pressure and make the heart work harder. For some people, that feels like a stronger heartbeat. For others, it shows up as a faster heartbeat at rest.
It may also increase your sensitivity to stress hormones. So even if you're sitting still, your body can feel like it's in mild fight-or-flight mode. That can create the sensation of an internal buzz, jitteriness, or a pulse that suddenly feels louder than usual.
A dose-response pattern makes this more believable, not less. A 2020 study found that people taking less than 5 mg of prednisolone daily had twice the risk of heart disease compared with non-users, while those taking 25 mg or more daily had six times the risk, showing that risk rises with dose according to this review of the 2020 findings.
Your heart doesn't only react to disease. It reacts to pressure, fluid shifts, mineral changes, and stress signals.
Why this can feel confusing
Some people expect a heart side effect to feel dramatic, like movie-style chest pain. Palpitations are often subtler than that. They may come and go. They may be worse after a dose increase. They may show up at night when everything else is quiet.
If stress is also in the mix, the picture gets murkier. Some readers find it helpful to also learn how to balance cortisol levels naturally because stress and steroid effects can overlap in how they feel in the body, even though they aren't the same thing.
What Prednisone Palpitations Can Feel Like
People describe palpitations in very different ways. That's part of why they can be hard to talk about. You might say "my heart is racing," while someone else says "it feels like a fish flipping in my chest."
Common ways people describe it
Here are a few sensations that often fit:
- Fluttering: A light, shaky feeling in the chest or throat.
- Pounding: The heart feels extra forceful, even if it isn't wildly fast.
- Racing: Your pulse suddenly feels like you just ran upstairs.
- Skipping: A pause, then a heavy thump.
- Flip-flopping: An uneven, rolling sensation that comes in little bursts.
If you've been asking yourself whether what you're feeling "counts" as a palpitation, it probably does. The body doesn't always use textbook language.
Some people notice symptoms only when lying down. Others notice them after taking a dose, during a taper, when dehydrated, or when they're already emotionally keyed up. A wearable can help link that feeling to an actual rhythm strip instead of guesswork. If you want examples of how people describe these sensations, this guide on what heart palpitations feel like is useful.
The range can be wider than most people think
In more serious situations, rhythm changes can be dramatic. Hospital telemetry has recorded heart rates swinging between 35 and 160 beats per minute after corticosteroid exposure, as described in this discussion of prednisone-related palpitations and rhythm changes.
That doesn't mean every flutter is dangerous. It means the sensation deserves respect.
Some palpitations feel tiny but come from a real rhythm change. Others feel huge and turn out to be a brief, harmless surge. The feeling alone can't always tell you which is which.
That's why pattern matters. Is it brief or sustained? Random or tied to dosing? Regular and fast, or irregular and chaotic? The more specific you can get, the less helpless you feel.
Key Factors That Can Increase Your Risk
Not everyone taking prednisone will notice heart symptoms. The same dose can feel manageable for one person and miserable for another. Risk depends on your body, your history, and the context around the prescription.
Dose and duration matter
A larger dose usually puts more pressure on the systems that affect heart rhythm. The same goes for staying on prednisone longer, especially if side effects are building in the background instead of appearing all at once.
Some people feel palpitations soon after starting. Others notice them after a dose increase, after several days of poor sleep, or during a taper when the body is adjusting again. If your symptoms changed when the prescription changed, that's worth paying attention to.
Your baseline heart health matters too
If you already have high blood pressure, a rhythm disorder, or another heart condition, prednisone may be more likely to aggravate what was already there. The medication can add fluid strain, raise pressure, and make rhythm stability more fragile.
Even if you don't have a diagnosed heart condition, you may be more sensitive if you tend to react strongly to caffeine, stress, poor sleep, or dehydration. Some bodies are less forgiving when several triggers pile up at once.
Other medications and body stressors can pile on
Palpitations rarely happen in a vacuum. A few factors that can make them more likely include:
- Other stimulant-like inputs: Caffeine, decongestants, energy drinks, and some over-the-counter medications can raise heart rate or make you feel more wired.
- Fluid loss: If you're not drinking enough, your heart may compensate by beating faster or more noticeably.
- Sleep disruption: Prednisone can make sleep harder, and poor sleep lowers your tolerance for both stress and body sensations.
- Anxiety symptoms: Even when anxiety isn't the original cause, it can amplify the awareness of each heartbeat.
This isn't about blaming you for a side effect. It's about spotting which knobs may be turned up at the same time.
Is It The Prednisone or Something Else?
It's fair to question the obvious answer. Sometimes prednisone is the main driver. Sometimes it only exposes a problem you were already at risk for. Sometimes the medication causes anxiety or poor sleep, and those lead to the pounding feeling you're noticing.
A few common look-alikes
Prednisone-related palpitations can overlap with symptoms from:
- Caffeine
- Dehydration
- Panic or anxiety
- A separate arrhythmia that happened to be noticed now
- A drop in fitness during illness or recovery
- Fever, pain, or inflammation itself
That overlap is why it helps to think like a detective instead of picking one explanation too early.
Clues that point toward prednisone
Prednisone moves higher on the suspect list if the timing lines up. Maybe the fluttering started soon after a new prescription. Maybe it got stronger with a dose increase. Maybe it settles when the dose is lowered, or when you hydrate, rest, and avoid other triggers.
Anxiety can complicate this. Prednisone can make some people feel restless, edgy, or internally sped up. If panic symptoms are mixed in, learning a few calming tools can help you separate a stress surge from a rhythm problem. Some readers may find this DeTalks guide on panic management helpful alongside symptom tracking.
If the story in your body is messy, collect timestamps. Timing often reveals what memory blurs.
The key isn't to prove you're right on the first try. It's to gather enough information to narrow the field. When did it happen? How long did it last? What had you eaten, drunk, or taken? Were you resting, walking, anxious, or trying to sleep? Those details matter more than many realize.
Using Your Wearable ECG to Track Symptoms
Worry can turn into something useful. If you have an Apple Watch, Fitbit, Samsung Watch, Kardia device, or another wearable ECG tool, you don't have to wait for a clinic appointment to start documenting what your heart is doing.
What to capture in the moment
When you feel the symptom, try to do these things as calmly as you can:
- Sit or pause safely. Don't keep pushing through an episode if you're dizzy or unsettled.
- Check your wearable right away. If your device can record an ECG, start one during the sensation, not just after it passes.
- Log the context. Note the time, prednisone dose, hydration, caffeine, activity, and whether you felt anxious, short of breath, or lightheaded.
- Repeat if needed. If the feeling comes in waves, capture more than one reading.
A single rhythm strip can be surprisingly helpful. It may show a normal rhythm during a moment that felt scary, or it may catch something like extra beats or a brief run of a faster rhythm.
What a wearable can and can't tell you
Wearables aren't a replacement for emergency care, and they don't answer every question. But they can do something very important. They can connect symptom to timing.
Long-term prednisone use has been linked with a 15% incidence of palpitations and may show on an ECG as PR prolongation greater than 200 ms or QRS widening, according to this NIHR evidence summary on steroid-related cardiovascular risk. That matters because it shows why recording an ECG during symptoms can be more informative than just saying, "My heart felt weird."
If you're using an Apple Watch, this guide to an ECG app for Apple Watch can help you understand what you can record and review at home.
Turning raw data into something your doctor can use
A waveform screenshot is useful. A pattern across several recordings is better. What often helps most is a clear summary that says: these symptoms happened at these times, under these conditions, and these were the rhythms or intervals seen.
One option some wearable users choose is Qaly, which reviews wearable ECGs with certified cardiographic technicians and provides interval readings such as PR, QRS, and QTc, along with arrhythmia analysis from supported devices. That kind of summary can make a medical appointment more concrete, especially when the symptom didn't happen in the exam room.
Your Action Plan When You Feel Palpitations
When your heart starts acting strangely, the most helpful response is a calm, clear decision. Not every episode is an emergency. Some are. Knowing the difference can reduce panic and keep you from freezing.
If the symptoms feel dangerous
Get urgent medical help right away if palpitations come with chest pain, fainting, severe shortness of breath, or a rhythm that feels sustained and extreme. The same applies if you feel very weak, confused, or close to passing out.
A resting heart rate over 120 beats per minute or a clearly irregular rhythm can also be a sign that you shouldn't just watch and wait.
If the symptoms are uncomfortable but stable
If you're alert, breathing normally, and the episode passes or stays mild, use a home plan:
- Capture the rhythm: Record an ECG if your device allows it.
- Write down the details: Dose, timing, fluids, caffeine, sleep, and what the sensation felt like.
- Check basic contributors: Drink water if you may be dehydrated. Rest. Avoid more stimulants for the day.
- Review patterns: If symptoms repeat, collect several examples instead of relying on memory.
- Bring evidence to your appointment: A symptom log plus device recordings is far more useful than a vague summary.
Existing advice often misses this middle ground. People notice silent effects like low resting heart rates around 40 BPM or irregular rhythms during tapers, and those can be captured on consumer devices according to this discussion of prednisone and wearable-detected rhythm changes.
If anxiety becomes part of the cycle, support for both the mind and the heart can help. Some people also want to understand broader anxiety treatment options while they're sorting out whether a symptom is rhythm-related, stress-related, or both.
For a fuller checklist on escalation and timing, this guide on heart palpitations and when to see a doctor can help you decide what deserves urgent attention.
Frequently Asked Questions About Prednisone and Heart Health
Will the palpitations go away after I stop taking prednisone
Often, they improve after the dose is lowered or the medication is stopped, especially if prednisone was the main trigger. But don't assume every palpitation will disappear automatically. If symptoms continue, keep tracking them and let your clinician know. A medication side effect can overlap with a separate rhythm issue.
Can hydration or food choices help while I'm taking prednisone
They can help in some cases. Dehydration can make the heart feel more reactive, and poor intake can make you feel weaker, shakier, or more aware of each beat. Drinking enough fluids, being cautious with caffeine, and eating in a steady, balanced way may reduce the intensity of symptoms for some people. If your care team has given you diet restrictions, follow those first.
My watch flagged a slow heart rate too. Can prednisone do that
Yes, it can happen. People often think only of a fast heartbeat, but some users notice unusually slow rates while on prednisone or during a taper. A low reading isn't always dangerous, but it deserves attention if it comes with dizziness, weakness, fainting, confusion, or a strong sense that something is wrong.
A wearable alert is not a diagnosis. It's a prompt to look closer, especially when it matches how you feel.
The reassuring part is that you don't have to choose between brushing it off and rushing into panic. You can document what happened, compare episodes over time, and bring something specific into your next medical conversation.
If you're trying to figure out whether prednisone is behind your palpitations, Qaly can help you make sense of wearable ECG recordings you capture at home










.png)
.png)