Key Takeaways
Hello Heart Hero.
You finally made it through surgery. You're home, trying to rest, and then your chest feels strange. Maybe it's a flutter. Maybe your heart seems to race for a few seconds. Maybe your watch throws up a rhythm alert right when you were starting to relax. That moment can make your mind spin fast.
If that's happening to you, your concern makes sense. Atrial fibrillation after surgery is real, common, and often confusing. Many people are told to focus on incision care, pain control, and walking. Far fewer get a simple explanation of what a new irregular heartbeat might mean once they leave the hospital.
Recovery is bigger than the surgical site. Your whole body is adjusting. If you're also working on rebuilding strength and confidence, these Peak Physical Therapy insights can help you think about recovery as a full-body process, not just wound healing. If your procedure involved the heart, this overview of post-heart-surgery complications can also give useful context.
A Guide for Your Post-Surgery Heart Concerns
One of the hardest parts of recovery is uncertainty. In the hospital, nurses watch monitors and check vital signs. At home, it's just you, your symptoms, and whatever your body decides to do at 2 a.m. That gap can feel unsettling, especially if you already have doubts about how smoothly care continues after discharge.
A lot of readers come to this topic with the same question. "Is this just stress, or is something actually wrong with my heart?" The answer isn't always obvious from the sensation alone. A skipped beat can feel dramatic and still be harmless. Atrial fibrillation can feel mild and still deserve prompt attention.
A strange heartbeat after surgery isn't something to ignore, but it also isn't a reason to panic. The goal is to notice it, document it, and respond clearly.
This guide is built for that middle ground. Not alarmist. Not dismissive. Just practical.
You'll see what atrial fibrillation after surgery is, why it happens, what symptoms matter, and how to think about monitoring once you're back home. The more you understand the pattern, the less power that uncertainty has over you.
What Is Post-Surgical Atrial Fibrillation
Think of your heartbeat as a concert with one conductor. In a normal rhythm, the conductor gives a clear cue, and each section of the orchestra comes in on time. Your heart's upper chambers, called the atria, contract in an organized way, then the lower chambers follow.
With atrial fibrillation, that clear cue gets replaced by many rapid, disorganized electrical signals. Instead of squeezing smoothly, the atria quiver. The lower chambers then receive irregular messages, so the pulse often feels uneven and sometimes fast.
What makes it post-surgical
When this happens for the first time around a surgery, clinicians often call it postoperative atrial fibrillation, or POAF. The key idea is that surgery can temporarily disturb the heart's electrical system, even when the heart muscle itself isn't failing.
That distinction matters. Many people hear "arrhythmia" and imagine their heart is permanently damaged. Usually, that's not the right picture. In many cases, this is better understood as an electrical disruption during a physically stressful time.
What it can feel like
Some people notice it immediately. Others don't.
Common descriptions include:
- Fluttering in the chest that feels like a fish flipping
- Racing heartbeat that seems out of proportion to activity
- Breathlessness during simple tasks like walking to the bathroom
- Weakness or fatigue that feels different from expected post-op tiredness
- Dizziness or a vague sense that something is off
Some episodes are silent. That's one reason wearable ECG tools have become so interesting for recovery. They can capture what you can't always describe. If you want to understand how doctors think about repeated episodes over time, this explanation of Afib burden is a helpful next layer.
Practical rule: Don't try to diagnose the rhythm from the feeling alone. Symptoms tell you something is happening. The ECG tells you what it is.
Why a Bumpy Heartbeat Can Happen After Surgery
It seems unfair. You may have had surgery on your knee, abdomen, or lungs, and now your heart is acting up. But your body doesn't recover in isolated compartments. Surgery sends stress signals through the whole system.
Inflammation can irritate the heart's electrical system
Surgery causes tissue injury, even when everything goes well. Your immune system responds with inflammation to help healing begin. That response is useful, but it can also make the heart's electrical pathways more irritable.
A review in Frontiers in Cardiovascular Medicine notes that post-operative atrial fibrillation often peaks on the second and third days after surgery, and that this timing matches the body's inflammatory response, with C-reactive protein peaking around 48 hours post-procedure in continuous ECG monitoring studies (Frontiers in Cardiovascular Medicine review).
That timing explains why some people feel fine right after surgery and then develop symptoms a bit later. The rhythm problem often follows the body's stress response, not the clock on the operating room wall.
Stress hormones and the nervous system play a role
Pain, anesthesia, poor sleep, and emotional stress all affect the autonomic nervous system. That's the system that helps regulate heart rate, blood pressure, and the balance between "fight or flight" and rest. After surgery, that balance can get messy.
When stress hormones rise, the heart may become more likely to slip into an irregular rhythm. This doesn't mean you caused the problem by feeling anxious. It means your body is navigating a heavy physiologic load.
Fluids, electrolytes, and medications can add friction
Surgery often changes hydration, salt balance, and medication use. Even small shifts can matter when the heart is already electrically sensitive.
A few examples that commonly confuse patients:
- Fluid changes: IV fluids, blood loss, or reduced appetite can all change how full the circulation is
- Electrolyte shifts: potassium and magnesium changes can make rhythm problems easier to trigger
- Medication effects: some drugs can speed the heart, slow it, or indirectly make irregular rhythms more likely
If you're wondering whether a medicine could be contributing, this guide to medications that cause atrial fibrillation can help you frame better questions for your clinician.
None of this means your recovery is going off the rails. It means the body after surgery can be a temporary "perfect storm" for rhythm changes.
Knowing Your Risk and Recognizing the Signs
Some people are more likely to develop atrial fibrillation after surgery than others. Knowing that isn't about labeling yourself as high risk. It's about understanding your body's context.
Who tends to be at higher risk
Risk tends to be higher in people with:
- Older age
- High blood pressure
- Obesity
- Heart failure or valve disease
- A history of atrial fibrillation
- An enlarged atrium or other underlying heart disease
The risk is especially relevant after cardiac procedures. After cardiac surgery, POAF is the most common complication and affects 20% to 50% of patients, and those who develop it have a 62% higher risk of stroke within 30 days and a 37% higher long-term stroke risk compared with patients without POAF (PMC review on POAF after cardiac surgery).
That sounds scary, but it should also clarify why clinicians pay close attention to this rhythm. It's not a minor nuisance.
What symptoms people notice
Patients often expect one dramatic symptom. Real life is messier.
You might feel:
- A pounding or racing heartbeat
- An uneven pulse
- Shortness of breath
- Lightheadedness
- Tiredness that feels different from normal recovery fatigue
- Chest discomfort or a vague sense of internal jitteriness
And sometimes, you feel nothing at all.
Silent atrial fibrillation is one reason some episodes are found on telemetry or wearable ECGs rather than from symptoms alone.
If you want a symptom checklist in plain language, this guide to heart arrhythmia symptoms is useful.
When to take symptoms more seriously
Call your care team promptly if the rhythm feels sustained, keeps returning, or comes with worsening breathlessness, faintness, or chest pressure. If symptoms are severe or sudden, seek urgent care.
A good rule is simple. New symptoms after surgery deserve attention. Repeated symptoms deserve documentation.
The Real Risks and What Doctors Do in the Hospital
The biggest concern with atrial fibrillation after surgery is stroke. When the atria quiver instead of squeezing well, blood can stagnate inside the heart. Stagnant blood can clot. If a clot travels to the brain, it can block blood flow and cause a stroke.
That risk is why medical teams don't treat atrial fibrillation as "just palpitations." They look at the rhythm itself, your heart rate, your blood pressure, your symptoms, and your bleeding risk after surgery. Those pieces guide treatment.
What the hospital team is trying to accomplish
Most hospital treatment follows a few goals:
- Slow the heart rate if it's too fast
- Restore normal rhythm in some patients
- Decide about blood thinners based on stroke risk and bleeding risk
- Watch for recurrence during the vulnerable early recovery period
Common treatments include beta-blockers to slow the rate, rhythm-control medicines in selected cases, and sometimes cardioversion if the situation calls for it. The exact plan depends on the surgery, the patient's stability, and how long the rhythm has been present.
Why hospitals take it seriously
New-onset POAF after cardiac surgery can extend hospital stays by an average of 3.7 days and independently double mortality risk, according to a review discussing Society of Thoracic Surgeons guidance and postoperative management (PMC review on new-onset POAF and STS guidance).
Those numbers explain the urgency without meaning that every patient will have a bad outcome. Many patients benefit from close monitoring and timely treatment. The main danger comes from missing the rhythm, underestimating it, or assuming it doesn't matter because it started after surgery.
Hospital mindset: control the rhythm problem, reduce stroke risk, and get the patient safely through the transition from monitored care to home.
Taking Charge of Your Heart Health After You Go Home
Going home is supposed to feel reassuring. Sometimes it does. Sometimes it feels like losing your safety net.
In the hospital, a monitor notices rhythm changes before you do. At home, the responsibility shifts back to you. For people who are already skeptical about how smooth follow-up care really is, that shift can feel uncomfortable. In fact, that skepticism isn't irrational.
Why home monitoring matters
A large 2022 study found that atrial fibrillation after non-cardiac surgery affected 13% of patients and was often undertreated, even though these patients had an equivalent long-term stroke risk to those with non-surgical Afib (Harvard Health summary of the 2022 study).
That finding matters because many patients are told, directly or indirectly, that post-surgical episodes are temporary and therefore less important. Sometimes they are temporary. That doesn't automatically make them harmless.
What taking charge looks like
This doesn't mean you need to become your own cardiologist. It means becoming a careful observer of your own recovery.
Useful steps include:
- Know your pattern: when palpitations happen, how long they last, and what else you notice
- Take medications exactly as prescribed: especially rate-control medicines and blood thinners if they've been ordered
- Capture rhythm data when possible: a watch ECG or portable ECG can be more useful than a memory of the sensation
- Bring concrete records to follow-up: dates, symptoms, and ECG strips help your clinician make better decisions
If you're also dealing with incision healing, mobility limitations, or discomfort around scar tissue, this practical Highbar PT's scar tissue guide can support the broader recovery picture.
The emotional side matters too
Many patients aren't just worried about stroke. They're exhausted by not knowing whether each flutter is dangerous. A good monitoring plan reduces guesswork. It doesn't eliminate uncertainty, but it turns vague fear into usable information.
How to Use Your Watch ECG to Monitor Your Heart
A smartwatch or handheld ECG device can be more than a gadget during recovery. Used well, it becomes a notebook for your heart rhythm.
What to look for on the tracing
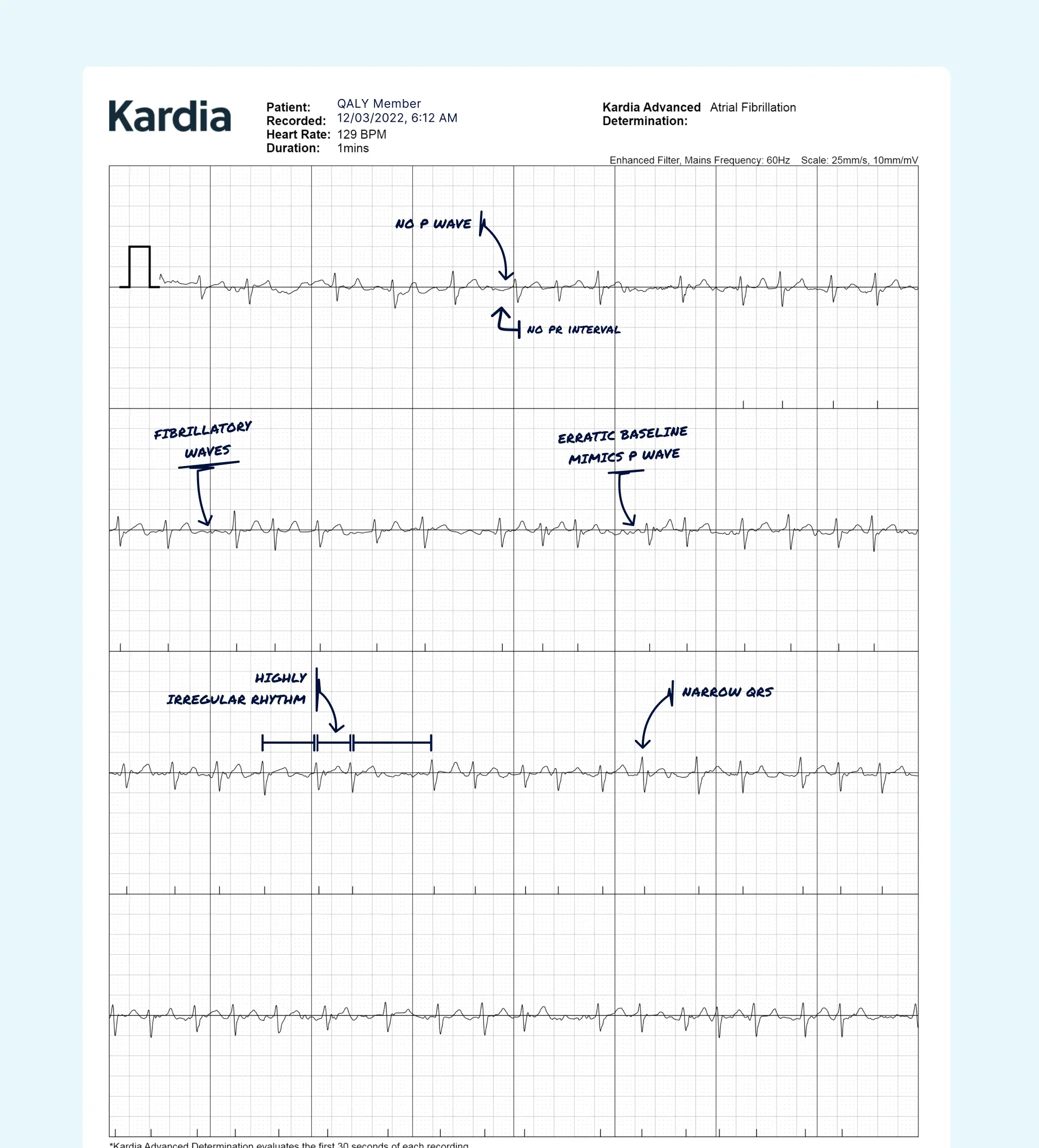
You do not need to become an expert reader to get value from a wearable ECG. Start with two practical signs that raise suspicion for atrial fibrillation:
- Irregularly irregular rhythm: the spaces between beats look random rather than rhythmic
- No clear repeating P waves: before each beat, you don't see the same organized little bump each time
That said, consumer ECGs are easy to misread. Movement, poor skin contact, muscle tension, and signal noise can all mimic something abnormal. That's why context matters. If the line looks chaotic because your hand was shaking, that isn't the same as true Afib.
How to record a useful ECG
A few basics make a big difference:
- Sit still for the recording
- Rest your arm on a table if you can
- Repeat the tracing if the first one is noisy
- Note your symptoms at that moment
- Save the ECG with the time and date
If your pulse feels odd for only a minute or two, record as soon as possible. The strip captured during symptoms is often the most valuable one.
How expert review helps
Raw data is helpful. Interpreted data is better.
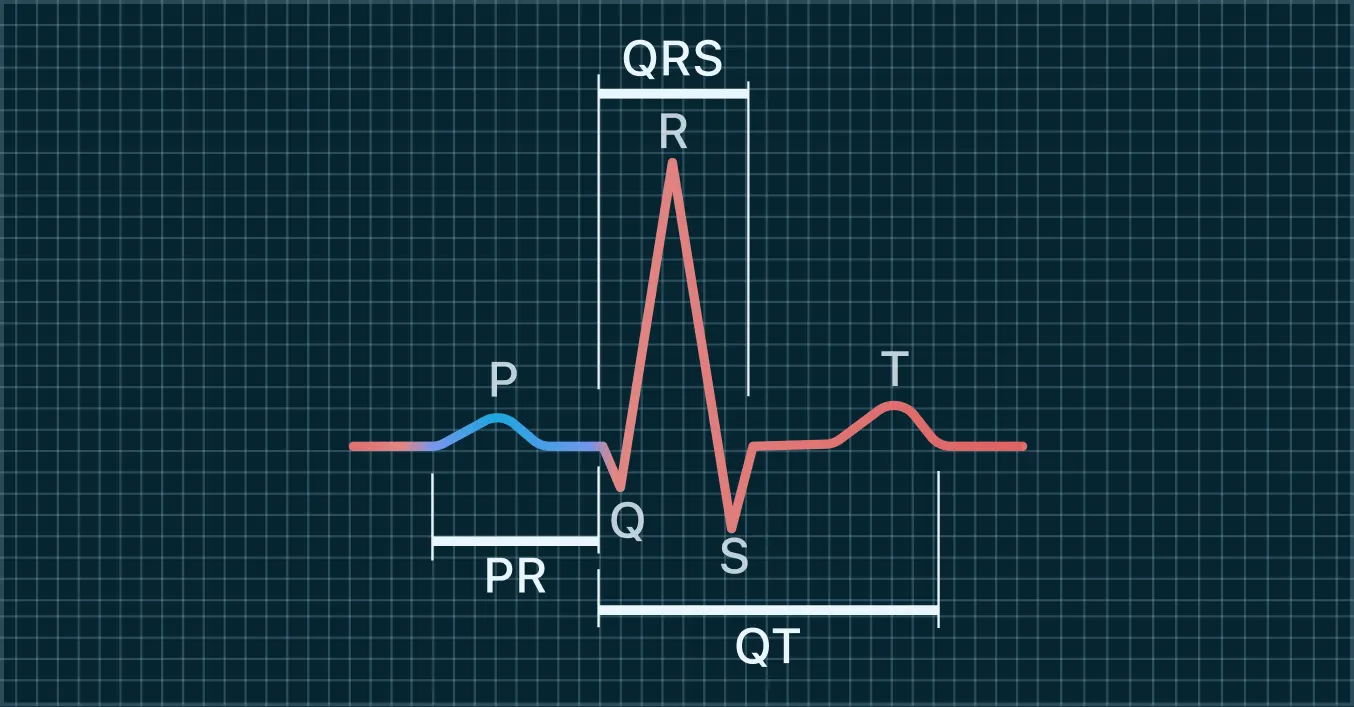
One option is Qaly, which lets people upload wearable ECGs from devices such as Apple Watch, Fitbit, Samsung, and Kardia for review by certified cardiographic technicians, with interval measurements like PR, QRS, and QTc included in the report. That kind of review can make it easier to tell the difference between artifact, benign extra beats, and a rhythm that deserves quicker medical follow-up.
If your watch flags something, don't treat the device as the final word. Treat it as a prompt to gather a clean tracing and get informed interpretation.
A simple habit works well for many patients. Record when symptoms happen. Save the tracing. Write one sentence about how you felt. Share those records with your clinician. That turns an anxious moment into evidence.
Don't guess at your readings. Have a certified technician review your ECG with Qaly.










.png)
.png)