Key Takeaways
That flutter gets your attention fast. You check your smartwatch, see an irregular rhythm alert, then remember your blood pressure has been running high. Now your mind starts connecting dots. Is this stress, a bad reading, or a real warning sign?
If that's where you are, your concern makes sense. Many people with palpitations feel stuck between too little information and too much alarm. You may also feel like you're expected to show up to a medical visit with perfect answers, even though you're the one trying to make sense of symptoms in real time.
Atrial fibrillation and hypertension are closely connected. High blood pressure can change how the heart is built and how its electrical system behaves. The good news is that home blood pressure readings and wearable ECGs can give you useful clues. They can't replace medical care, but they can help you notice patterns, ask sharper questions, and bring more than a vague memory to an appointment.
Your Guide to Heart Health
Hello Heart Hero. You might be reading this after a chest flutter that lasted a few seconds, a watch alert that made your stomach drop, or a week of blood pressure readings that seem harder to ignore.
A common moment goes like this. You stand up, walk across the room, and feel your heart start beating in a strange uneven way. You sit down, check your watch, and start scrolling for answers. If you've also been told you have high blood pressure, it's completely reasonable to wonder whether the two are related.
They often are.
High blood pressure usually doesn't create drama at first. Its onset is often subtle. Atrial fibrillation, or AFib, can feel much more obvious because it may show up as pounding, fluttering, racing, skipped beats, fatigue, lightheadedness, or a general sense that something isn't right.
Why this feels so unsettling
Part of the anxiety comes from not knowing what kind of problem you're dealing with. Some rhythm changes are brief and less dangerous. Others deserve prompt medical attention. That uncertainty can make every sensation feel bigger.
You are not overreacting by paying attention to your body. You're gathering information.
Many readers are also skeptical of the healthcare system, and that feeling doesn't come from nowhere. People with intermittent symptoms often hear, "Everything looked fine," especially if the episode stopped before testing happened. That's one reason patient-captured data matters.
What makes this guide useful
This article is built for the person holding two pieces of information at once:
- High blood pressure readings that may have been creeping up or staying high
- Irregular heartbeat alerts or palpitations that don't feel random anymore
You'll see how atrial fibrillation and hypertension connect, why the combination matters, and how to use your own recordings in a calm, practical way. The aim isn't to turn you into your own cardiologist. It's to help you become a clearer observer of your own health.
How High Blood Pressure Leads to Atrial Fibrillation
High blood pressure forces the heart to push against extra resistance. If that happens once, the heart can handle it. If it happens day after day, year after year, the heart starts adapting in ways that aren't always helpful.
Think of the upper chambers of the heart, called the atria, like flexible rooms that need to fill and empty smoothly. Constant high pressure changes those rooms. The tissue gets stretched, less springy, and more irritated. Electrical signals don't travel through damaged tissue as neatly as they do through healthy tissue.

The rubber band analogy
A fresh rubber band snaps back into shape easily. An old rubber band that's been stretched too many times becomes loose and unpredictable. Heart tissue under chronic pressure can behave in a similar way.
That change in shape and flexibility is part of what doctors call atrial remodeling. It means the atria are no longer the same structure they once were. Once the structure changes, the electrical system becomes more vulnerable to short circuits and chaotic signals.
What the research shows
Large studies have found that hypertension raises the risk of developing new AFib by 1.5- to 1.8-fold, and the ARIC study found that hypertension accounted for about 20% of new AFib cases according to this American Heart Association review on hypertension and atrial fibrillation.
That doesn't mean every person with high blood pressure will develop AFib. It does mean the relationship is strong enough that neither issue should be brushed off when they appear together.
Why the rhythm becomes irregular
In normal rhythm, electrical signals move through the atria in an organized pattern. In AFib, many signals fire in a disorganized way. Instead of one clean instruction, the atria receive competing messages.
Here is the simple chain:
- Pressure stays high and the heart works harder.
- Atrial tissue stretches and becomes less healthy.
- Electrical pathways become unstable.
- Irregular rhythm becomes easier to trigger and sustain.
Practical rule: If you have hypertension and new palpitations, don't assume they're unrelated just because the symptoms come and go.
Understanding the Mechanisms of Heart Remodeling
The heart doesn't just react to pressure. It remodels itself around it.
One important change happens in the main pumping chamber, the left ventricle. When it has to pump against high pressure for a long time, the muscle can thicken. This is called left ventricular hypertrophy. At first, that sounds like strength. In practice, a thicker heart muscle can become stiffer and less efficient.
How pressure backs up into the atria
When the left ventricle gets stiff, filling pressure rises. That pressure can back up into the left atrium. So even if your symptoms seem electrical, the setup often starts as a mechanical problem.
The atrium then stretches under that added strain. Stretch changes the tissue physically, and it also changes how electrical impulses move through it. That's one reason an echocardiogram can be so helpful. It can show chamber size, wall thickness, and other structural clues. If you want a plain-language overview of that test, this guide to a transthoracic echocardiogram is a useful starting point.
Fibrosis is the hidden troublemaker
Another major change is fibrosis. Think of fibrosis like patches of stiff scar-like material developing inside tissue that should stay flexible. Healthy electrical signals prefer smooth roads. Fibrosis creates potholes, detours, and dead ends.
That matters because AFib often thrives when signals start circling, colliding, or getting blocked.
A hormone system called the renin-angiotensin-aldosterone system, or RAAS, also plays a role here. When overactivated in hypertension, RAAS promotes inflammation and fibrosis, which can make the atria even more vulnerable.
Why this is more than theory
Research has linked sustained high blood pressure to left ventricular hypertrophy and atrial stretch, and a Mendelian randomization analysis found that a genetically determined 10 mmHg increase in blood pressure raised AFib odds by 90% in this hypertension and arrhythmia study.
That kind of finding helps answer a question many patients ask: "Is my blood pressure just associated with AFib, or does it help cause it?" The evidence supports a causal role.
- Mechanical strain: the heart muscle thickens and stiffens
- Pressure overload: the atria stretch
- Tissue change: fibrosis makes the atria less cooperative
- Electrical instability: abnormal rhythm becomes easier to start
Clinical Implications and Stroke Risk
People often think of AFib as a rhythm problem and hypertension as a pressure problem. In real life, they interact. That interaction is why clinicians take the combination seriously.
AFib can allow blood to pool in the atria instead of moving through in a smooth, coordinated way. Blood that sits still is more likely to clot. If a clot leaves the heart and travels to the brain, it can cause a stroke.

Why high blood pressure makes this more serious
High blood pressure can damage blood vessels over time. So when AFib and hypertension happen together, you don't just have one issue piled on top of another. You have two conditions that can increase the chance of a dangerous event.
For patients with atrial fibrillation, co-existing hypertension doubles stroke risk and is built into clinical tools such as CHA2DS2-VASc and HAS-BLED, which doctors use when weighing stroke and bleeding risk around anticoagulant treatment, as described in this review on hypertension in atrial fibrillation.
What those risk scores actually mean
These scores can sound cold and impersonal. They aren't meant to reduce you to a number. They are structured ways to make treatment decisions more consistent.
A doctor may use them to help decide:
- Whether blood thinners are appropriate
- How strongly to prioritize blood pressure control
- How to balance stroke prevention with bleeding concerns
If you've ever felt uneasy hearing that your treatment plan depends on a score, that's understandable. But the score is only one part of the conversation. Your symptoms, blood pressure history, age, other conditions, and actual heart rhythm recordings still matter.
A good appointment isn't just "Do I have AFib?" It's also "How does my blood pressure change what we do next?"
The practical takeaway for wearable users
If your watch flags an irregular rhythm and you also have hypertension, don't think only in terms of comfort. Think in terms of risk clarification.
Useful records to bring include:
- ECG strips from symptom moments
- Home blood pressure logs from the same day
- Notes about dizziness, breathlessness, or exercise intolerance
- Questions about clot prevention, including whether you need to discuss treatment options guided by resources like these atrial fibrillation anticoagulation guidelines
That kind of preparation turns a rushed visit into a more focused one.
Proactive Diagnosis with Your Smartwatch
Your smartwatch or handheld ECG device can do something very important. It can capture a rhythm while it's happening.
That matters because palpitations are often gone by the time you reach urgent care or a clinic. A symptom described from memory is helpful. A recording captured in the moment is better.
What to record when symptoms happen
Start with the basics. If you feel fluttering, pounding, skipped beats, or an odd wave of weakness, try to capture both rhythm and context.
Write down:
- What you felt such as fluttering, racing, thumping, or chest unease
- What you were doing like resting, walking, climbing stairs, or standing up
- What your blood pressure was, if you can measure it safely
- How long it lasted
- Whether your watch labeled it as AFib, irregular rhythm, high heart rate, or something else
This turns random events into a pattern log.
What people often get confused about
Many consumers look at a single-lead ECG and expect it to be obvious. Sometimes it is. Sometimes it isn't. AFib often appears as an irregularly irregular rhythm without clear repeating P waves, but wearable tracings can also be noisy, brief, or hard to interpret.
So don't put pressure on yourself to diagnose your own strip. A better goal is to capture good-quality recordings and pair them with blood pressure readings and symptom notes.
A practical Apple Watch overview is available in this article on whether Apple Watch can detect AFib.
Don't ignore posture-related clues
One overlooked pattern is symptoms that happen when you stand up. Orthostatic hypotension, which is a sudden drop in blood pressure after standing, has been linked to increased future AFib risk according to this American Heart Association page on high blood pressure, AFib, and stroke risk.
That doesn't mean every dizzy spell is AFib. It does mean posture changes belong in your notes.
If your symptoms tend to happen after standing, bending, showering, or getting out of bed, write that down. Timing can be as useful as the ECG itself.
A calm way to use your device
Use your watch as a notebook, not a judge.
Try this approach:
- Capture the rhythm
- Take a blood pressure reading when appropriate
- Log the trigger or situation
- Save the recording for review
- Share the cluster of information, not just one screenshot
That gives your clinician a clearer picture than a single alert ever could.
Your Management Plan for AFib and Hypertension
If you have both atrial fibrillation and hypertension, the center of the plan is simple. Control the blood pressure consistently. Not perfectly for one day. Consistently over time.
That matters because the heart responds to blood pressure burden, meaning the severity and duration of high pressure. Studies show AFib risk rises by 8% to 71% depending on the level of hypertension burden over time in this American Heart Association analysis of blood pressure burden and incident AF.
What treatment usually tries to do
Doctors generally think about AFib management in a few lanes at once.
- Pressure control first: lower the ongoing strain that keeps feeding the problem.
- Rate control: slow the heartbeat so the heart can work more efficiently, even if AFib is still present.
- Rhythm control: try to restore or maintain normal rhythm when that approach fits the person and situation.
- Stroke prevention: decide whether clot prevention treatment is needed.
Some medicines overlap. For example, a medication used for blood pressure may also help with heart rate. Other medicines target rhythm more directly. The right mix depends on your full history, not just one watch strip.
What you can do at home
You don't need to wait passively between appointments. You can build a home routine that makes treatment decisions easier.
Consider these habits:
- Use a reliable upper-arm blood pressure monitor and take readings in a consistent way
- Keep a simple symptom diary rather than relying on memory
- Bring trends, not isolated numbers, to your appointment
- Ask what the treatment target is for you, so you're not guessing what counts as controlled
- Review your care team communication, because atrial fibrillation and hypertension often involve primary care, cardiology, pharmacy, and sometimes electrophysiology
Questions worth asking your clinician
Instead of asking only "Is this serious?", try more specific questions:
- Do my BP readings suggest enough burden to worsen rhythm problems?
- Are my symptoms more consistent with short AFib episodes or another arrhythmia?
- Should I focus on rate control, rhythm control, or both right now?
- What BP pattern do you want me to track at home?
For a practical overview of measuring and logging home readings, this guide on blood pressure tracking can help you organize what to bring.
How Human-Reviewed ECGs Empower Your Care
Raw data can calm you or confuse you. Most of the time, it does both.
A smartwatch tracing may show an irregular rhythm, but many people don't know whether they're looking at AFib, motion artifact, a few ectopic beats, or a poor recording. That's where reviewed interpretation becomes useful. Instead of trying to decode every squiggle yourself, you can turn a wearable ECG into something more understandable and shareable.

Why reviewed data changes the conversation
A human-reviewed ECG report can help in two ways.
First, it reduces some of the panic that comes from staring at a recording alone. Second, it gives you a more credible summary to bring into care. That matters if you've ever felt dismissed for describing symptoms that were gone by the time anyone checked.
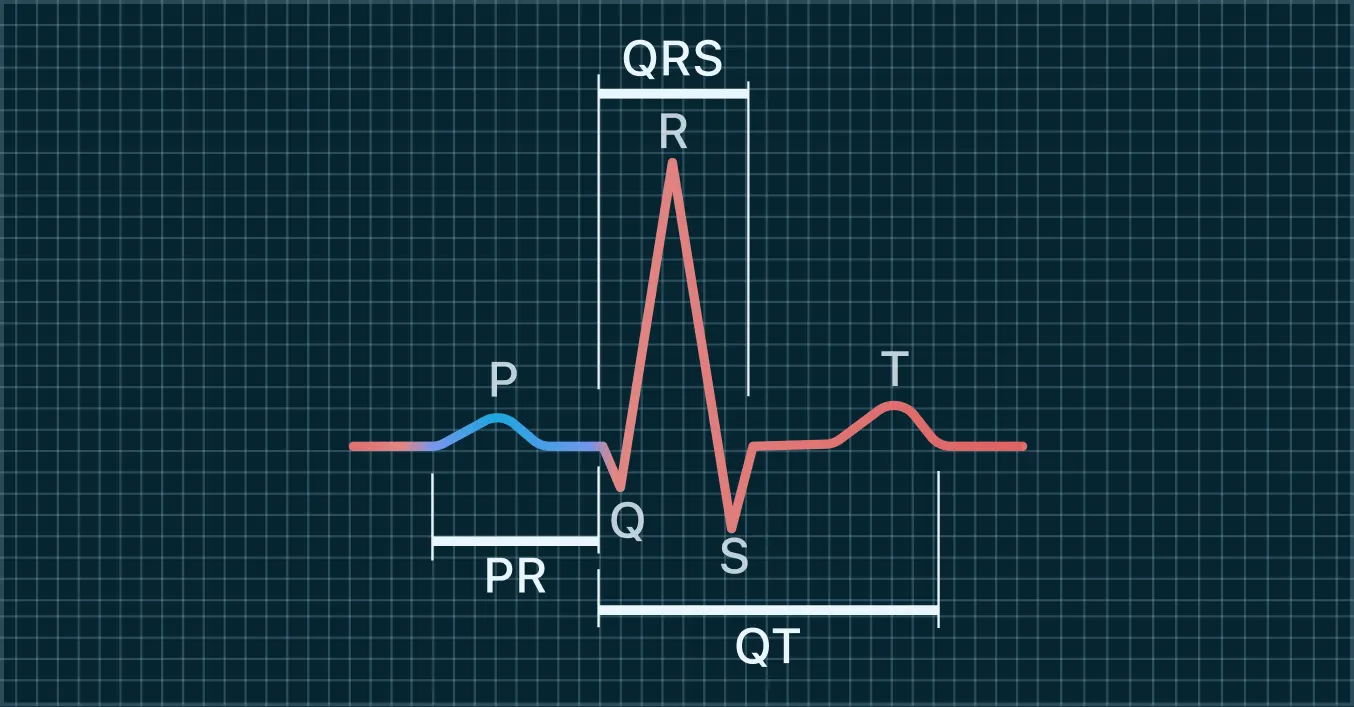
Qaly is one option for this. It reviews wearable ECGs from devices like Apple Watch, Fitbit, Kardia, and others, and provides interpretation of findings such as rhythm patterns and intervals including PR, QRS, and QTc. Used this way, it becomes less about self-diagnosis and more about building better evidence for discussion with your clinician.
What this looks like in practice
Instead of saying, "My watch scared me last Tuesday," you can show:
- The ECG strip
- The time symptoms started
- Your blood pressure around the event
- A reviewed summary of what the tracing showed
Better data doesn't replace medical judgment. It helps you bring something concrete into the room.
That shift can be powerful, especially for anxious wearable users. You stop being just the person with a vague story and become the person with organized observations.
Wondering if it's Atrial Fibrillation? On the Qaly app, human experts will interpret your ECGs for Atrial Fibrillation within minutes. Get started today.











.png)
.png)