Key Takeaways
Hello Heart Hero.
You may be reading this after a clinic visit that left you more alarmed than informed. A doctor said “advanced heart failure,” someone mentioned more testing, and now you're home trying to figure out what that means for your body, your future, and your family.
That moment can feel lonely. It can also stir up a lot of skepticism. If the healthcare system has ever felt rushed, fragmented, or hard to trust, you're not imagining that. Many people with heart failure feel like they have to fight for clear answers, timely referrals, and a care plan that fits real life.
You still have more power than it may feel like right now. Advanced heart failure is serious, but it is not a reason to give up your voice. It's a reason to use it more clearly, with better information, better tracking, and better questions.
Your Guide to Navigating Advanced Heart Failure
A common story goes like this. Someone has heart failure for a while, takes their medications, tries to watch salt, and pushes through fatigue. Then everyday tasks start getting harder. Walking across the room feels like a chore. Sleeping flat becomes uncomfortable. Swelling lingers. A doctor says the condition may be moving into a more severe stage.
That shift is more common than many people realize. Current estimates indicate that 5 to 7% of all patients with symptomatic heart failure have advanced heart failure, and within the U.S. heart failure population of 6.7 million Americans, that means hundreds of thousands of people are living with this severe stage according to HFSA heart failure epidemiology and outcomes statistics.
If you're here, you may be asking questions like these:
- What changed in my heart failure
- How serious is this
- What should I watch at home
- Do I need a specialist
- How do I know if my doctor is moving fast enough
Those are the right questions.
Important mindset: You do not need to become your own cardiologist. You do need to become an informed observer of your own body.
That means noticing patterns, documenting symptoms, and bringing usable information to appointments. For some people, that includes a notebook with daily weights and swelling notes. For others, it also includes data from wearables that capture rhythm changes when something feels off.
Advanced heart failure care often works best when patients and families stop being passive recipients of instructions and start acting like partners. Not confrontational partners. Informed ones. Calm, organized, persistent, and specific.
When you know what advanced heart failure means, what signs matter, and how doctors decide on next steps, the whole process becomes less foggy. That doesn't erase the fear, but it can reduce the helpless feeling that fear brings.
What Exactly Is Advanced Heart Failure
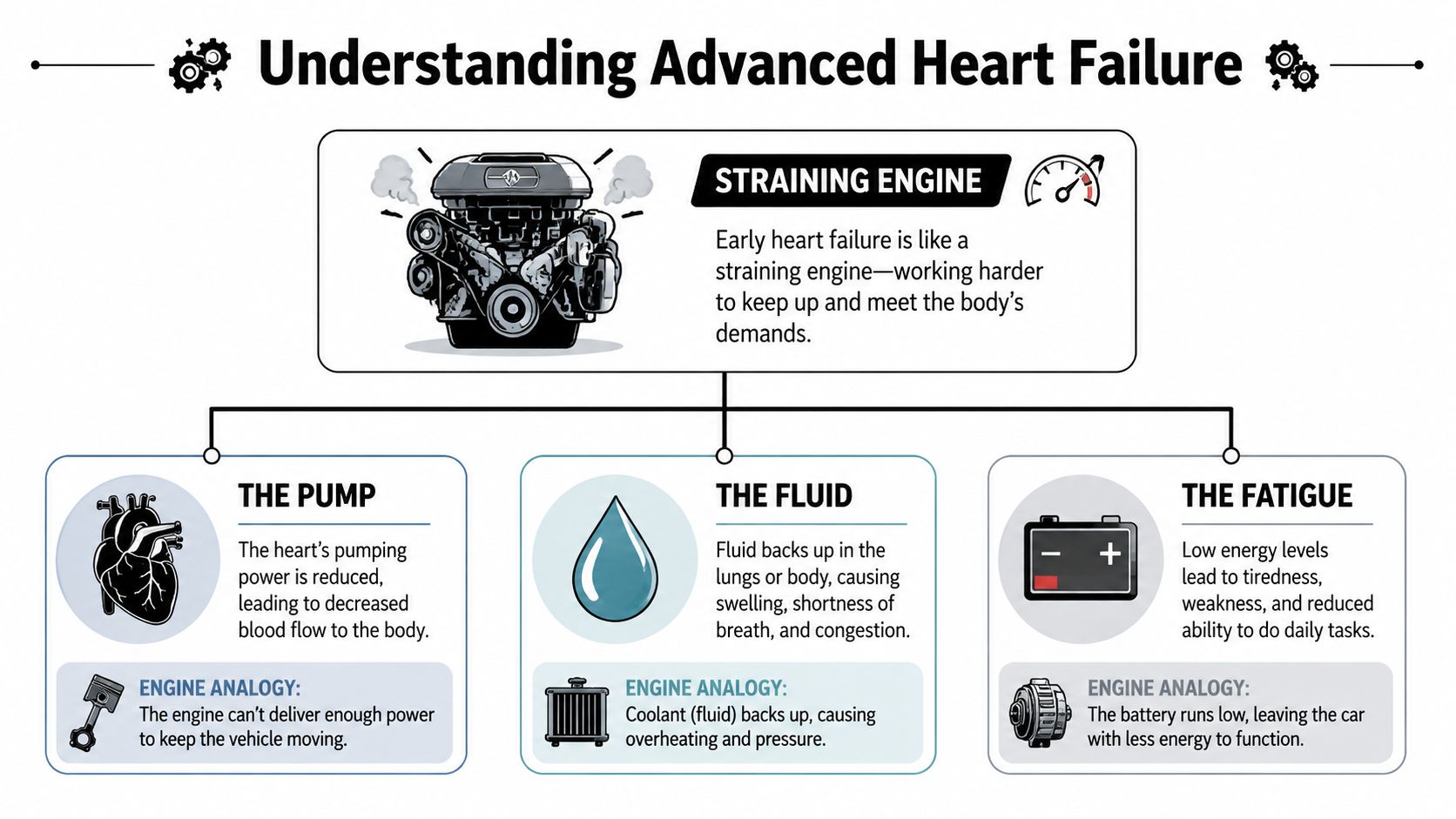
Think of your heart like a car engine that has been compensating for a problem for a long time. In earlier heart failure, the engine is strained but still manages to get the car up the hill with fuel, maintenance, and careful driving. In advanced heart failure, the engine is struggling even after the usual fixes have already been tried.
Doctors also call this Stage D heart failure. In plain language, it means the heart has structural problems and symptoms remain severe even though the person is already on the best tolerated standard treatments.
What the official definition means in real life
A practical definition from this clinical guide to identifying advanced heart failure says advanced heart failure is classified as Stage D by the ACC/AHA and involves severe resting symptoms, often NYHA Class III to IV, that continue despite maximally tolerated guideline-directed medical therapy. The same source notes that a 6-minute walk test distance of less than 300 meters is associated with short-term mortality and the need for advanced therapies.
That's a lot of medical language, so let's translate it.
- Stage D means standard treatment may no longer be enough on its own.
- NYHA Class III to IV describes how much symptoms limit daily activity. Class III usually means symptoms with small amounts of activity. Class IV can mean symptoms even at rest.
- Maximally tolerated therapy means your team has already tried the usual medications and treatments as much as your body can handle.
If you want a broader plain-language overview of how heart failure affects the body, this article on congestive heart disease can help connect the terms to symptoms people feel.
Why this stage feels different
Earlier in the disease, people often have “good days and bad days.” In advanced heart failure, the body has less reserve. Small stressors can hit harder. A salty meal, a medication change, an infection, or a rhythm problem can tip the balance more quickly.
The heart's trouble pumping forward can lead to fluid backing up. The reduced blood flow can also leave muscles, kidneys, and the brain with less of what they need. That's why the condition doesn't just feel like “being out of shape.” It can affect breathing, energy, thinking, sleep, and appetite.
A helpful way to think about it is this. The heart is no longer just working inefficiently. It's running out of backup options.
That's also why labels matter. They are not there to frighten you. They help doctors decide whether someone needs specialized evaluation for options beyond routine care.
Recognizing the Signs and Underlying Causes
Many people don't realize how much they've been adapting until symptoms become impossible to ignore. They stop taking stairs. They sleep propped up. They plan errands around fatigue. They call it “getting older” or “just a rough patch.”
Advanced heart failure often shows up through those lived experiences long before the words feel clear.
What your body may be telling you
A heart that can't keep up usually creates a pattern, not just one symptom.
- Breathlessness that lingers: You may feel short of breath walking short distances, lying flat, or sometimes even while resting.
- Deep fatigue: This is more than being tired after a busy day. It can feel like your body battery never recharges.
- Swelling: Fluid may collect in the legs, ankles, feet, or abdomen.
- Reduced stamina: A shower, getting dressed, or making a meal may leave you wiped out.
- Mental fog or poor appetite: When the body is under strain, concentration and appetite can slip too.
The “why” matters. If the heart can't move blood effectively, fluid can back up into the lungs or body tissues. At the same time, less oxygen-rich blood reaches muscles and organs. That's why you can feel both puffy and drained.
How to describe symptoms clearly to your doctor
Specific descriptions help more than broad ones. “I feel bad” is honest, but it doesn't guide care very well. Try language like this instead:
- “I need three pillows now to sleep comfortably.”
- “My shoes leave marks by afternoon.”
- “I get winded walking from the bedroom to the kitchen.”
- “I've stopped doing things I could do a month ago.”
That kind of detail gives your care team something they can act on.
Keep a short symptom log. Write down what happened, when it happened, and what you were doing at the time. Patterns are easier to spot on paper than from memory.
How people get to this stage
Advanced heart failure usually doesn't appear out of nowhere. It often grows out of earlier heart failure caused by problems such as coronary artery disease, prior heart injury, long-standing high blood pressure, heart muscle disease, or valve disease.
Sometimes people did everything “right” and the condition still progressed. That's important to say plainly. Progression is not proof that you failed. It means the disease has become more demanding and may need a different level of treatment and monitoring.
How Doctors Diagnose and Plan Your Care
A good advanced heart failure workup should feel like a decision process, not a mystery. Doctors are trying to answer two practical questions. How strained is the heart right now, and what kind of support is most appropriate next?
That process can feel overwhelming, especially if you've already had tests before. But each test serves a different purpose.
The main pieces of the workup
An echocardiogram shows how the heart is moving and pumping. It can help your team assess chamber size, valve function, and overall heart performance. If you want a simple explainer before or after your appointment, this guide to understanding your heart health is a helpful starting point.
A blood test for natriuretic peptides can give clues about how much strain the heart is under. Other bloodwork may look at kidney function, liver function, and related issues that shape treatment decisions.
An exercise assessment may be used to understand how limited your functional capacity has become. In some people, that includes a 6-minute walk test or a more formal cardiopulmonary exercise evaluation.
For a plain-language look at what happens during a heart ultrasound, this overview of a transthoracic echocardiogram can make the process less intimidating.
Clinic ECG versus wearable ECG
Many people find this stage confusing.
A 12-lead ECG in clinic is a medical snapshot. It gives a detailed, structured look at your heart's electrical activity at one moment in time.
A wearable ECG is different. It's not a replacement for a clinical ECG. It's useful because it helps capture what happens outside the office, especially when symptoms come and go. If you feel palpitations on Tuesday night but your appointment is next week, your wearable may help document what was happening in that moment.
Both have value. One is a high-detail snapshot. The other can be a running diary.
Why referral matters so much
Advanced heart failure care sometimes requires a treatment center with expertise in device therapy, advanced medications, or evaluation for options like LVAD or transplant. Referral delays can matter.
The process is not always equitable. According to the American Heart Association overview of advanced heart failure, underrepresented groups, including Black, Hispanic, female, and older patients, often face lower referral rates to advanced heart failure treatment centers, and some studies show Black adults are 30 to 50% less likely to receive devices like ICDs or CRT despite being eligible.
If that reality makes you uneasy, use it as motivation to be concrete and organized, not discouraged.
Here are useful questions to bring to an appointment:
- “Am I at the point where I should see an advanced heart failure specialist?”
- “What signs tell you I may need device therapy or another level of care?”
- “What test result are you waiting on before making that referral?”
- “If I worsen at home, what should trigger a same-day call?”
Good self-advocacy is not being difficult. It's making sure your symptoms, test results, and priorities are visible.
Your Active Role in Daily Health Management
Daily management can feel repetitive. Weigh yourself. Check swelling. Watch salt. Take medications. Do it again tomorrow. But these aren't just chores. They are some of the clearest ways to catch change early and protect your energy.
When people feel powerless, routine can feel insulting. When people understand what routine does, it becomes a tool.
Build a home system you can actually sustain
Most plans fail because they ask too much all at once. Keep it simple.
- Morning weight: Take it at the same time each day, in similar clothing, and write it down.
- Symptom check: Notice breathing, swelling, energy, sleep, and appetite.
- Medication cue: Tie pills to an existing habit like brushing your teeth or breakfast.
- Food environment: Make the lower-sodium option the easiest option in your kitchen.
A low-sodium eating pattern is easier when you stop relying on willpower alone. Stock ingredients you can combine quickly. Rinse canned beans if you use them. Flavor food with herbs, garlic, lemon, vinegar, onion, and salt-free seasoning blends instead of reaching for the shaker.
For meal ideas specifically designed with heart failure in mind, this guide to a low-sodium diet for heart failure can give you practical starting points.

Make support tools work for you
Some people with advanced heart failure are also prescribed oxygen or have questions about using it at home. If that applies to you, a plain-language medical oxygen guide can make the equipment side less confusing.
Your phone can also become part of your care routine. Use it for medication reminders, symptom notes, and a short list of emergency contacts and medication names.
A very practical home checklist looks like this:
- On the fridge: Medication list, pharmacy number, doctor number, emergency contact
- By the bed: Notebook for nighttime symptoms, especially breathlessness or palpitations
- On the phone: Recurring reminders for medications and daily check-ins
Why this matters emotionally too
Small daily actions don't cure advanced heart failure. They do something else that matters just as much. They reduce chaos.
When you can say, “My weight has been steady, but my breathing changed three days ago,” that's stronger than feeling scared and not knowing what changed. A calm record often gets taken more seriously than a vague description, and it helps you feel less at the mercy of every symptom.
Using Wearables for Proactive Heart Monitoring
Wearables are not magic, and they are not a substitute for medical care. They are tools. Used well, they can help you notice rhythm changes early, document symptoms clearly, and show your doctor what happened outside the clinic.
That matters because advanced heart failure doesn't always worsen on a neat schedule. Sometimes the first clue is that your rhythm seems different, your palpitations are more frequent, or you feel “off” in a way you can't easily explain.
What wearables can help you catch
According to UT Southwestern's discussion of advanced heart failure clues, palpitations or arrhythmias detected by devices like Apple Watch or Kardia can signal early decompensation in heart failure patients, and arrhythmias are known to precede 20 to 30% of heart failure exacerbations. The same source notes that tracking ECG interval trends with a service like Qaly can help flag this instability before it requires hospitalization.
That doesn't mean every alert is dangerous. It means rhythm changes can be one useful clue, especially if they line up with symptoms like breathlessness, dizziness, worsening fatigue, or reduced exercise tolerance.
Examples of changes worth documenting include:
- New irregular rhythm notifications
- More frequent skipped beats or pounding beats
- Episodes of fast heart rate that feel different from usual
- Changes that keep appearing alongside swelling or breathlessness
_apple.webp)
How to use wearable data wisely
The best approach is to treat your wearable like a logbook, not a judge.
If you record an ECG during symptoms, save the date, time, and what you were feeling. If your device or app provides interval data such as PR, QRS, or QTc, trend changes over time can make your follow-up visit more productive.
One option some wearable users choose is remote patient monitoring benefits, especially when they want their home data organized in a way that is easier to share with clinicians.
A useful script for your appointment might be:
- “I had palpitations on three days this week, and I recorded them.”
- “These episodes happened when I was also more short of breath.”
- “Here are the ECG recordings and dates.”
Bring patterns, not panic. A short timeline with symptoms and recordings is often more useful than a flood of screenshots.
What wearables cannot do
They cannot diagnose advanced heart failure on their own. They cannot tell you whether you need a transplant or a device. And they cannot replace urgent evaluation if you're having severe symptoms.
But they can help bridge a common gap in care. They can turn “I swear something changed” into “here is when it changed, how often it happened, and what my rhythm looked like when I felt it.”
For patients who feel dismissed or rushed, that can make conversations more grounded and less speculative.
Navigating Prognosis and Prioritizing Quality of Life
This is the hardest part to talk about, but honest information is kinder than vague reassurance.
Advanced heart failure is a serious condition. Half of patients diagnosed with this stage die within one year, and survivors often require multiple hospital admissions annually, according to population-based research on advanced heart failure outcomes. That's exactly why early identification, referral, and clear communication matter so much.
A serious prognosis does not mean there is nothing to do. It means every useful layer of support should be on the table.
What quality of life care really means
Many families hear palliative care and think it means giving up. It doesn't. Palliative care focuses on symptom relief, stress reduction, support with difficult decisions, and aligning treatment with what matters most to you.
That support can exist alongside active treatment. A person can still pursue specialist care, advanced therapies, or hospital treatment and also receive palliative support for breathlessness, fatigue, anxiety, sleep trouble, or caregiver strain.
Red flags that need urgent attention
Call your medical team promptly or seek urgent care if symptoms suddenly worsen, especially if you notice:
- Breathing that becomes much harder than usual
- New chest discomfort
- Confusion, fainting, or severe dizziness
- Rapid swelling or obvious fluid buildup
- A major change in your ability to function from one day to the next
The right time to ask for help is earlier than your fear tells you. Don't wait for symptoms to become unbearable just to avoid “bothering” someone.
Quality of life also includes practical conversations. Who should speak for you if you're too sick to decide? What tradeoffs feel acceptable to you? What kind of daily life are you hoping to preserve?
Those are not defeatist questions. They are wise ones.
Living with advanced heart failure means every heartbeat counts. Qaly turns your wearable ECG recordings into clear, human-reviewed reports.










.png)
.png)