Key Takeaways
Hello Heart Hero. If you're reading this because your watch showed a pause, your pulse suddenly felt slow, or your heart keeps switching between calm and chaotic, your concern is reasonable. Many people notice something real in their body long before they get a clear explanation.
You may also be tired of hearing vague reassurance when what you want is a straight answer. A strange heartbeat can be unsettling, especially when symptoms come and go and your clinic ECG happens to look normal that day.
sa node dysfunction sits right in that frustrating gap. It can be subtle, intermittent, and confusing. But it can also be understood. And if you use a smartwatch or wearable ECG, you already have a tool that can help you gather useful evidence and have a better conversation with your doctor.
Your Guide to Understanding an Irregular Heartbeat
A common story goes like this. You feel a flutter while folding laundry, then a heavy pause, then a wave of lightheadedness. You check your watch. It shows a low heart rate, or maybe an odd tracing you don't understand. Later, when you feel fine again, you wonder if you imagined it.
You didn't.
Heart rhythm symptoms often arrive in short bursts. That makes them easy to miss in a clinic and easy for other people to minimize. If you've felt brushed off, that frustration makes sense. Your lived experience matters, especially with conditions that don't follow a convenient schedule. SA node dysfunction involves the heart's natural pacemaker. When that pacing system misfires, the result may be a rhythm that is too slow, pauses at the wrong time, or swings between slow and fast. Some people notice fatigue. Others notice dizziness, skipped beats, or sudden weakness. For some, the first scary clue is fainting.
Why patients often feel confused
The symptoms can overlap with stress, dehydration, medication effects, poor sleep, thyroid problems, or other rhythm conditions. That's why people often end up asking, "Is this dangerous, or just annoying?"
The honest answer is that it depends on the pattern, the symptoms, and the context.
Your watch doesn't replace a doctor. But it can capture the moment your body is trying to tell you something.
That matters because wearable ECGs can help connect sensation to rhythm. When you pair symptom notes with ECG recordings, you're no longer walking into an appointment with only a vague memory. You're bringing clues.
What this means for you
You don't need to become an electrophysiologist. You just need a workable mental model:
- Your heart has a built-in starter. That starter is the SA node.
- Sometimes it slows too much. That can leave you tired, foggy, or dizzy.
- Sometimes it pauses or becomes erratic. That can feel abrupt and frightening.
- Not every case is permanent. Age matters, but medications and other reversible factors can matter too.
That's a much more useful starting point than "my heart feels weird."
What Is SA Node Dysfunction
Think of your heart like a band. The SA node, short for sinoatrial node, is the drummer. It sets the tempo so the rest of the group can stay together. Every beat starts with that signal.
When the drummer keeps steady time, blood moves efficiently. When the beat slows too much, drops out, or becomes inconsistent, the whole performance feels off. That's sa node dysfunction, also called sick sinus syndrome.
What can go wrong
This condition isn't one single rhythm problem. It's a family of related problems involving the heart's natural pacemaker.
- Sinus bradycardia: The SA node fires too slowly.
- Sinus pause or sinus arrest: The SA node seems to stop firing for a stretch of time.
- Bradycardia-tachycardia pattern: The rhythm alternates between too slow and too fast.
- Chronotropic incompetence: The heart doesn't speed up appropriately when your body needs it to, such as during walking or climbing stairs.
If you've ever thought, "My resting heart rate is low, but sometimes my heart suddenly races," that combination can fit under the same umbrella.
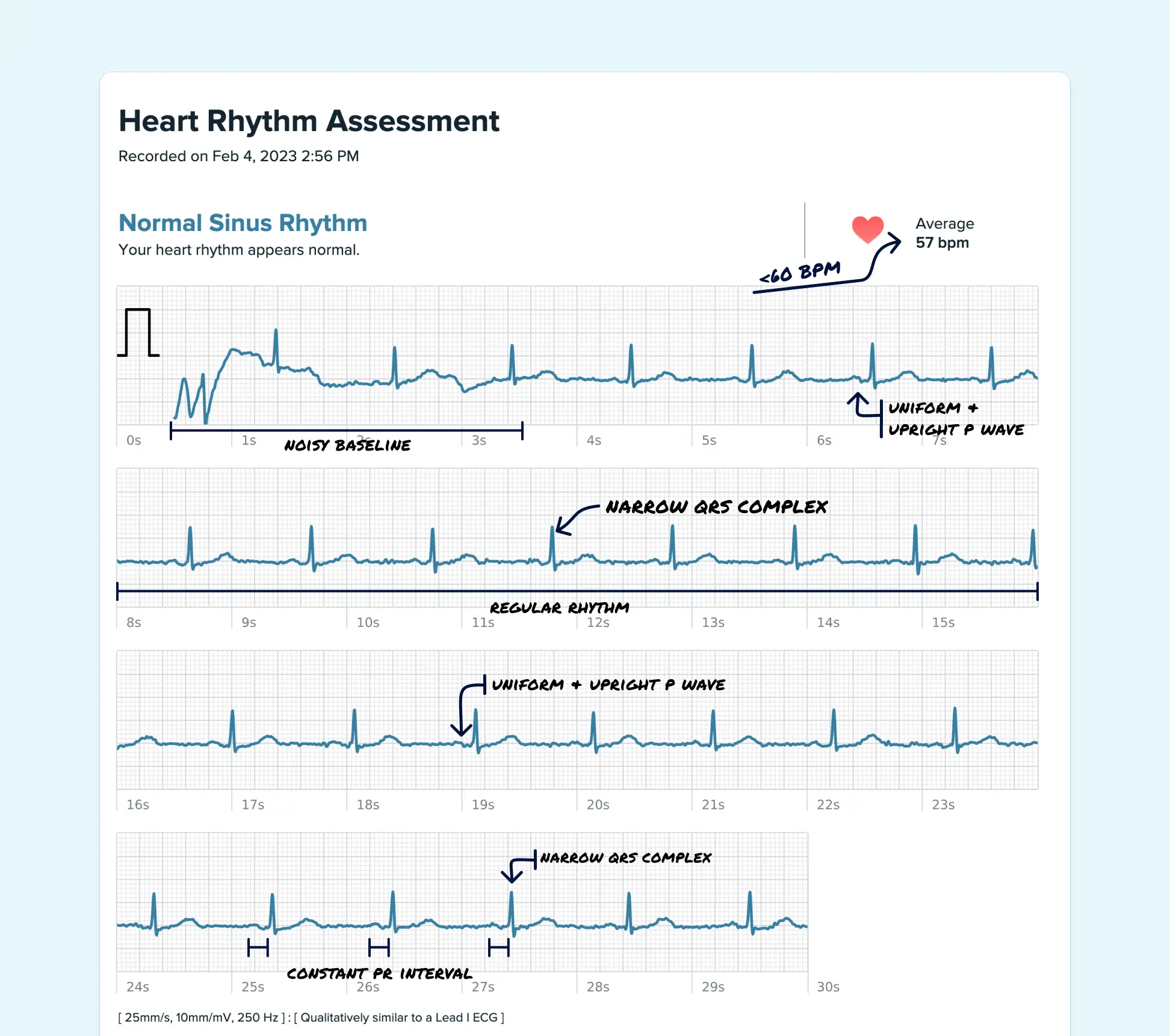
Why the SA node becomes unreliable
At the cell level, the SA node depends on a coordinated timing system. One part comes from ion channels in the cell membrane, often called the membrane clock. Another part comes from calcium moving inside the cells, called the Ca2+ clock. When those systems stop syncing well, the pacemaker can slow down or shift. That disruption can happen with fibrosis or other electrical remodeling, as described in this review on sinus node biology and dysfunction: SA node membrane clock and Ca2+ clock interplay.
You don't need to memorize the chemistry. The practical point is simpler. The SA node isn't just a wire. It's living tissue with delicate timing. If that timing system is disturbed, the rhythm can become unreliable.
Practical rule: A strange heartbeat isn't always a problem with the whole heart muscle. Sometimes the issue is the timing system that tells the heart when to beat.
Why this feels so different from person to person
One person may notice only reduced stamina. Another may have dramatic palpitations. A third may faint without warning. That's because the same underlying node can malfunction in different ways.
It also helps explain why wearable tracings can be confusing. A single watch ECG may show only one slice of the story. The larger pattern over time often matters more than one isolated recording.
Common Causes and Risk Factors
A common story goes like this. Your watch starts showing heart rates in the 40s. You mention it at an appointment and hear, "That can happen with age." Sometimes that is true. Sometimes it is only part of the picture.
Age is one of the strongest risk factors for sinus node dysfunction. The condition becomes more common in older adults, especially as the tissue around the SA node develops fibrosis, or microscopic scarring, that interferes with the heart's timing signals. The American Heart Association explains that sinus node dysfunction is usually related to age-dependent progressive fibrosis of the sinus nodal tissue and nearby atrial muscle in its overview of bradycardia and cardiac conduction delay.
The simplest way to picture it is this. A healthy SA node works like a reliable conductor keeping an orchestra on tempo. With age, the conductor may still be present, but the cues can become less steady and the surrounding players may respond less cleanly. That can lead to slower heart rates, pauses, or an uneven handoff of electrical signals.
Age, though, is only one lane in the road.
A slower rhythm can also come from medications, other medical conditions, or underlying heart disease. That distinction matters because age-related change is usually gradual, while medication effects or metabolic problems may appear after a clear trigger and may improve when the trigger is corrected.
Causes your doctor will usually sort into a few groups
Age-related fibrosis and electrical change:
This is the classic pattern. The node and nearby atrial tissue become less dependable over time, which raises the chance of bradycardia, pauses, or alternating slow and fast rhythms.
Medication effects:
Beta-blockers, some calcium channel blockers, digoxin, and certain antiarrhythmic drugs can slow the sinus node. If your symptoms began after a dose increase or a new prescription, that timing is worth bringing up clearly.
Other heart conditions:
Coronary artery disease, prior heart surgery, atrial fibrillation, or other structural heart problems can affect how the sinus node fires or how the signal travels.
Systemic or reversible contributors:
Sleep apnea, thyroid disease, electrolyte problems, infection, and low oxygen states can all contribute to a slow or unstable rhythm.
If you are trying to make sense of low pulse alerts or brief pauses on a device, this guide on what causes bradycardia gives a useful overview of the possibilities clinicians review.
How wearable data can help, and where it can mislead
Wearables are often most useful when they show a pattern, not a single strange reading. A one-time low heart rate during sleep may mean very little. Repeated daytime bradycardia with fatigue, lightheadedness, or exercise intolerance gives your doctor a much more meaningful clue.
Try to collect context with the tracing or alert:
- What time did it happen?
- Were you asleep, resting, walking, or exercising?
- Did it start after a medication change?
- Did you feel symptoms, or did the device flag it without symptoms?
- Is this a repeated pattern over days or weeks?
That kind of record helps separate three questions that often get blurred together. Is this a normal age-related slowing? Is this a medication effect? Or is this a rhythm problem that needs closer evaluation?
Questions that can make an appointment more productive
If you feel brushed off, bring specifics instead of only the label you are worried about. A few focused questions can shift the conversation:
- Could my medications be contributing to these readings or symptoms?
- Do my wearable ECGs suggest sinus node dysfunction, or only sinus bradycardia?
- Are there reversible causes that should be checked before this is called age-related?
- Do the episodes happen in a pattern that makes them more concerning?
- Would formal monitoring help confirm what my wearable is picking up?
That approach gives your clinician something concrete to interpret. It also gives you a clearer path if the first explanation feels too simple.
Recognizing the Signs and Symptoms of SND
The symptoms often seem disconnected until you know what ties them together. A pause in the heart rhythm can briefly reduce blood flow to the brain. That can feel like dizziness, dimming vision, or a sudden need to sit down.
A very slow rhythm can leave you drained in a quieter way. You may notice unusual fatigue, reduced exercise tolerance, brain fog, or the sense that your body isn't keeping up with basic activity.
The symptoms people describe most often
The most alarming symptom is syncope, or fainting. It occurs in up to 50% of patients with sinus node dysfunction. Another 50% of patients experience bradycardia-tachycardia syndrome, where the heart alternates between slow and fast rhythms, as outlined by the American Academy of Family Physicians in this clinical review of sinus node dysfunction.
That fast-slow switching helps explain why the condition can feel contradictory. One day your watch flags a low rate. Another day your chest feels like it's fluttering or pounding.
How it can feel in everyday life
Some people say it feels like:
- A dropped beat followed by a thud
- A slow, heavy pulse when they stand up
- Sudden weakness while walking or climbing stairs
- A burst of racing beats after a quiet pause
If you've looked at your watch tracing and wondered what normal slow rhythm looks like compared with something more concerning, this article on what sinus bradycardia looks like on your watch ECG can help you build pattern recognition.
A symptom diary is often more useful than memory. Write down what you felt, what you were doing, and whether your wearable captured the moment.
When symptoms deserve faster attention
Seek urgent medical care if you have fainting with injury, chest pain, severe shortness of breath, or a rhythm problem that leaves you feeling unstable. Even if the cause turns out not to be sa node dysfunction, those symptoms need prompt evaluation.
The key point is this. Your symptoms are data. They are not a nuisance, and they are not separate from the ECG story. When the feeling and the tracing line up, diagnosis gets much easier.
How SA Node Dysfunction Is Diagnosed Today
Diagnosing sa node dysfunction can be tricky because the rhythm problem may not be happening when you're sitting in a clinic chair. A standard ECG is useful, but it's just a snapshot. If your symptoms happen twice a week, at night, or only after medication, a snapshot may miss the event entirely.
That's why modern diagnosis often depends on matching symptoms, timing, and rhythm evidence over days or weeks.
Traditional tools still matter
Doctors may use:
- Office ECGs: Good for persistent abnormalities, not as good for rare episodes.
- Holter monitors: Helpful when symptoms happen often over a day or two.
- Longer event monitoring: Better for rhythms that come and go.
- Medication review and exam: Essential, especially when a drug may be slowing the node.
If you're comparing the role of a watch ECG with longer monitoring, this overview of a cardiac monitor and Holter helps clarify how these tools complement each other.
Where wearable ECGs change the game
Wearables like Apple Watch, Kardia, Fitbit, Samsung, and Withings can capture an event when you feel it. That's their big advantage. They travel with you.
If you feel dizzy at 8:14 p.m. and record an ECG at 8:15 p.m., you've captured something a clinic never could have planned for. That is powerful.
Still, single-lead wearable ECGs have limits. A pause on a tracing doesn't always mean the same thing. One of the most confusing examples is the difference between sinus arrest and SA exit block. Both can look like missing activity on a single-lead recording, but the underlying problem is different.
A 2024 study on wearable ECGs estimated that 15% of readings labeled as a "sinus pause" were likely misclassified SA exit block, which matters because single-lead devices can't reliably distinguish the two on their own. Human-reviewed trend analysis can help reduce anxiety and misdiagnosis, as discussed in this source: wearable ECG pause misclassification and SA exit block.
What to bring your doctor
The most useful wearable evidence is organized, not overwhelming.
Bring:
- The ECG strip itself
- The time and date
- What you felt
- What you were doing
- Your medication list, including recent changes
A report that tracks interval trends and recurring patterns can be especially helpful. One option some wearable users choose is Qaly, which provides human-reviewed analysis of at-home and wearable ECGs, including interval measurements and narrative reports that can be shared with clinicians.
The goal isn't to prove your doctor wrong. It's to give your doctor cleaner evidence.
A smarter way to think about diagnosis
A diagnosis isn't just "the watch said pause." It's a reasoning process.
Your clinician is asking:
- Is the rhythm abnormal?
- Does it match the symptom?
- Could medication or another reversible issue explain it?
- Is the pattern intermittent or progressive?
- Does it suggest monitoring, medication change, or pacemaker discussion?
When you arrive with precise recordings and symptom context, you move that process forward faster. That can mean less uncertainty and fewer assumptions.
Treatment Options and Lifestyle Considerations
You may arrive at this stage with a watch alert, a few scary symptoms, and one big question. Is this a problem to monitor, a medication effect to fix, or a rhythm issue that needs a device?
That distinction shapes treatment.
Some people improve after a careful review of medications that can slow the sinus node, such as certain beta blockers, calcium channel blockers, or antiarrhythmic drugs. In other cases, the pattern reflects age-related change in the heart's natural pacemaker. A smaller group has persistent sinus node dysfunction that causes clear symptoms and leads to a pacemaker discussion.
Start with what can be changed
The SA node works like the heart's timekeeper. If a medicine is pressing too hard on that timekeeper, the rhythm may slow even when the node itself is not permanently damaged. That is why your medication list, including recent dose changes, matters so much.
Daily habits can help make the picture clearer too. Good hydration, regular sleep, and limiting substances that trigger palpitations or worsen lightheadedness can reduce extra noise around the rhythm. These steps do not repair intrinsic SA node dysfunction, but they can help you and your clinician tell the difference between a temporary stressor and a more consistent pacing problem.
Wearable data can be very useful here. A cluster of slow-rate alerts right after a medication increase tells a different story than repeated pauses that happen across many days with the same symptoms.
When a pacemaker enters the conversation
Permanent pacemakers are commonly used for symptomatic sinus node dysfunction. The key word is symptomatic. Doctors are usually looking for a match between what the ECG shows and what you feel, such as dizziness, near-fainting, unusual fatigue, or exercise intolerance.
A pacemaker works like a backup metronome. If your own sinus node keeps good time, the device may do very little. If your rate drops too low or pauses become unreliable, it steps in to keep the rhythm from falling behind.
For many patients, that means more steadiness and less fear. If the idea feels abstract, this plain-language guide to heart pacemaker operation can help you picture what the device does and what treatment involves.
.webp)
Lifestyle still matters after the treatment decision
Even with a clear diagnosis, daily tracking has value. Wearables can help you notice whether symptoms improve after a medication change, whether episodes still happen during sleep, or whether your energy is better after pacemaker placement. Used this way, your device becomes part of follow-up care, not just a source of alarms.
That same habit can also support broader monitoring cardiovascular health, especially if rhythm symptoms are happening alongside blood pressure changes, poor exercise tolerance, or recovery issues.
Red flags that should never wait
Get urgent help if you have:
- Fainting with injury
- Chest pain
- Severe shortness of breath
- A rhythm problem with marked weakness or confusion
Treatment should match the cause. Age-related slowing, a medication side effect, and true sinus node failure can look similar at first, but they are managed differently.
Clear records help your doctor sort that out faster. That matters most for people who have felt dismissed, because a short symptom diary plus well-timed ECG strips often makes the next step much easier to choose.
Taking Charge of Your Heart Rhythm Health
A strange heartbeat can make you feel powerless. Good information changes that. Once you understand that sa node dysfunction can range from medication-related slowing to a more persistent pacing problem, your next steps become clearer.
Start with observation. Save the ECGs that match symptoms. Write brief notes about dizziness, fluttering, fatigue, or near-fainting. Keep track of medication changes. Those details may look small, but they can change the whole interpretation.
Build a useful record, not a giant folder
Try to collect:
- Symptom-linked ECGs
- A short timeline of when episodes happen
- Recent medication changes
- Questions you want answered at your visit
That kind of record supports better conversations about diagnosis, monitoring, and treatment. It also helps if you're interested in broader habits for monitoring cardiovascular health over time, especially if you're using wearables as part of your daily routine.
Trust your body and bring evidence
You are the person who feels the symptom first. That's not a small thing. When you combine that lived experience with recordings from your own device, you become a much stronger partner in your care.
If you've felt unheard before, let the data support your story. Calm, organized evidence often gets better traction than trying to describe a fleeting sensation from memory alone.
If you want help making sense of watch or at-home ECG recordings before your next appointment, Qaly offers human-reviewed ECG interpretation for wearable devices so you can track rhythm patterns and share clearer information with your healthcare team.
Wondering what your ECG means? Track your rhythm. Share your data. Get answers faster with Qaly.









.png)
.png)