Key Takeaways
Hello Heart Hero.
You may be here because a doctor mentioned rheumatic heart disease, or because your watch flagged an irregular rhythm and you started searching for answers late at night. That kind of uncertainty can feel heavy. A lot of people hear the term and think it sounds old-fashioned, confusing, or far away from modern life.
What matters most right now is this. Rheumatic heart disease is serious, but it is understandable. And once you understand it, the condition becomes much less mysterious.
Your Guide to Understanding Rheumatic Heart Disease
Rheumatic heart disease happens when the heart valves are damaged after an immune reaction called acute rheumatic fever. That immune reaction can follow an untreated group A strep throat infection.
Many people get confused because the problem starts in the throat but ends up in the heart. That sounds strange at first. A simple way to think about it is this: your immune system is trying to fight off one problem, but in some people it mistakenly irritates healthy tissues too, including parts of the heart.
Some people learn about this diagnosis after years of subtle symptoms. Others only hear about it when a clinician notices a murmur, shortness of breath, or signs of an irregular heartbeat. If that happened to you, you're not behind. Rheumatic heart disease often develops without prominent early symptoms.
Why this topic still matters
In many high-income settings, people assume rheumatic heart disease disappeared. It hasn't. It may be less common there, but it still shows up in people whose earlier infections weren't recognized or fully treated, especially in communities facing barriers to care.
That matters if you use a smartwatch, Kardia device, or another wearable ECG tool. Those devices can't tell you whether a valve is scarred, but they can help you notice the rhythm problems that sometimes develop when the valves are under strain.
Rheumatic heart disease is not just a historical diagnosis. For some people, it's a present-day explanation for palpitations, fatigue, breathlessness, or pregnancy-related heart symptoms.
What to keep in mind right away
- It starts with a treatable infection: The chain begins with strep throat, not with a mysterious heart problem.
- It affects valves: The damage is mechanical. The "doors" inside the heart may become stiff or leaky.
- It can be monitored: Doctors use echocardiograms to see the valve damage and ECGs to look at rhythm effects.
- You can take action: Prevention, follow-up, and symptom tracking all matter.
How Rheumatic Heart Disease Begins
A sore throat doesn't usually make people think about heart disease. That's one reason rheumatic heart disease is so easy to misunderstand.
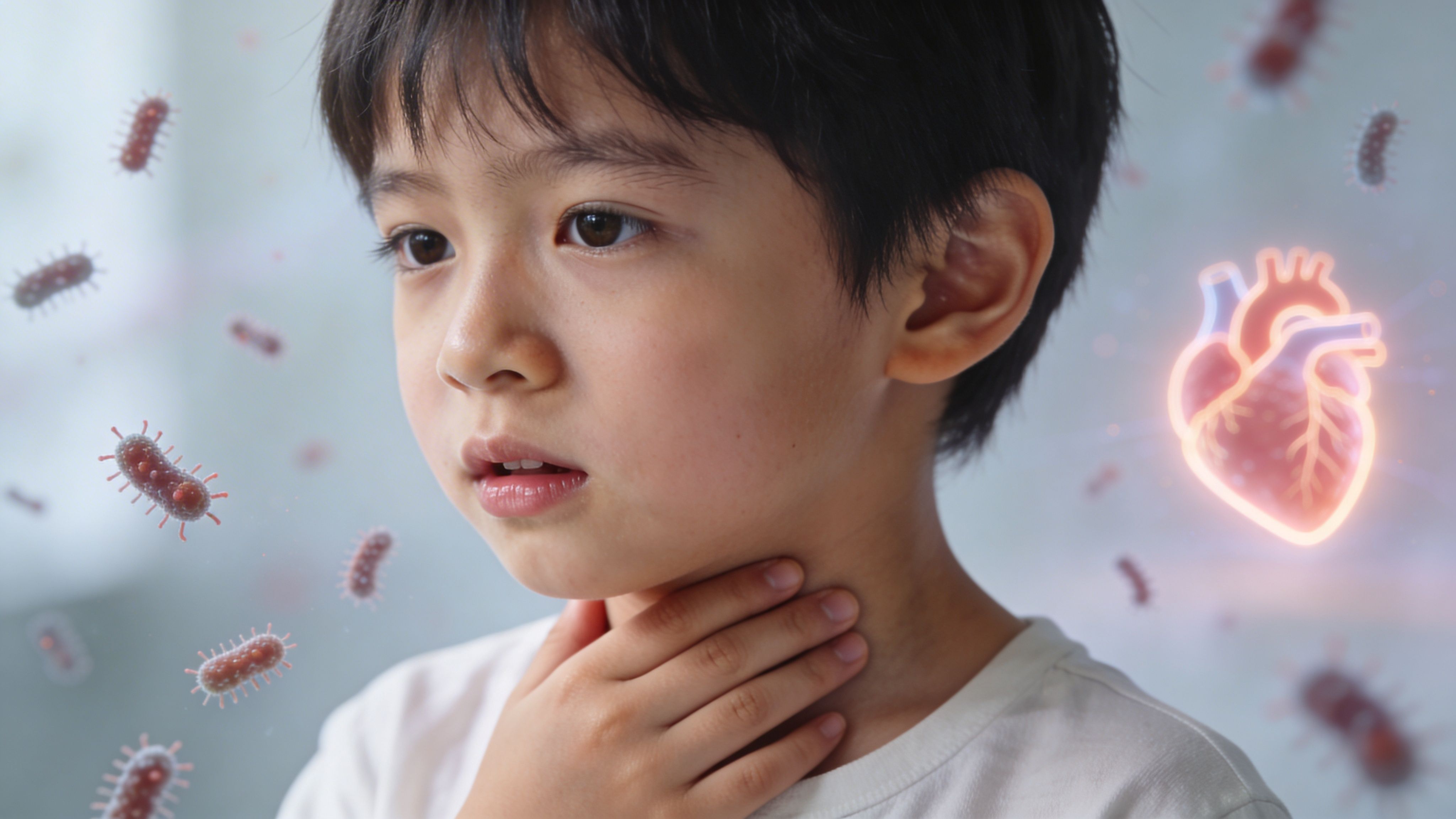
The chain reaction
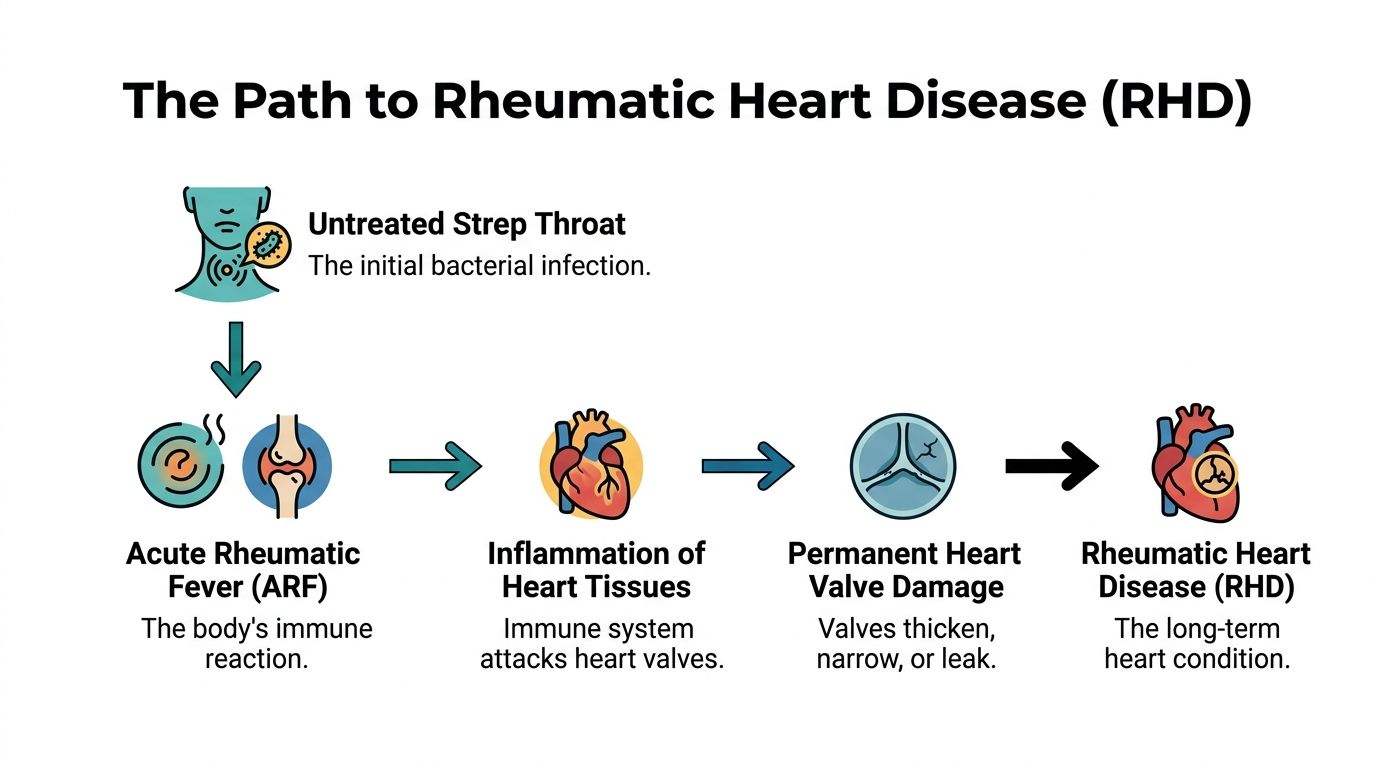
It often unfolds in a sequence:
- A person gets strep throat
Group A Streptococcus causes the throat infection. - The infection isn't treated promptly
Not every sore throat is strep, and not every strep infection leads to heart trouble. But untreated strep creates the risk. - The immune system overreacts
In some people, the body's defense system begins attacking healthy tissues by mistake. - Acute rheumatic fever develops
This is the inflammatory illness that can affect joints, skin, brain, and heart. - The valves become scarred over time
That long-term valve injury is rheumatic heart disease.
Why prevention matters so much
Rheumatic heart disease affects an estimated 33.4 million people worldwide, with a huge gap between settings. The incidence is 3.4 cases per 100,000 people in non-endemic countries versus 444 cases per 100,000 in endemic regions like Oceania and central sub-Saharan Africa. It is also described as the leading cause of cardiovascular death in children and young adults in low-resource settings (NCBI Bookshelf overview of rheumatic heart disease burden).
Those numbers tell a human story. People don't develop this condition because they did something wrong. It often reflects gaps in access to early diagnosis, antibiotics, and follow-up care.
A useful mental model
Think of the immune system as a home security system. Its job is to detect an intruder and respond fast. In acute rheumatic fever, the alarm system doesn't shut off cleanly. It keeps firing and starts damaging the house itself.
That same idea helps people understand why heart inflammation can follow a throat infection.
If you've also come across other heart inflammation terms online, it can help to compare them carefully. For example, myocarditis affects the heart muscle, while rheumatic heart disease mainly leaves its mark on the heart valves.
Practical rule: Treating suspected strep throat early can prevent a long chain of later problems. That's why clinicians take recurrent sore throats seriously in high-risk settings.
The Way RHD Damages Heart Valves
Rheumatic heart disease leaves its longest-lasting mark on the heart valves. These are the thin flaps that keep blood moving in the right direction with each heartbeat.
How valve injury happens
Your heart valves work like one-way doors. They should swing open easily, then close firmly so blood does not wash backward.
After rheumatic inflammation, those doors can lose their shape. The valve leaflets may become thick, scarred, or partly stuck together. Over time, that creates two main problems:
- Stenosis: the valve becomes stiff or narrow, so blood has trouble getting through
- Regurgitation: the valve does not seal well, so some blood leaks backward
A worn door with a swollen frame helps as a mental picture. It may scrape when it opens and fail to shut cleanly. A damaged valve creates the same kind of mechanical problem inside the heart, except the heart has to deal with it all day, every day.
Which valve is usually involved
The mitral valve is affected most often in rheumatic heart disease, according to a review in StatPearls on rheumatic heart disease. This valve sits between the left upper chamber and the left lower chamber, where smooth one-way flow matters a lot.
If the mitral valve leaks, part of the blood moves in reverse. If it narrows, blood has to squeeze through a tighter opening. In both cases, the heart spends more effort to do the same job.
If a scan report mentions a leak, this plain-language guide to mild valve regurgitation can make that wording easier to understand.
What doctors look for on an echo
An echocardiogram lets clinicians watch the valve move in real time. They are looking at both function and structure. Does blood move backward in an abnormal way? Do the valve leaflets look thickened, restricted, or distorted?
That matters because rheumatic valve disease is not diagnosed from symptoms alone. The diagnosis depends on seeing a pattern of valve damage that fits with prior rheumatic injury.
For people at higher risk, or for anyone with a history that raises concern, early cardiovascular screening can help catch valve problems before they cause major strain.
Why this matters for symptoms and rhythm changes
A damaged valve changes the pressure and flow pattern inside the heart. Chambers can stretch. Pressure can back up toward the lungs. The electrical system may also become more irritable, which helps explain why some people later develop palpitations or arrhythmias.
This is one reason wearable ECG devices can be useful in the bigger picture. They do not diagnose valve disease, but they can help you capture rhythm symptoms that sometimes appear after valve damage has been present for a while.
That combination matters for a tech-savvy patient. An echocardiogram shows the plumbing. A wearable ECG can help track the wiring.
Recognizing Symptoms and Getting Diagnosed
Some people with rheumatic heart disease feel unwell early. Others don't notice anything until the valve damage has been there for years.

What you might feel
Symptoms can be vague at first. That's frustrating, especially if you've been told "everything seems fine" while your body feels different.
Common experiences include:
- Shortness of breath: Especially during walking, climbing stairs, or lying flat
- Fatigue: A drained feeling that's hard to explain
- Palpitations: Fluttering, pounding, skipping, or racing beats
- Chest discomfort: Not always severe, but worth noting
- Swelling: Sometimes in the legs or ankles if the heart is under strain
Pregnancy can also bring hidden valve problems to the surface because the heart has to handle more blood flow during that time.
What the clinician is looking for
A doctor may first suspect valve disease by hearing a murmur through a stethoscope. A murmur is the sound of turbulent blood flow. It isn't a diagnosis by itself, but it often prompts more testing.
The test that answers the main question is an ultrasound of the heart. If you're unfamiliar with that process, a transthoracic echocardiogram is the standard scan used to look at valve structure and blood flow.
Where wearable ECGs fit in
A wearable ECG can't diagnose valve scarring directly. It doesn't show the valve leaflets opening and closing. But it can detect the electrical effects of strain on the heart.
One of the most important rhythm complications is atrial fibrillation, which occurs in over 30% of patients with RHD because the upper heart chambers stretch over time. On an at-home ECG, a PR interval over 200 ms or QTc prolongation over 460 ms can be warning signs that deserve discussion with a doctor (journal overview of rhythm findings and interval clues in RHD).
That means your Apple Watch, Fitbit ECG feature, KardiaMobile, or similar device can be useful for spotting patterns such as:
- irregular rhythm episodes
- recurring palpitations at the same time of day
- changes after exertion
- interval changes if your reports include PR or QTc values
If your wearable repeatedly shows an irregular rhythm, that's not proof of rheumatic heart disease. It is a reason to bring the tracing to a clinician and ask whether valve disease or another heart issue should be ruled out.
Your Path to Treatment and Prevention
A diagnosis of rheumatic heart disease can stir up fear quickly. Many people hear "heart valve damage" and assume life will immediately become narrow or fragile. That's not the whole picture.
The condition is serious, but there are effective ways to reduce further injury and manage the damage already there.
Protecting the heart from repeat attacks
One of the most important ideas is secondary prophylaxis. That means ongoing treatment to prevent another episode of acute rheumatic fever, because another inflammatory attack can worsen valve damage.
For many patients, that means regular benzathine penicillin G injections given periodically. You can think of this as a shield. It doesn't erase the scar tissue already present, but it helps protect the valve from being hit again.
For skeptical patients, this can feel repetitive or burdensome. That's understandable. But this part of treatment is prevention with a very specific purpose.
Treating the effects of valve disease
Treatment depends on which valve is affected, whether the problem is mainly narrowing or leaking, and how much strain the heart is under.
A care plan may include:
- Medicines for fluid buildup: These can ease breathlessness and swelling.
- Rhythm management: If atrial fibrillation develops, your team may address rate control, rhythm control, or stroke prevention.
- Regular imaging: Repeat echocardiograms help doctors see whether the valve is stable or worsening.
- Procedures or surgery: Some people need repair or replacement when symptoms or heart strain become significant.
Why follow-up matters even when you feel okay
Rheumatic heart disease doesn't always announce itself loudly. People can feel stable while the valve slowly changes. That is why scheduled follow-up is not just bureaucracy. It's how clinicians catch the moment when a treatment shift can protect heart function.
It can help to bring a simple log to appointments:
- Your symptoms: breathlessness, fatigue, swelling, dizziness
- Your triggers: exercise, illness, pregnancy, stress
- Your rhythm notes: palpitations, irregular rhythm alerts, episode timing
Treatment works best when you and your clinician can see the pattern, not just one snapshot from one visit.
A hopeful way to frame it
Rheumatic heart disease management is not about waiting for something bad to happen. It's about reducing avoidable strain, preventing further damage, and stepping in before the heart gets overwhelmed.
That mindset often lowers anxiety. You don't need perfect control. You need steady partnership, clear follow-up, and a plan that makes sense to you.
Living Well and Monitoring Your Heart with Wearables
You feel a sudden flutter while walking to the kitchen. Your smartwatch pings. For a moment, the hardest part is not the sensation itself. It is the question that follows. Is this harmless, or is my heart asking for attention?
For people living with rheumatic heart disease, that uncertainty can wear you down. The valve problem may be structural, but one of the most stressful day-to-day effects is often electrical. Palpitations, skipped beats, or an irregular pulse can leave you guessing between appointments. A wearable ECG cannot diagnose a damaged valve, but it can help you catch rhythm changes that deserve a closer look.
Why rhythm tracking matters so much
Rheumatic heart disease remains a major global cause of illness and early death, especially in places where diagnosis and follow-up are delayed, as described in this JAMA study of global outcomes in adults with rheumatic heart disease. That broader public health reality matters on a personal level too. Many patients live for years with symptoms that come and go, and rhythm problems may be one of the first changes they can notice at home.
That is where wearables can be useful in a very practical way. They give you a chance to document what your body is doing in real time instead of trying to remember a brief episode days later in clinic.
What to watch for on your device
A helpful way to frame this is simple. Your echocardiogram is the camera that shows the valve. Your wearable ECG is the notebook that records the heart's electrical behavior.
Look for patterns such as:
- An irregular rhythm: This can raise concern for atrial fibrillation or another rhythm problem.
- Episodes that keep coming back: A repeat pattern usually matters more than a single odd reading.
- Symptoms that match the tracing: Dizziness, breathlessness, chest discomfort, or a pounding heartbeat during an abnormal recording deserve extra attention.
- A change from your usual baseline: New alerts, longer episodes, or more frequent recordings can all be worth discussing.
If you want a clearer sense of what your watch can and cannot show, this cardiologist's guide to the smartwatch ECG explains the basics in patient-friendly terms.
A calm routine is more useful than constant checking
People often assume more data always means more clarity. In real life, random checking can increase anxiety and produce a pile of recordings with no context.
A steadier routine works better:
- Record when symptoms happen: Take a tracing during fluttering, racing, pounding, or a strange pause.
- Add one sentence of context: Were you resting, climbing stairs, sick, dehydrated, stressed, or using caffeine?
- Save recordings in one place: A simple folder or note on your phone makes follow-up easier.
- Track frequency, not just screenshots: Clinicians often learn more from when episodes happen and how often they recur than from one isolated strip.
Your wearable works best as a witness, not a judge. It helps document the moment so you and your clinician can interpret it together.
Using the device without letting it run your day
There is a balance to aim for. Ignoring every symptom can delay care. Checking your pulse every few minutes can make normal body sensations feel frightening.
A wearable can help you find the middle ground. You notice a symptom, capture a recording, jot down the setting, and move on. Over time, that creates a clearer story. For a tech-savvy patient with rheumatic heart disease, that story can turn vague worry into something more useful. A pattern you can share, discuss, and act on with your care team.
When to Seek Care and Your Key Takeaways
You don't need to rush to emergency care for every skipped beat. But some symptoms should never be brushed aside.
Seek urgent medical care if you have
- Severe shortness of breath: Especially if it comes on suddenly or makes speaking difficult
- Chest pain: Particularly if it's intense, persistent, or paired with nausea, sweating, or breathlessness
- Fainting or near fainting: This can signal a dangerous rhythm or severe valve-related strain
- Rapid swelling or sudden weakness: Especially if it appears with breathing trouble or palpitations
- A new irregular rhythm with severe symptoms: If your device shows an abnormal rhythm and you feel unwell, get assessed promptly
Arrange a routine appointment if you notice
- More frequent palpitations
- A drop in exercise tolerance
- New fatigue that doesn't fit your usual baseline
- Breathlessness when lying down or climbing stairs
- Repeat wearable alerts even when you feel mostly okay
The clearest takeaways
Rheumatic heart disease begins with a throat infection that can trigger an immune reaction in vulnerable people. The lasting problem is valve damage. That damage can stay quiet for years, then show up as breathlessness, fatigue, or rhythm problems.
An echocardiogram confirms the valve problem. A wearable ECG doesn't diagnose the valve itself, but it can help you catch arrhythmias and track changes worth discussing with your care team.
Most important, you are not powerless here. If you're proactive, organized, and willing to seek care when patterns change, you're already doing something meaningful for your heart.
If your smartwatch or at-home ECG is picking up palpitations, irregular rhythm alerts, or tracings you don't understand, Qaly can help you get fast human-reviewed ECG interpretation from certified cardiographic technicians. It's a practical way to turn confusing wearable data into something you can understand and share with your doctor.
Confused by your wearable ECG? Get fast, expert interpretation from Qaly.










.png)
.png)