Key Takeaways
Hello Heart Hero. If you've ever felt that unsettling flutter, skip, or racing beat in your chest, you know how alarming heart palpitations can be. You’re not alone, and it’s completely understandable to feel concerned, especially when the healthcare system can feel slow to provide clear answers.
So, let's get right to it: yes, a lack of vitamin B12 can absolutely be a cause of heart palpitations.
Your Guide to Understanding Heart Palpitations
This guide is here to explore a frequently overlooked cause of those unnerving chest flutters: vitamin B12 deficiency. Think of your heart's rhythm like a skilled orchestra drummer; palpitations are like the drummer suddenly losing their rhythm, creating a jarring, out-of-sync beat. While frightening, these sensations often stem from manageable issues, and knowledge is the first step toward finding a solution.
We understand the frustration that comes with seeking answers for symptoms that are often dismissed or hard to pin down. Many people feel unheard when they describe these sensations, which is why we're taking a deep dive into the connection between vitamin B12 and heart health. You're taking a proactive step just by researching this, moving beyond waiting rooms and toward empowerment.
The Hidden Link Between B12 and Your Heartbeat
The link between vitamin B12 and heart palpitations isn't just a vague theory; it's rooted in how your body produces energy and delivers oxygen. When B12 is in short supply, it can trigger a chain reaction that directly impacts your heart.

Heart palpitations can strike unexpectedly, sometimes feeling like a serious arrhythmia you might see on a wearable ECG. But often, a hidden culprit is a vitamin B12 deficiency causing a specific type of anemia.
Here's how it works: A B12 shortage leads to a condition called megaloblastic anemia. This slashes the production of healthy red blood cells, which are crucial for carrying oxygen. To compensate for the lack of oxygen-rich blood, your heart has to work overtime, sometimes beating up to 20-30% faster in severe cases. This rapid heart rate (tachycardia) is the body's scramble to get oxygen to your vital tissues, and you feel it as palpitations. This is why for many, symptoms like palpitations go hand-in-hand with fatigue and weakness. You can learn more about how B12 deficiency anemia causes these symptoms from Medical News Today.
The feeling isn't "all in your head." It's a real, physical signal from your body that something is out of balance. Your heart is working harder to make up for a nutritional shortfall, and that extra effort is what you feel as palpitations.
This guide will walk you through everything you need to know, helping you understand:
- Why your body needs vitamin B12 for a steady heart rhythm.
- How to identify symptoms that point toward a B12 issue.
- What steps you can take to investigate the root cause.
Our goal is to give you the clarity and confidence to have more informed discussions with your doctor and to take control of your heart health journey, starting today.
How B12 Deficiency Affects Your Heart Rhythm
It’s incredibly frustrating to feel your heart flutter or race, know something isn't right in your body, and then be told all your tests look normal. Let's connect the dots and explore the science behind why a shortage of vitamin B12 can throw your heart's rhythm off kilter.
Think of your body as having a sophisticated factory that produces red blood cells. Vitamin B12 is one of the most essential workers on that assembly line. When you don't have enough B12, the whole production process sputters and breaks down. The factory starts making fewer red blood cells, and the ones it does manage to produce are oversized, poorly formed, and can't do their job properly.
This condition is called megaloblastic anemia. These abnormally large red blood cells, known as megaloblasts, simply can't carry oxygen as efficiently as healthy, normal-sized ones. It's like sending out delivery trucks that are too big to navigate the narrow city streets; they fail to deliver their precious cargo of oxygen to your tissues and organs.
The Oxygen Shortage and Your Heart's Response
When your body's tissues are starved for oxygen, your heart gets an urgent signal to step up. It's an all-hands-on-deck emergency. In response, your heart kicks into overdrive, beating faster and harder to push what little oxygen is available through your bloodstream.
This faster-than-normal heart rate is known as tachycardia. That forceful, rapid, or fluttering feeling is exactly what you experience as vitamin b12 and heart palpitations. Your heart isn't malfunctioning; it's compensating for a critical supply-chain problem elsewhere in your system. It's working heroically to keep everything running despite the oxygen deficit.
The Homocysteine Connection
But there's another important piece to this puzzle: an amino acid called homocysteine. Vitamin B12 helps process and break down homocysteine, keeping its levels in a healthy range. When B12 is missing in action, this "supervisor" is off the job.
Consequently, homocysteine levels can start to climb, and high levels are bad news for your cardiovascular system. Elevated homocysteine can damage the delicate lining of your blood vessels, causing inflammation and making them less flexible. This vascular stress can, in turn, contribute to heart rhythm disturbances and other problems.
It’s a two-pronged attack: the anemia forces your heart to beat faster, while high homocysteine levels stress your blood vessels. Both pathways underscore why maintaining adequate B12 is so vital for a steady, reliable heartbeat.
And this isn't some rare, obscure issue. Globally, B12 deficiency affects a significant portion of the population, ranging from 6% in some groups to as high as 20% in older adults. What's more concerning is that it’s often overlooked, especially if a standard blood test shows "normal" B12 levels but more sensitive markers like homocysteine aren't checked.
Why Standard Tests Can Be Misleading
This brings up a critical point that resonates with so many people who feel their symptoms are being dismissed. You can have all the signs of B12 deficiency, including heart palpitations, yet have a blood test come back in the "low-normal" range. This is because a standard serum test measures the total amount of B12 in your blood, not the amount that is actively available for your cells to use.
It's a crucial distinction and a common source of frustration. Your body might have B12 floating around in your bloodstream, but if it can't get inside the cells where the real work happens, you'll still experience the symptoms of a deficiency. This is why a complete picture is so important. While you're learning about vitamin B12, you might find it useful to also explore our guide on how vitamin D can affect heart palpitations too. Understanding these connections empowers you to ask better questions and advocate for more thorough testing.
Identifying the Cause of Your Chest Flutters
We've talked about how a vitamin B12 shortage can directly lead to heart palpitations by making your heart work overtime. But when you feel that startling flutter, pound, or skip in your chest, it's only natural to wonder, "Is it really B12, or could it be something else?" That uncertainty can easily spike your anxiety, especially when you feel like you're not getting clear answers about what's happening inside your own body.
Feeling uncertain is completely normal. The sensations you're having are very real, and figuring out what they might mean is the first step toward getting some peace of mind. Let’s gently unpack what these palpitations can feel like and explore what else might be behind them.
Palpitations often show up in a few distinct ways:
- A Flutter: This feels like a brief, quivering sensation, almost like a butterfly is trapped in your chest.
- A Pound: A sudden, hard thump that can feel like your heart is smacking against your ribs.
- A Racing Sensation: Your heart suddenly speeds up for no apparent reason, as if you just ran a sprint while sitting perfectly still.
- A Skipped Beat: You might notice an unnerving pause, often followed by a more forceful beat as your heart gets back in rhythm.
It’s important to remember that while vitamin b12 and heart palpitations are linked, other conditions can cause these exact same feelings. The goal here isn't for you to self-diagnose, but to give you the knowledge you need for a more productive conversation with your doctor.
Exploring Other Potential Causes
One of the most common mimics is anxiety. A racing heart is a classic symptom of both anxiety and panic attacks. This can create a frustrating cycle where the physical sensation fuels more worry, which in turn makes the palpitations even worse. Many people find it helpful to understand this connection, and you can learn more about it in our dedicated guide on how anxiety can cause heart palpitations.
Beyond anxiety, several other physical issues can set off these chest flutters. These are often missed in a quick check-up but are critical pieces of the puzzle.
Your body is an interconnected system. A problem in one area, like your gut's ability to absorb nutrients or your body's mineral balance, can send ripple effects straight to your heart's rhythm.
Other potential culprits include:
- Thyroid Imbalances: Both an overactive thyroid (hyperthyroidism) and an underactive one (hypothyroidism) can mess with your heart rate and trigger palpitations.
- Electrolyte Disruptions: Your heart's electrical system depends on a precise balance of minerals. Low levels of potassium or magnesium can interfere with its ability to beat steadily.
- Other Types of Anemia: While B12 deficiency causes one type of anemia, a lack of iron can do the same. Iron-deficiency anemia also lowers your blood's oxygen-carrying capacity, forcing your heart to pump faster and harder to compensate.
Knowing that there are many possible causes can be incredibly reassuring. It confirms that what you're feeling is real, but it also shows that many non-cardiac issues can feel just like a heart problem. This knowledge arms you with specific questions to ask your doctor and helps you advocate for a more thorough investigation, moving you from a place of uncertainty to empowered action.
A Practical Plan for Investigating Your Palpitations
When your heart is doing things that feel scary and unpredictable, it's easy to feel anxious. But having a clear, practical plan can replace that anxiety with action. This section is your roadmap for getting to the bottom of your palpitations, putting you in control of your health journey.
It's absolutely crucial to work with a healthcare professional. However, walking into that conversation prepared with good information makes a world of difference. Remember, you're the expert on your own body, and your insights are vital.
Starting the Conversation with Your Doctor
If you think there might be a connection between your vitamin B12 levels and heart palpitations, your journey will likely start with some specific lab work. Don't hesitate to ask your doctor to explore this angle directly. A great resource to check out beforehand is this guide on what to expect from a B12 blood test.
To get the full picture, your doctor will probably order a few different blood tests. Here’s what they are and why each one is important:
- Complete Blood Count (CBC): This is a fundamental test that looks at the number, size, and health of your red blood cells. It’s the main way to spot anemia, a condition where your heart has to work overtime because there aren't enough cells to carry oxygen.
- Serum Vitamin B12 Test: This test measures the total amount of B12 floating in your blood. It's a decent starting point, but it can sometimes be misleading. It’s possible to have "normal" levels on this test but still have a functional deficiency where your body can't actually use the B12 it has.
- Methylmalonic Acid (MMA) and Homocysteine Tests: These are the key players for sniffing out a hidden B12 deficiency. When your cells are starved for usable B12, the levels of MMA and homocysteine in your blood go up. Elevated levels of these markers are a much more sensitive sign of a true deficiency than the standard B12 test alone.
If your first B12 test comes back in the "normal" range but you're still having symptoms, asking for MMA and homocysteine tests is a smart and proactive next step. It shows your doctor you're engaged and advocating for a thorough investigation.
Taking an Active Role with At-Home Monitoring
The waiting game for answers can be incredibly stressful. The good news is, you don't have to just sit and wait. You can take an active role by monitoring your heart at home and capturing real data. This turns a vague symptom into concrete evidence you can share.
Modern wearables are fantastic tools for this. Devices like an Apple Watch, Fitbit, or KardiaMobile can record a single-lead electrocardiogram (ECG) the moment you feel a palpitation. This is a game-changer. Palpitations are often fleeting and rarely show up on command during a quick doctor's visit. For more information, check out our guide on choosing a portable electrocardiogram monitor.
This technology empowers you to catch the event as it happens. Instead of just saying you felt a flutter, you can show your doctor the actual ECG recording of what your heart was doing at that exact moment. This completely changes the conversation.
But what do you do with that squiggly line from your watch? That's where a service like the Qaly app comes in. The app acts as a bridge, letting you send your ECG from your wearable device straight to a certified human expert for analysis, 24/7. In minutes, you receive a verified interpretation of your heart rhythm, turning raw data into a clear report. This provides both immediate peace of mind and a professional analysis you can confidently take to your next appointment.
Your Recovery Path From B12-Related Palpitations
If your investigation points to low vitamin B12 as the culprit behind your heart palpitations, you’ve already won a major part of the battle. Pinpointing the cause is a huge step forward, and thankfully, the path to feeling better is often straightforward and very effective. This part of the journey is all about replenishing your body's B12 stores and giving your heart the support it needs to find its steady rhythm again.
We get it; hearing you have a deficiency can feel overwhelming. But this is where real hope begins. The solution isn’t some complex, uncertain procedure; it’s about giving your body a nutrient it’s been desperately missing.
Choosing the Right Form of B12
When it comes to boosting your B12 levels, you have a few excellent options. The best choice for you will hinge on why you became deficient in the first place, something you and your healthcare provider can figure out together.
Here are the most common ways to get your B12 levels back up:
- Oral Tablets or Capsules: These are a great starting point if your deficiency is mild and likely tied to your diet. They’re easy to find and simple to take.
- Sublingual Drops or Tablets: These dissolve right under your tongue, letting the B12 absorb directly into your bloodstream. This is a smart move if you have issues absorbing nutrients in your gut.
- Vitamin B12 Injections: For severe deficiencies, pernicious anemia, or significant digestive problems that block absorption, injections are the gold standard. They deliver B12 right into the muscle, guaranteeing 100% bioavailability.
Setting Realistic Expectations for Recovery
It’s completely normal to want your palpitations to stop yesterday. But it’s important to see this as a journey, not an instant fix. Think of it like refilling a reservoir that has run completely dry; it takes time for the water level to rise and for the whole ecosystem to bounce back.
Once you start supplementation, your body gets to work making new, healthy red blood cells. Over the next several weeks to a few months, as your red blood cell count normalizes, your blood's ability to carry oxygen improves dramatically. Your heart will no longer need to work in overdrive, and the palpitations should start to ease up.
You might notice your energy and mental clarity improving first, sometimes within just a few weeks. The palpitations might take a little longer to resolve completely as your cardiovascular system adjusts to its new, healthier state. Be patient and kind to yourself during this process.
The Importance of Follow-Up and Finding the Root Cause
Starting B12 treatment is a huge first step, but following up is just as crucial. Your doctor will likely want to recheck your B12 levels and your complete blood count after a few months to make sure the treatment is working and your levels are where they should be.
Beyond just fixing the deficiency, it’s essential to understand why it happened. Was it a dietary choice, like a vegan or vegetarian diet without proper supplementation? Could it be a digestive issue like Crohn's or celiac disease? Or is it pernicious anemia, an autoimmune condition that requires lifelong B12 treatment?
Answering this question is the key to your long-term health. It ensures you have a permanent strategy in place, preventing your levels from dropping again and keeping those palpitations from coming back. This is your roadmap to lasting relief.
What Else Your Wearable ECG Can Uncover
While a vitamin B12 deficiency is a critical piece of the puzzle, it’s good to know that your wearable ECG is a powerful tool for understanding your heart's complete electrical health. Think of it this way: if your heart's electrical system is like a house's wiring, a B12 deficiency might cause a "brownout" (like anemia-induced tachycardia), but there could be other wiring issues your device can spot, too.
An ECG translates your heart’s electrical signals into a visual line graph, showing exactly how it's beating in real-time. This is incredibly empowering. It helps you move from just feeling a flutter to capturing what that flutter actually is.
Looking Beyond B12-Related Palpitations
A low B12 level can absolutely show up on your ECG. In fact, studies suggest that when B12 levels drop below a certain threshold, around 253 pg/ml, it can cause changes on an ECG that point to a higher risk for arrhythmias, even in otherwise healthy people. The deficiency can disrupt how the heart muscle "recharges" between beats. You can read the full research about these B12 and ECG findings to learn more.
However, palpitations can also come from common arrhythmias that have nothing to do with B12. This is where a service like Qaly becomes so helpful; it's designed to have certified technicians analyze your wearable ECGs so you and your doctor can tell the difference.
Here are a few other rhythms your ECG can help identify:
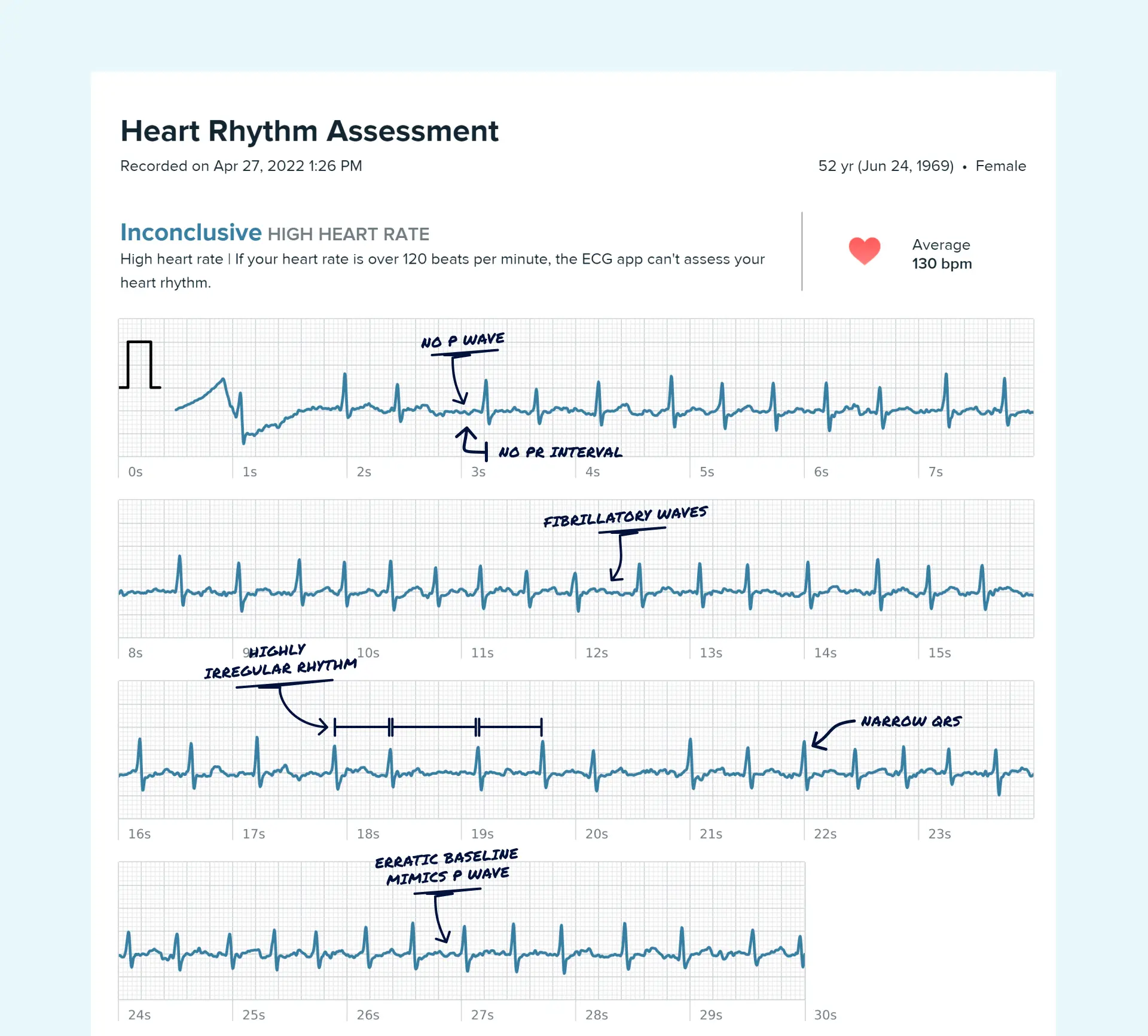
- Atrial Fibrillation (AFib): This is when the heart's upper chambers (the atria) beat chaotically, out of sync with the lower chambers. People often describe it as a rapid, irregular, or "quivering" heartbeat.
- Supraventricular Tachycardia (SVT): This is a very fast but regular heart rhythm that starts in the upper chambers. It can feel like someone suddenly "flips a switch," causing your heart to race, and then it stops just as abruptly.
-apple.webp)
- Premature Ventricular Contractions (PVCs): These are extra, abnormal heartbeats that begin in the ventricles (the lower chambers). They often feel like a "skipped beat" followed by a strong, noticeable thump.
-kardia.webp)
Knowing what is happening inside your body provides peace of mind. The purpose of monitoring isn't to create alarm but to provide clarity. Having an expert look at your ECG helps you know if what you're feeling is a benign flutter or something that needs a doctor’s attention.
Catching these rhythms early is key. It allows you to have a much more specific and productive conversation with your doctor. Instead of just describing a feeling, you can show them a professionally interpreted ECG report, turning your wearable from a gadget into a proactive health tool. If you're seeing extra beats on your watch, our guide on how to identify ectopic beats on your Apple Watch ECG can provide more helpful insights.
Frequently Asked Questions
When you're dealing with something as unsettling as heart palpitations, it's natural to have a lot of questions swirling around. Getting clear, straightforward answers is a huge part of feeling in control. We've put together some of the most common questions we hear about the link between vitamin B12 and heart palpitations to give you the clarity you're looking for.
How Quickly Will B12 Supplements Stop My Palpitations?
If a B12 deficiency is the only thing causing your palpitations, you could start feeling better within a few weeks to a couple of months. As your body rebuilds its supply of healthy red blood cells, your heart won't have to work so hard to circulate oxygen. This means the palpitations should gradually start to fade.
That said, everyone's body is different. The exact timeline really depends on how severe your deficiency is and how well your body absorbs the supplement. It's so important to stick with the plan your doctor lays out and keep a close eye on your symptoms.
Can I Have a B12 Deficiency If My Blood Test Was Normal?
Yes, you absolutely can. This is a common and incredibly frustrating experience for many people. A standard serum B12 test can be misleading because it measures the total amount of B12 floating around in your blood, not what's actually available for your cells to use.
This is what's known as a "functional" deficiency. Your blood test might look 'normal' on paper, but your body can still be starved for this vital vitamin. This is why many doctors now look at more sensitive tests.
To get a truer picture, they often check for high levels of methylmalonic acid (MMA) and homocysteine. These substances build up in your blood when your body can't properly use B12. If you still suspect a deficiency despite a normal test, asking your doctor about these more specific markers is a great next step.
Is Taking B12 Supplements Without a Doctor's Advice Safe?
Since vitamin B12 is water-soluble, your body typically just flushes out any extra it doesn't need. Because of this, it's generally considered safe for most people.
But, and this is a big but, you should always talk to a healthcare professional before starting any new supplement. If you self-treat the issue of vitamin b12 and heart palpitations, you risk masking another, potentially more serious, reason for your symptoms. A doctor can confirm the diagnosis, figure out the right dose and form of B12 for you, and make sure nothing else is being missed.
Wondering if it's an irregular heartbeat? On the Qaly app, human experts will interpret your ECGs for PAC, PVC, and PJC within minutes. Get started today.










.png)
.png)